Converging Innovation, A Promising Gastric Future
Converging Innovation, A Promising Gastric Future
—Our hospital's Department of Gastric Surgery has independently and successfully performed laparoscopic proximal gastrectomy with GIRAFFE reconstruction for the first time.
To date, issues such as the extent of lymph node dissection, surgical approach selection, resection range, and digestive tract reconstruction methods for adenocarcinoma of the esophagogastric junction (AEG) have remained hotly debated topics in the field of digestive surgery, with postoperative digestive tract reconstruction following proximal gastrectomy being a particularly contentious focus. In recent years, the surgical team led by Director Nie Peng from the Department of Gastric Surgery at Wuwei Cancer Hospital in Gansu Province has long been dedicated to exploring optimal post-proximal gastrectomy digestive tract reconstruction methods. Their research has spanned from esophagogastrostomy (anterior/posterior wall) ± pyloroplasty, to interposed jejunal anastomosis and double-tract anastomosis, and further to the double-flap technique (Kamikawa anastomosis). They have found that each reconstruction method has its own advantages and disadvantages, and there is still no universally recognized ideal reconstruction approach.

Recently, the surgical team led by Director Nie Peng from our hospital's Department of Gastric Surgery has once again successfully and independently performed a new reconstruction method after proximal gastrectomy—the GIRAFFE reconstruction. This procedure was developed by the team of Professor Cheng Xiangdong from the Cancer Hospital affiliated with the University of Chinese Academy of Sciences. It is based on the concept of interposed tubular stomach and reconstructed gastric fundus with His angle to prevent reflux, featuring low complication rates and effective anti-reflux properties. This technique can be performed either through open surgery or laparoscopy, provided there is extensive long-term experience with various digestive tract reconstruction methods. Currently, this technology has only been implemented at its development institution, where 100 cases have demonstrated favorable outcomes. There have been no related reports from other domestic institutions or within Gansu Province. Therefore, the successful completion and routine implementation of this reconstruction method at our center will provide another entirely new option for gastric cancer patients in the region and also marks a new milestone in the surgical diagnostic and treatment capabilities of our hospital's laparoscopic gastric cancer team in the Department of Gastric Surgery.
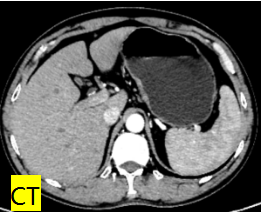
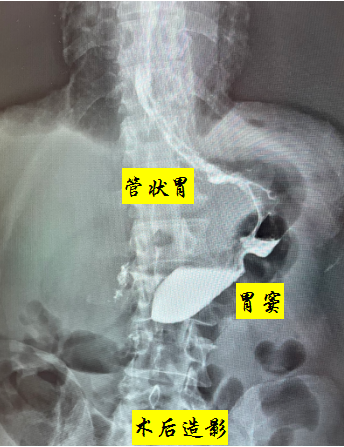
A 64-year-old patient surnamed Wang was diagnosed with gastric cancer (cT2NxM0) four months ago at a hospital in Lanzhou. Due to comorbidities including emphysema, grade 3 hypertension, hepatitis B, and a history of cerebral hemorrhage, along with long-term anticoagulant medication use, he had relative contraindications for surgery. He was therefore given two cycles of SOX regimen neoadjuvant chemotherapy while his comorbidities were actively managed. After the two chemotherapy cycles, a follow-up gastroscopy showed lesions at the cardia of undetermined nature (post-chemotherapy changes). Pathological examination confirmed well-differentiated adenocarcinoma of the cardia, and CT scans revealed localized slight thickening of the lesser curvature of the gastric wall at the cardia with an intact serosal surface. The patient’s condition improved further after neoadjuvant therapy, with localized lesions and no lymph node or distant metastases, making surgery the preferred treatment. However, considering his advanced age and multiple comorbidities, to minimize perioperative complications while ensuring R0 resection of the tumor, the surgical team thoroughly discussed the short- and long-term outcomes and risks of various procedures with the family before ultimately deciding on proximal gastrectomy. Among the available reconstruction methods for proximal gastrectomy—such as interposed jejunal, double-tract, or direct esophagogastrostomy—all carry relatively high risks of postoperative complications like reflux esophagitis. While the Kamikawa anastomosis can reduce reflux esophagitis and lower the risk of anastomotic leakage, it is technically complex and time-consuming. Given the patient’s multiple underlying conditions, prolonged surgery might not be well tolerated. Research indicates that the GIRAFFE reconstruction is relatively simple, minimizes operative time, and provides excellent anti-reflux effects. Led by Director Nie Peng, the laparoscopic gastric cancer team at the hospital’s Gastroenterology Surgery Department closely followed international advancements in gastric cancer treatment, conducted in-depth research, and actively applied clinical practices. After thorough preoperative preparation, they successfully performed a laparoscopic proximal gastrectomy with esophagogastrostomy using the GIRAFFE reconstruction for this patient, achieving excellent surgical outcomes.
