Summary of Efficacy Analysis of Heavy (Carbon) Ion Therapy for Sarcoma in 164 Cases Abstract
Summary of Efficacy Analysis of Heavy (Carbon) Ion Therapy for Sarcoma in 164 Cases
Abstract
This study summarizes the clinical data of 164 sarcoma patients treated with heavy (carbon) ion therapy at the Wuwei Heavy Ion Center from November 2018 to March 2026. Heavy (carbon) ion therapy demonstrated high efficacy against various types of sarcomas (including multiple rare and refractory types), achieving an extremely high local control rate. In this cohort, the mean survival time during the average follow-up period was (36.99 ± 2.58) months, with a four-year survival rate of 67.25% for osteosarcoma patients. These findings indicate that heavy (carbon) ion therapy is safe and effective for treating various sarcomas, highlighting its unique value for sarcomas in complex locations, those that are surgically unresectable, or those that have failed conventional treatment.
I. Introduction: Advantages of Heavy (Carbon) Ion Therapy for Sarcomas
Sarcomas are a group of rare malignant tumors originating from mesenchymal tissue, encompassing various types such as bone, muscle, fat, and blood vessels. Traditional treatment primarily relies on surgical resection, supplemented by radiotherapy, chemotherapy, as well as targeted and immunotherapies. However, for sarcomas located in critical sites, those that are inoperable, or those insensitive to conventional photon radiotherapy, treatment options are limited and outcomes remain poor.
Heavy (carbon) ion therapy, as an advanced radiotherapy technique, offers unique physical (Bragg peak) and biological (high relative biological effectiveness, RBE) advantages. It enables precise delivery of a high radiation dose to the tumor target while maximally sparing surrounding normal tissues. It is sensitive against various sarcomas and is particularly suitable for cases adjacent to critical organs, those with prior radiotherapy, or those resistant to conventional radiotherapy.
II. Basic Information of the Patient
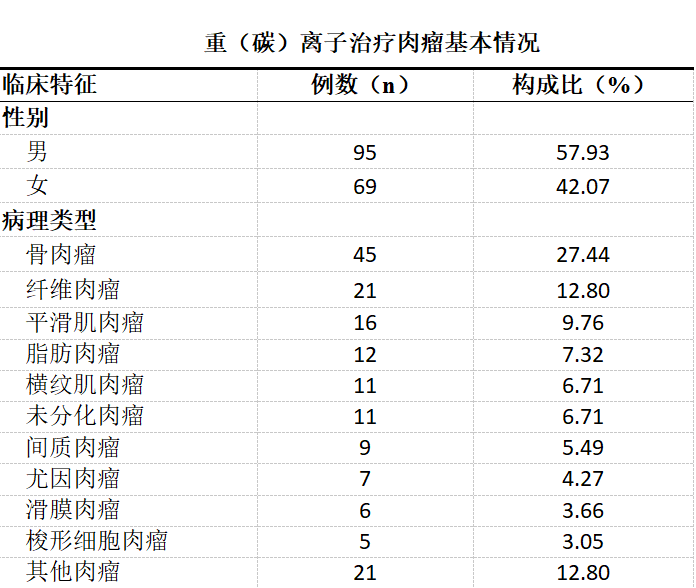
Our center performed the first heavy (carbon) ion therapy in November 2018, and has treated a total of 164 sarcoma patients. Among them, there were 95 males and 69 females, with a mean age of (44.82 ± 18.54) years (range: 12 to 92 years). The cohort included 45 cases of osteosarcoma, 21 cases of fibrosarcoma, 16 cases of leiomyosarcoma, 12 cases of liposarcoma, 11 cases of rhabdomyosarcoma, and 21 cases of other sarcomas.
Demographic characteristics: 95 males and 69 females; mean age (44.82 ± 18.54) years (range: 12 to 92 years).
The pathological types were diverse, including osteosarcoma (45 cases), fibrosarcoma (21 cases), chondrosarcoma (14 cases), leiomyosarcoma (16 cases), as well as various subtypes such as synovial sarcoma, rhabdomyosarcoma, and liposarcoma, covering almost all clinically rare sarcoma types.
Regarding case special features: this cohort included 5 cases of radiation-induced secondary tumors (sarcomas) and 3 cases of cardiac sarcoma. Notably, the use of heavy (carbon) ion therapy for cardiac sarcoma was a world-first, made possible by the center's director, Dr. Zhang Yanshan, whose previous experience in cardiac surgery provided him with a profound understanding of cardiac anatomy.
