1mm Motion Control: Wuwei HFOV Boosts Precision Heavy Ion RT
1mm Motion Control: Wuwei HFOV Boosts Precision Heavy Ion RT
Introduction
What is the biggest concern during radiotherapy? Not the noise of the equipment, not the length of treatment, but the fact that—while you are breathing, your tumor is moving as well.
Respiratory motion causes displacement of the lungs, liver, pancreas, and other thoracic and abdominal organs, making the tumor target "unpredictable"—like aiming at a moving target from a rocking boat. For conventional radiotherapy, this might be managed by expanding the irradiation field as a safety margin. But for precision-heavy ion (carbon ion) radiotherapy, which pursues ultimate accuracy, every single breath carries the risk of compromising treatment efficacy and damaging healthy tissue.
After years of exploration, Professor Zhang Yanshan's team at the Wuwei Heavy Ion Center has pioneered the use of high-frequency oscillatory ventilation (HFOV) under general anesthesia, successfully achieving "apnea-like" precise radiotherapy management. To date, more than 50 patients have safely received this treatment, with significant efficacy and good tolerance. Today, we will discuss this innovative "respiratory control" technology.
I. Why is it Necessary to "Control Breathing" During Radiotherapy?
The heavy (carbon) ion beam features a sharp Bragg peak—where the dose is concentrated at the end of its range, with almost no dose beyond the peak. This is its core advantage for destroying tumors while protecting healthy tissues. However, it also means that positioning must be extremely precise.
Organ displacement caused by respiratory motion is most pronounced in the head-foot direction. Taking the diaphragm as an example, its maximum range of motion during free breathing can reach 3–5 cm, causing the liver, pancreas, and other organs to move substantially as well. If the tumor "moves" while the beam is delivered to the original position, the consequences could be unimaginable.
Even more critically, heavy (carbon) ion therapy often uses a hypofractionated, single high-dose regimen. The treatment time is relatively long, and the requirements for respiratory stability are far higher than those for conventional photon radiotherapy. In short, without good respiratory management, there can be no high-quality heavy (carbon) ion therapy.
II. From "Invasive" to "Non-Invasive": An Advancement in Technology
As early as 2016, Gansu Wuwei Cancer Hospital took the lead in China in implementing the apnea method for precision radiotherapy, which involves the use of muscle relaxants under general anesthesia to temporarily eliminate patient respiratory motion. This method is effective, but has notable limitations:
- Requires the use of a laryngeal mask;
- Demands full-time support from an anesthesia team;
- Carries anesthesia-related risks such as hypoventilation, CO₂ retention, hypoxemia, and circulatory depression;
- Prolonged recovery time, with some patients taking 45 minutes to 3 hours to regain full function.
To overcome these drawbacks, the center's team turned their attention to high-frequency oscillatory ventilation (HFOV).
III. What is High-Frequency Oscillatory Ventilation (HFOV)?
HFOV (high-frequency oscillatory ventilation) is a specialized mode of respiratory support that differs from conventional ventilators:
- Extremely small tidal volume: Below anatomical dead space (approx. 50–60 mL), with almost no chest movement;
- Very high frequency: 240–500 cycles per minute, 10–20 times the normal breathing rate;
- Constant airway pressure: Mean airway pressure maintained at 8–12 cmH₂O, keeping the alveoli continuously inflated;
- Efficient gas exchange: Through high-frequency oscillation and convective diffusion, adequate oxygenation and effective CO₂ clearance are achieved.
In simple terms: HFOV allows patients to "barely breathe" while maintaining normal oxygenation and ventilation—this is precisely the "respiratory stillness" state that precision radiotherapy has long sought.
IV. From Non-Invasive to General Anesthesia: Further Technological Upgrades
The center team first conducted a feasibility study of non-invasive HFOV in 23 healthy volunteers, with results published in Scientific Reports:
- Median respiratory suppression time of 32 minutes, with the longest exceeding 60 minutes;
- Diaphragm motion in the head-foot direction reduced from 1.8 cm during free breathing to 0.3 cm, a reduction of over 80%;
- Coefficient of variation for right lung volume of only 2.4%, demonstrating excellent repeatability;
- Transcutaneous CO₂ only mildly increased by 4–6 mmHg, with no hypercapnia;
- Transcutaneous O₂ significantly increased to over 300 mmHg, indicating adequate oxygenation;
- Good tolerability scores, with no serious adverse reactions.