Director Nie Peng explained that the GIRAFFE reconstruction offers several advantages:
1. Preserves normal physiological pathways, facilitating postoperative endoscopic examinations of the remnant stomach and duodenum.
2. Retains the distal stomach, which not only stores food but also mechanically grinds food particles through peristalsis, mixing them with gastric juice before propelling chyme into the duodenum.
3. Maintains gastric pacemaker cells located in the middle greater curvature of the stomach (5–7 cm from the cardia), ensuring good postoperative gastric emptying.
4. Provides superior anti-reflux effects: The reconstructed gastric fundus blocks some refluxed gastric contents. The increased pressure in the artificial fundus then compresses the distal tubular stomach through the reconstructed His angle, reducing the amount of refluxed contents entering the tubular stomach. The interposed tubular stomach between the esophagus and remnant stomach acts as a buffer zone, reducing gastric reflux toward the esophagus.
5. The free tubular stomach effectively resolves anastomotic tension issues.
Thus, this reconstruction method is technically simple, safe, feasible, and highly effective.
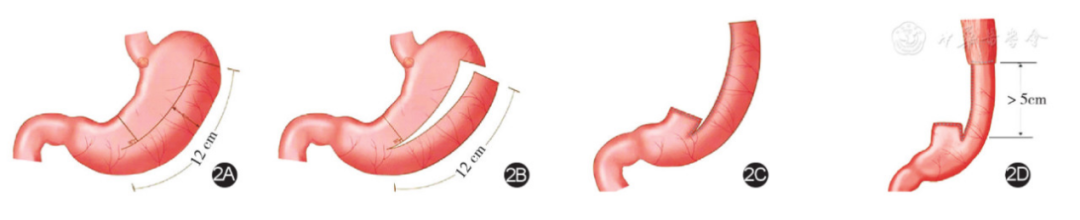
Currently, the GIRAFFE reconstruction is suitable for patients with clinical stage cT1-3N0M0 upper third gastric body cancers or Siemert II/III type adenocarcinoma of the esophagogastric junction (AEG) who are candidates for proximal gastrectomy. Recent studies have demonstrated that this procedure offers advantages such as simplified surgical technique, broad indications, tension-free anastomosis, and a reliable anti-reflux mechanism. These benefits are expected to significantly advance the further innovation of surgical approaches for upper gastric cancers or esophagogastric junction tumors, ultimately delivering greater benefits to patients.
Expert Profiles

Nie Peng
Chief Physician
Master of Surgery. Bachelor's degree from Lanzhou University Medical College in 2001, Master's degree from Qinghai University Medical College in 2010. Chief Physician of Oncological Surgery at Wuwei Academy of Medical Sciences & Tumor Hospital, Assistant to the President, Party Branch Secretary of Digestive Diseases Hospital, Director of General Surgery Department, and Director of Gastric Surgery Department. Deputy Director of Gansu Anti-Cancer Association Gastric Cancer Professional Committee, Standing Committee Member of Gansu Geriatric Medical Association Gastric Cancer Professional Committee, Director of Wuwei Medical Association General Practice Professional Committee, and Deputy Director of Wuwei Medical Association Oncology Professional Committee.
With over 20 years of surgical experience, he has completed advanced training at Peking University Cancer Hospital, Zhongshan Hospital affiliated with Fudan University (Shanghai), Tumor Hospital affiliated with Guangzhou Medical University, Tumor Hospital affiliated with Tianjin Medical University, Xijing Hospital affiliated with Fourth Military Medical University, and Lanzhou General Hospital of Lanzhou Military Command. Through continuous dedicated research and comprehensive integration, he has achieved exceptional expertise in the diagnosis and treatment of digestive tract diseases, particularly specializing in gastric disease management and minimally invasive surgical treatments for various gastric conditions.
In recent years, he has participated in one national natural science research project, led one provincial health commission research project, five Wuwei municipal research projects, and is currently leading one provincial natural science foundation project. He has published over 10 academic papers, including nine in national core journals.
Specializing in comprehensive treatment and minimally invasive surgery for various gastric diseases, he has personally performed over 3,000 surgical procedures, including more than 2,000 radical gastrectomies for gastric cancer.
Scope of Practice: Gastric Surgery, Oncological Surgery
Clinic Location: Room 201, Outpatient Department, Digestive Diseases Hospital Campus
Clinic Hours: Every Monday, Wednesday, and Friday (all day)
Registration Methods: Online appointment via official website or on-site registration
Contact Number: 0935-6988091