III. Survival Status and Efficacy Conclusions
Core conclusion: Heavy (carbon) ion therapy achieved a local control rate of nearly 100% and an efficacy rate of 100% for sarcomas.
In this cohort of 164 patients, after treatment with heavy (carbon) ion therapy, all evaluable lesions were effectively controlled, achieving an extremely high local control rate. This provides a revolutionary local treatment modality for addressing the challenges of primary sarcomas, postoperative recurrence, residual disease, or inoperable cases.
Overall and Subgroup Survival Data:
Overall survival: Among the 164 patients, the mean survival time was (36.99 ± 2.58) months, with 1-year, 2-year, 3-year, and 4-year survival rates of 75.60%, 67.00%, 57.79%, and 51.00%, respectively.
Osteosarcoma: The 45 patients had a mean survival time of (48.33 ± 3.78) months, with a 4-year survival rate of 88.89%.
Chondrosarcoma: The 14 patients had a mean survival time of (28.93 ± 5.18) months, with a 3-year survival rate of 73.18%.
Fibrosarcoma: The 21 patients had a mean survival time of (23.20 ± 4.38) months, with a 3-year survival rate of 46.02%.
Leiomyosarcoma: The 16 patients had a median survival time of (17.00 ± 4.55) months, with a 2-year survival rate of 68.57%.
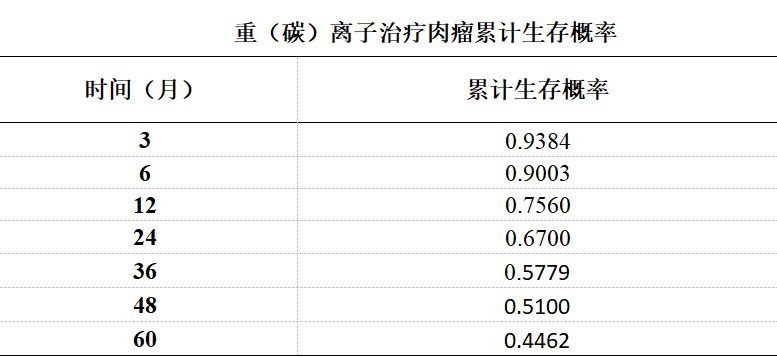
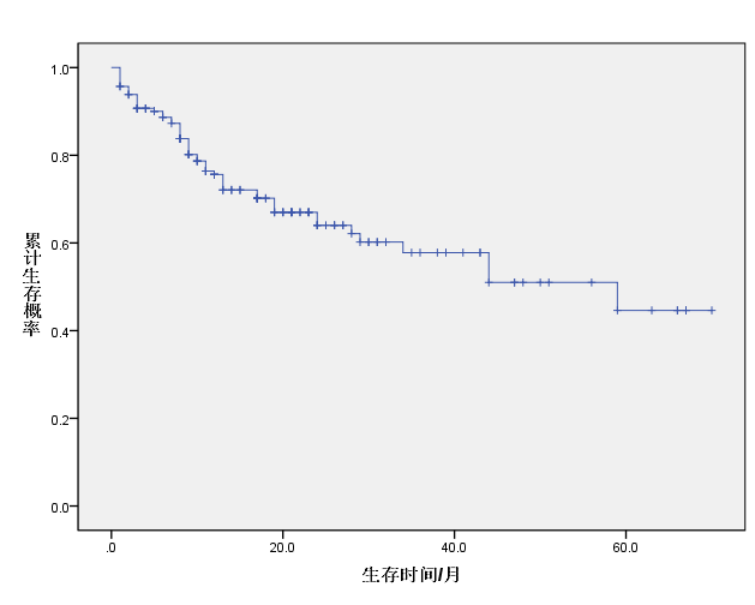
Survival curve from the end of treatment to 60 months after the end of treatment
IV. Display of Typical Cases
Case 1: Bai XX, female, 14 years old, Jinchang, Gansu. Diagnosis: Right femoral osteosarcoma cT2N0M0 IIB, KPS: 70. The patient did not undergo surgery and received heavy (carbon) ion therapy directly, along with 6 cycles of concurrent chemotherapy, with no other treatment. At 66 months after heavy (carbon) ion therapy, she has achieved complete recovery.