Based on these findings, the team further explored the application of HFOV under general anesthesia. Why is general anesthesia needed? Because some patients experience discomfort from the high-pressure airflow of the non-invasive mask, or require longer and more stable respiratory suppression. HFOV under general anesthesia combines "anesthetic comfort" with "HFOV precision":
- Patients experience no pain, no fear, and no respiratory resistance;
- Respiratory motion management is more stable and predictable;
- Sustained respiratory suppression of 45–60 minutes can be easily achieved, sufficient for a single hypofractionated session of heavy (carbon) ion therapy;
- Mean recovery time is only about 12 minutes, far shorter than the 90 minutes required for the traditional apnea method.
V. Clinical Practice: Real-World Experience from Over 50 Patients
To date, under the leadership of Dr. Zhang Yanshan, the Wuwei Heavy Ion Center has applied HFOV under general anesthesia to treat more than 50 patients with primary or metastatic malignant tumors of the lung, liver, pancreas, and other sites, with a single-fraction heavy (carbon) ion dose of up to 50 Gy (RBE). Clinical data show:
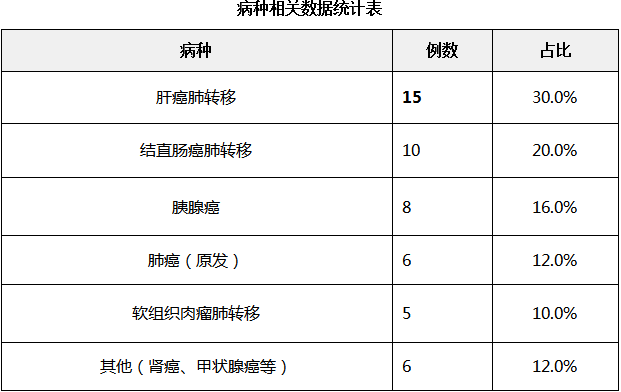
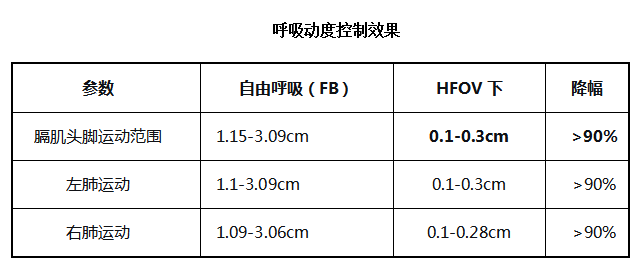
Core conclusion: HFOV controls respiratory motion within 1–3 mm, achieving a "near-stationary" level.
Safety and Tolerability
- Median respiratory control time: 32 minutes, with the longest exceeding 60 minutes;
- Anesthesia recovery time: Mean of 12 minutes, significantly shorter than traditional methods;
- CO₂ retention: TcpCO₂ increased by only 4–6 mmHg, all within normal range;
- Hypoxemia: None;
- Anesthesia-related adverse events: None;
- Treatment completion rate: 100%.
VI. What are the Advantages of this Technology?
Compared with traditional respiratory management methods, HFOV under general anesthesia offers the following core advantages:
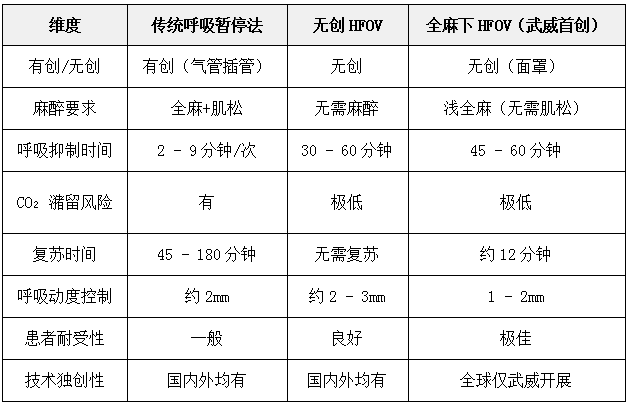
VII. Which patients are most suitable for this technology?
Based on 50 clinical cases, the following patient populations have benefited most from HFOV technology:
- Patients with multiple lung metastases: Numerous lesions (more than 5) with wide distribution, making conventional radiotherapy difficult to cover all targets. HFOV allows simultaneous irradiation of all lesions, achieving "total volume irradiation."
- Patients with liver cancer: The liver moves significantly with respiration (up to 3–5 cm) and is often complicated by cirrhosis, requiring high levels of protection for normal liver tissue. HFOV enables precise irradiation, maximizing preservation of liver function.
- Patients with pancreatic cancer: The tumor is located adjacent to hollow organs such as the stomach and duodenum, where respiratory motion limits the deliverable dose. HFOV allows safe administration of high doses, with even better outcomes when combined with SPACER technology.
- Elderly or frail patients: Unable to tolerate prolonged surgery or conventional radiotherapy. HFOV offers a non-invasive treatment with fast recovery and mild side effects.