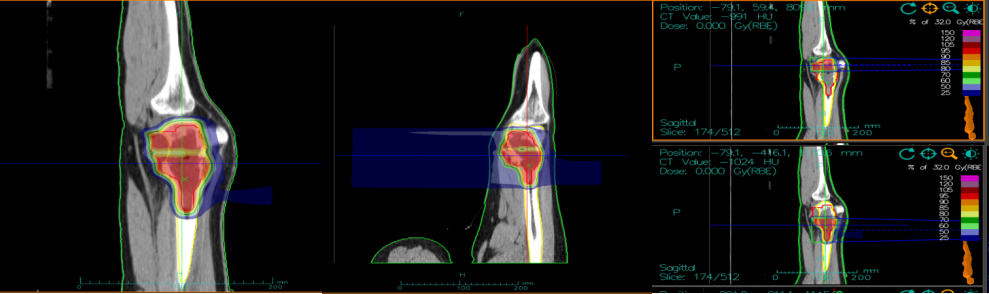
Pre-treatment heavy ion plan shows an osteosarcoma of 130mm in size at the lower end of the femur
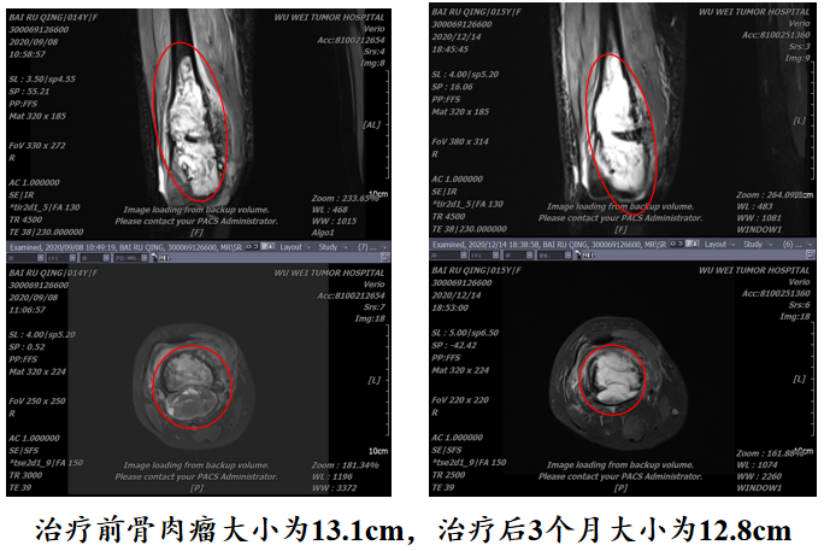
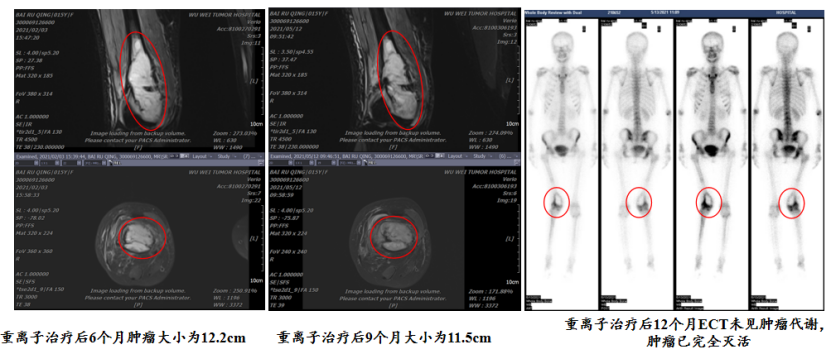
Currently, 66 months after heavy (carbon) ion therapy, the patient has fully recovered
Case provided by: Dr. Yang Yuling
Department: Radiation Oncology Center Ⅰ(International Medical Department Ⅰ)
Case 2: Patient, female, 55 years old. Medical history: Right calf liposarcoma, with two wide excision surgeries performed on November 17, 2014, and March 30, 2016. After the second surgery, she received adjuvant radiotherapy in May 2016 (total dose 50.4 Gy/28 fractions, followed by a boost of 10 Gy/5 fractions). On November 1, 2018, PET-CT and MRI (Figure 1) showed tumor recurrence, with a lesion located in the interval space between the right tibia and fibula, measuring approximately 4.2 × 2.0 cm. The clinical diagnosis was recurrent right calf liposarcoma. In November 2018, the patient received heavy (carbon) ion therapy with the following regimen: total dose 64 Gy (RBE) in 16 fractions, delivered over 28 days (Monday through Friday, once daily), with a two-field irradiation plan (horizontal field and vertical field, see Figure 2).
Efficacy: The tumor significantly shrank after treatment. Partial remission (PR) was achieved 60 days after treatment, with the tumor diameter reducing from 42 mm to 22 mm. Complete remission (CR) was achieved 120 days after treatment, with the tumor disappearing completely (Figure 4). MRI at 270 days after treatment (Figure 5) showed no signs of recurrence. Adverse effects: Only grade 1 radiation dermatitis (mild erythema and dry desquamation, see Figure 3) occurred 30 days after treatment, and no grade ≥2 acute toxicities were observed.
Figure 1. Imaging examination before treatment
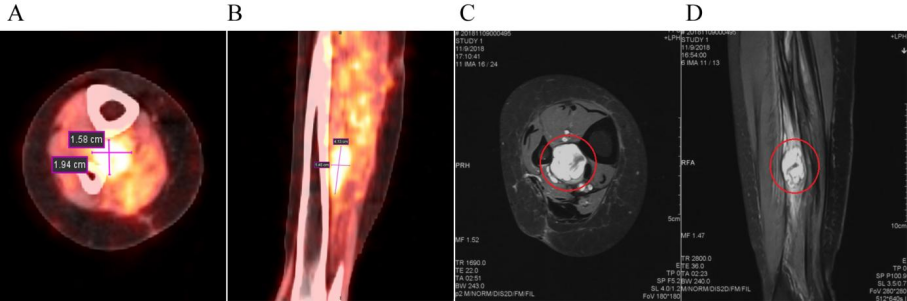
(A) PET/CT axial image: shows a lesion with high SUV uptake. (B) PET/CT sagittal image: T2WI shows high signal intensity. (C) MRI axial image and (D) MRI sagittal image
Figure 2. Design of irradiation fields for heavy (carbon) ion therapy
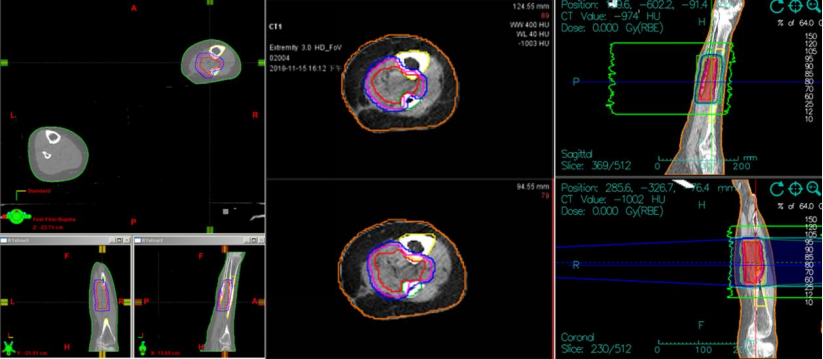
(Schematic diagram showing a two-field irradiation plan with horizontal and vertical fields)
Figure 3. Adverse reactions after treatment
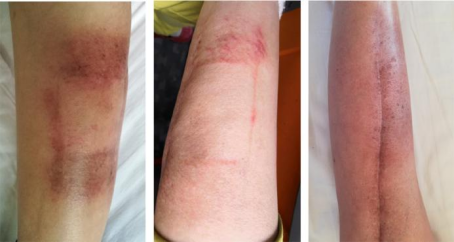
(Showing grade 1 radiation dermatitis in the treated area of the right calf 30 days after treatment, presenting as mild erythema and dry desquamation.)
Figure 4. Comparison of images before and after treatment
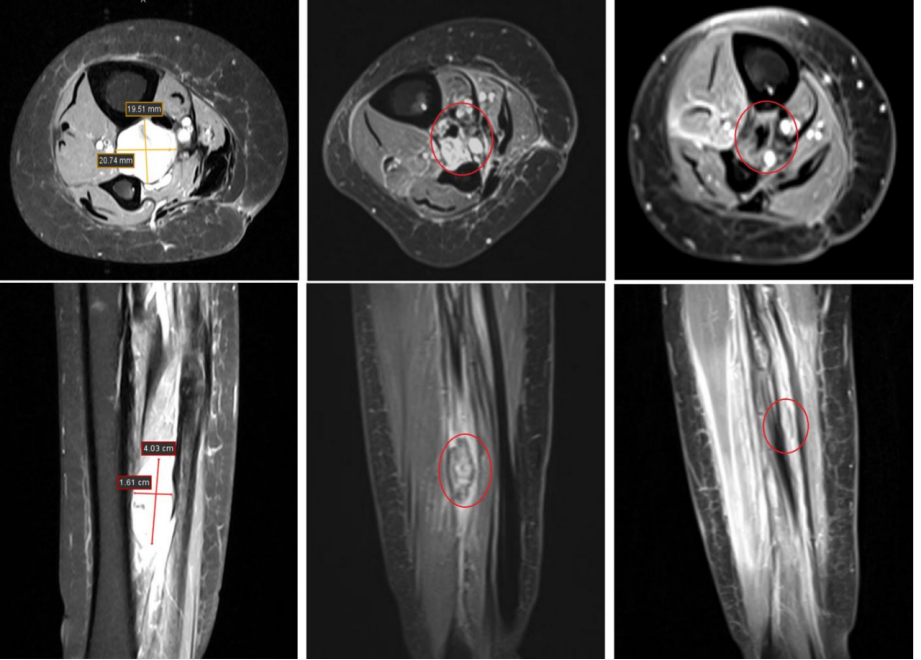
(Compare the imaging changes before treatment, 60 days after treatment (PR), and 120 days after treatment (CR).)
Figure 5. MRI follow-up at 270 days after treatment
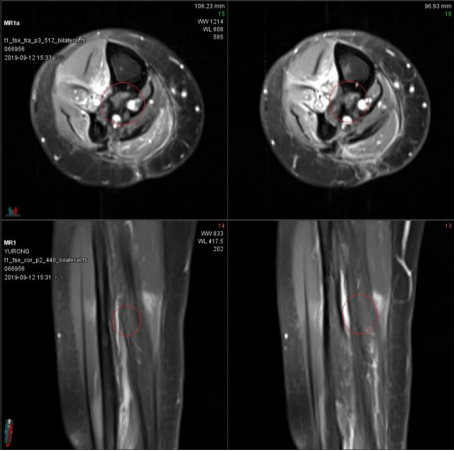
(Shows the MRI image 270 days after treatment, which displays no abnormal signals in the original tumor area, confirming a complete remission.)
Case 3: Li XX, female, 51 years old, from Qinghai. Chief complaint: Diagnosed with uterine leiomyosarcoma for over 8 years, with chest pain and cough for 12 days. Admission diagnosis: Secondary malignant neoplasm of the lung, malignant neoplasm of the uterus (leiomyosarcoma). The patient underwent total hysterectomy for "uterine fibroids" in May 2015, and postoperative pathology confirmed "uterine leiomyosarcoma." Subsequently, she experienced a long and complex treatment course, with the specific timeline as follows:
2015: Received postoperative adjuvant chemotherapy (doxorubicin + cyclophosphamide) for 4 cycles.
2016–2017: Switched to traditional Chinese medicine for management due to intolerance to chemotherapy.
2017–2022: Received targeted therapy with anlotinib hydrochloride, with efficacy evaluation showing partial remission (PR).
2022: PET-CT indicated new metastases in the right lower lobe of the lung and pancreas. Subsequently, various treatments including envafolimab, albumin-bound paclitaxel combined with cadonilimab, and others were attempted, all with poor efficacy (PD).
July 2022: Underwent biopsy at China-Japan Friendship Hospital, confirming that the right lung mass was a metastasis from uterine leiomyosarcoma. Genetic testing revealed a splicing mutation in the MED12 gene.
2023: Received treatment with cadonilimab combined with anlotinib, during which she developed shortness of breath and hemoptysis, leading to discontinuation of anlotinib at the end of the year.
January 2024: The patient experienced worsening chest pain, shortness of breath, and cough, and was unable to lie flat or ambulate. After receiving symptomatic treatment at West China Hospital, she was advised to undergo palliative supportive care. To seek further diagnosis and treatment, she was transferred to our center by recreational vehicle. Upon admission, chest CT revealed space-occupying lesions in the right hilum and right lung, measuring approximately 60 mm × 70 mm. Ultrasound-guided lung biopsy was performed, and pathology indicated "metastasis from uterine leiomyosarcoma." In January 2024, she underwent heavy (carbon) ion therapy. During treatment, her shortness of breath improved, and she became able to lie flat and ambulate. After treatment, the space-occupying lesions in the right hilum and right lung disappeared, and she returned to normal life.
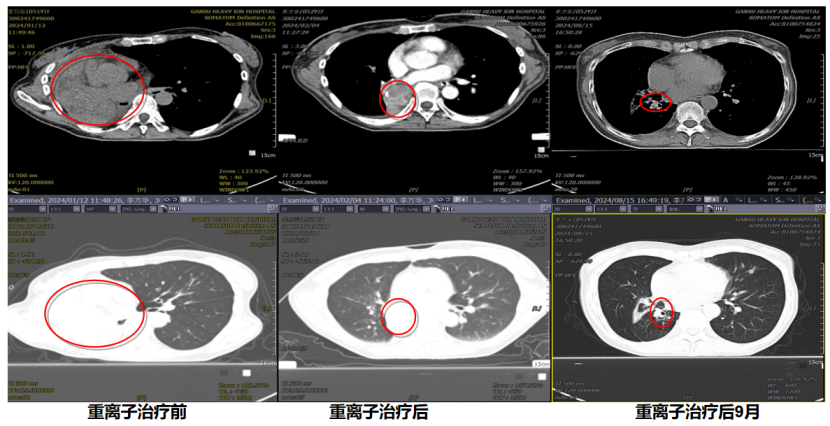
As of the manuscript submission date, 26 months after heavy (carbon) ion therapy, the space-occupying lesions in the patient's right hilum and right lung have disappeared. She is in good physical condition and is able to take care of herself in daily life.
Case provided by: Dr. Pan Xin
Department: Radiation Oncology Center Ⅰ(International Medical Department Ⅰ)
Case 4: Pu XX, female, 35 years old. Chief complaint: Over 4 years post-gastric sarcoma surgery, with low back pain for over 1 month. Diagnosis: 1. Malignant soft tissue neoplasm (post-gastric tumor surgery); 2. Malignant mesenchymal tumor; 3. Secondary malignant neoplasm of the ovary (post-chemotherapy); 4. Secondary malignant neoplasm of the abdominal cavity. Performance status: KPS score 80, ECOG score 1. Pre-treatment status: A large recurrent tumor in the abdominal cavity, deemed unresectable by exploratory laparotomy, accompanied by significant low back pain affecting mobility. Core treatment: Heavy (carbon) ion therapy.
Diagnostic and treatment process
1. Initial diagnosis and treatment (2020): On August 11, 2020, the patient presented with upper abdominal distension and pain, nausea, and melena. Gastroscopy revealed a large irregular ulcer in the gastric antrum, and biopsy pathology indicated "(gastric antrum) spindle cell tumor." Immunohistochemistry supported a diagnosis of malignant mesenchymal tumor, with a proliferation index (Ki-67) of 30%–40%. On October 21, 2020, she underwent surgical resection, and postoperative pathology confirmed malignant mesenchymal tumor of the stomach with vascular tumor thrombus. Genetic testing showed microsatellite stable (MSS) status, with no clear driver gene mutations identified. After surgery, she completed 4 cycles of adjuvant chemotherapy with the "epirubicin + ifosfamide" regimen.
2. First recurrence and treatment (2022): In April 2022, she presented with vaginal bleeding, and pelvic CT revealed a space-occupying lesion in the right pelvic region (7.6 × 5.7 cm). She underwent another surgical resection, with postoperative pathology consistent with the previous findings; immunohistochemistry showed an elevated Ki-67 of 50%. Postoperatively, she received alternating chemotherapy with "epirubicin" and "ifosfamide" for a total of 12 cycles.
3. Second recurrence and referral (2024): In September 2024, she developed low back pain. Chest and abdominal CT at the First Affiliated Hospital of Xi'an Jiaotong University revealed a space-occupying lesion in the splenorenal space, measuring approximately 76 × 60 × 71 mm, suspected to be a tumor metastasis with splenic involvement. On October 15, 2024, she underwent exploratory laparotomy; however, the tumor was deemed unresectable due to severe adhesions with surrounding tissues. Fifteen days after surgery, she was transferred to our Heavy Ion Center for further treatment.
4. Heavy (carbon) ion therapy and efficacy: She received locally radical heavy (carbon) ion therapy. Before treatment (November 5, 2024): CT showed a large intra-abdominal tumor with a volume of 1384.98 cm³. The patient was unable to bend over due to pain and had difficulty walking. After 5 treatment sessions (November 21, 2024): Follow-up CT showed significant tumor shrinkage, with the net tumor volume reduced to 558.89 cm³, a reduction rate of 60%. Improvement in clinical symptoms: After only 2 treatment sessions, the patient's low back pain was significantly relieved, and she was able to walk normally. Imaging at the end of treatment showed that, compared with before treatment, the tumor had been inactivated, significantly reduced in volume, and was in the process of absorption and resolution.
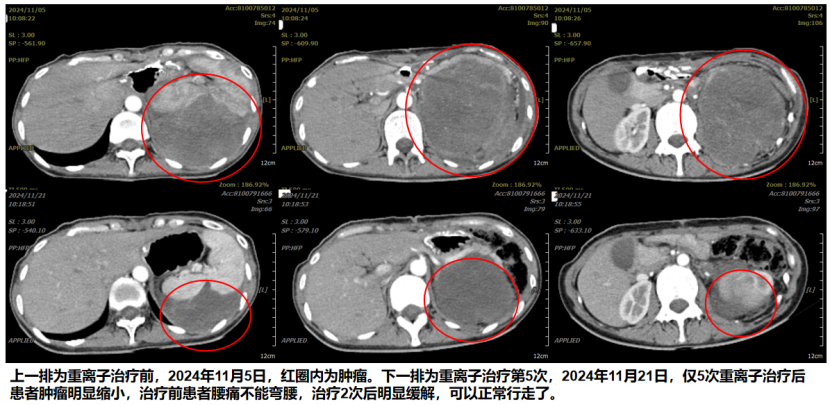
The above figure (upper row): CT image before heavy (carbon) ion therapy (November 5, 2024), with the large recurrent abdominal tumor shown within the red circle. The above figure (lower row): CT image after 5 sessions of heavy (carbon) ion therapy (November 21, 2024), showing a significant reduction in the tumor.
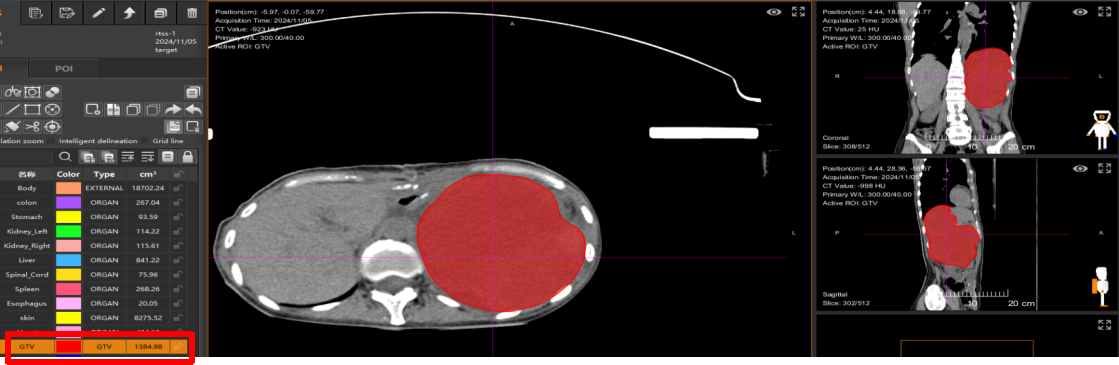
Transferred to Wuwei Heavy Ion Center for heavy (carbon) ion therapy. On November 5, 2024, the heavy (carbon) ion therapy plan was made. The tumor volume before treatment was 1384.98 cm³. The red part is the sarcoma.
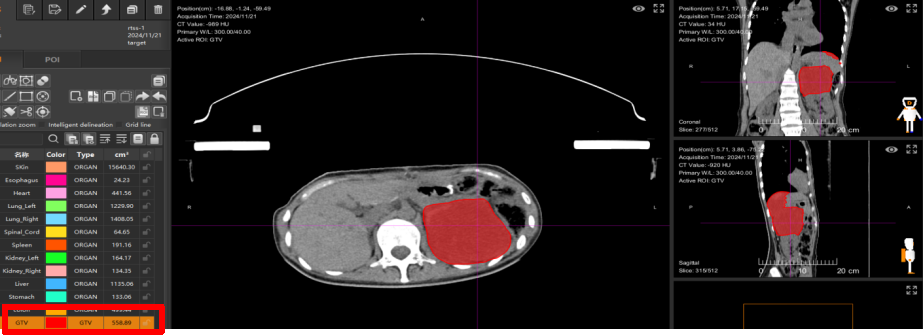
Received heavy (carbon) ion therapy at Wuwei Heavy Ion Center. The net tumor volume before treatment was 1384.98 cm³, and after 5 treatments, the net tumor volume shrank to 558.89 cm³, with the tumor volume reduced by 60%.
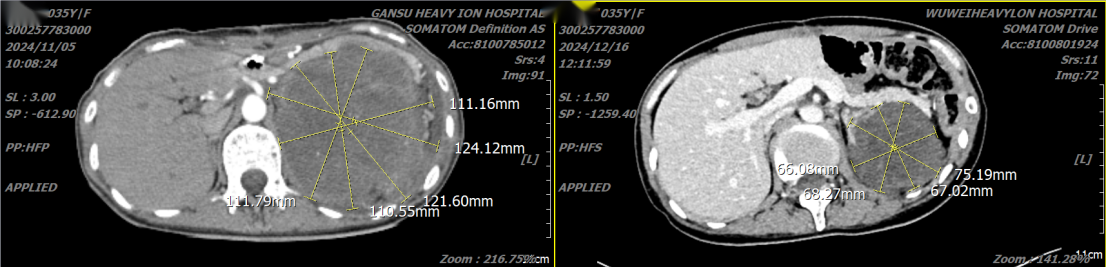
The left image shows the size of the tumor, approximately 120mm, on November 5, 2024, before heavy (carbon) ion therapy. The right image shows that at the end of heavy (carbon) ion therapy, the tumor has been inactivated, significantly shrunk, and is in the process of being absorbed and dissipated.
As of the press release date, 25 months after heavy (carbon) ion therapy, the patient's physical condition is good, the patient is in good health, and can take care of themselves in daily life.
V. Toxic and Side Effects
Due to its precision, heavy (carbon) ion therapy is associated with generally mild toxicities, primarily grade 1–2 local reactions:
Acute/subacute reactions: Skin erythema and dry/moist desquamation in the treated area; mucositis may occur during treatment of head and neck tumors.
Chronic reactions: May include tissue fibrosis in the treated area, with a low incidence.
Special cases in this cohort: Among the three patients with cardiac sarcoma treated, no severe toxicities such as injury to the cardiac conduction system were observed.
VI. Discussion and Summary
Through an analysis of 164 sarcoma patients treated with heavy (carbon) ion therapy, this study confirms the following key points:
Exceptional local control: Heavy (carbon) ion therapy is highly effective against various types of soft tissue sarcomas and osteosarcomas, achieving a local control rate of nearly 100%. It provides a curative local treatment option for patients with inoperable tumors or postoperative recurrence.
Significant survival benefit: Even in this cohort consisting predominantly of patients with advanced-stage and refractory disease, encouraging long-term survival data were obtained, notably a four-year survival rate of 88.89% for osteosarcoma patients.
Broad applicability: The treatment covered nearly all sarcoma subtypes, ranging from common to rare and from extremities to the heart (a world first), overcoming numerous previously established treatment limitations.
Favorable safety profile: The treatment was well tolerated, with a low incidence of severe toxicities, greatly preserving patients' quality of life while effectively combating the cancer.
Outlook
Heavy (carbon) ion therapy represents an important direction in the development of local treatment for sarcomas. As the only medical institution in the world operating two heavy (carbon) ion therapy systems simultaneously, the Wuwei Heavy Ion Center will continue to accumulate "Chinese data" and optimize treatment protocols, bringing this "pillar of national technology" to benefit more patients. The main challenge currently lies in the fact that most physicians and patients are unfamiliar with heavy ion therapy. Many often assume that heavy ions are similar to protons. In reality, heavy ions offer 2 to 5 times the efficacy of protons, with even lower side effects, and no tumor is resistant to heavy ion therapy. With the advancement of technology and the improvement of healthcare systems, heavy (carbon) ion therapy is expected to become one of the indispensable core modalities in the comprehensive treatment of sarcomas.
Contributors: Chen Xuelian, Li Pengqing (Cancer Registration and Follow-up Office)
Reviewer: Zhang Yanshan (Vice President of Gansu Wuwei Cancer Hospital)
Date: March 24, 2026