- Patients requiring repeated treatments: For example, those with sarcoma lung metastases who often need multiple irradiations for newly developed lesions. HFOV technology is repeatable with stable and consistent results.
VIII. Future Outlook: Beyond Radiotherapy
The success of HFOV under general anesthesia is not limited to heavy (carbon) ion radiotherapy. It can also be applied to:
- Proton radiotherapy: Proton therapy, which also demands stringent respiratory management;
- Stereotactic body radiotherapy (SBRT/SABR): Single-fraction, high-dose, high-precision irradiation;
- Imaging examinations: 4D-CT, PET-CT, MRI, and other scans requiring reduction of motion artifacts;
- Interventional procedures: Radiofrequency ablation, cryoablation, and other minimally invasive treatments that require a "stationary surgical field."
Currently, this technology developed by the center's team is steadily maturing. The inspired oxygen concentration has been reduced from the initial 100% to 50%, while still maintaining adequate ventilation.
IX. Case Examples
Patient Mr. Xie, male, 51 years old, was found to have lung metastases more than six months after undergoing surgery for liver cancer. He faced an extremely challenging situation: a total of 16 metastatic lesions in both lungs (8 in the left lung, 8 in the right lung). Conventional treatment options offered limited efficacy, and due to the large number and wide distribution of the metastases, neither surgery nor conventional radiotherapy could adequately address the condition. The patient was once at a therapeutic impasse.
In July 2022, the patient underwent surgery for liver cancer. Postoperative pathology showed hepatocellular carcinoma (poorly differentiated, Ki-67 50%). Shortly after surgery, multiple metastases appeared in both lungs. From August 2022 to January 2023, he received combination immunotherapy with bevacizumab and sintilimab, but the treatment response was assessed as progressive disease (PD), with an increase in both the number and size of the pulmonary nodules.
For a patient with as many as 16 bilateral lung metastases following liver cancer surgery, there were virtually no better curative treatment options available clinically. However, the innovative technique of HFOV under general anesthesia combined with heavy (carbon) ion radiotherapy, pioneered by Professor Zhang Yanshan at the Wuwei Heavy Ion Center, created a new treatment opportunity for such patients.
Pre-treatment 4D-CT (February 24, 2023) showed that under normal breathing, the 16 metastatic lesions in both lungs shifted significantly with respiratory motion. Under HFOV respiratory management, diaphragmatic motion was controlled to within 1 mm, achieving extremely stable target positioning. In February 2023, the patient underwent a single session of precise heavy (carbon) ion radiotherapy targeting all 16 metastases (8 in the left lung, 8 in the right lung) under general anesthesia combined with high-frequency oscillatory ventilator-assisted respiratory control. The total cost, covering both sites, was 250,000 RMB.
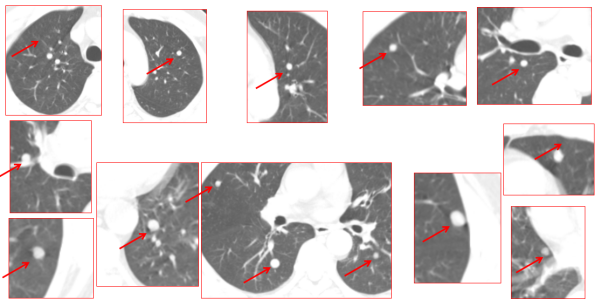
The above image shows 16 metastatic lesions in both the left and right lungs before treatment, with red arrows indicating the pulmonary metastatic nodules.
The above video shows the 4DC taken on February 24, 2023 under normal breathing conditions, and it can be seen that the lung motion amplitude exceeds 1.5 cm.
The above video shows the 4DCT of the same patient on February 24, 2023 under HFOV respiratory control. It can be seen that there is almost no lung motion, only the beating of the heart is visible.
This video shows a CT scan performed in June 2024, 16 months after heavy ion therapy, and the tumor has completely disappeared.
Case provided by: Director Zhang Yihe
Department: Radiation Oncology Center Ⅰ(International Medical Department Ⅰ)
Efficacy Assessment: Before treatment (February 27, 2023), all 16 metastatic lesions in both lungs were clearly visible. Sixteen months after treatment (June 14, 2024), all tumors had completely disappeared, with radiation-induced changes entering the fibrotic stage, and the patient was in generally good condition. This result is highly encouraging—all 16 metastatic lesions were completely inactivated in a single session, with remarkable efficacy and good tolerance.
Conclusion: For cases such as multiple bilateral lung metastases (16 lesions) following liver cancer surgery—where conventional treatment modalities are often ineffective—heavy (carbon) ion radiotherapy combined with high-frequency oscillatory ventilation under general anesthesia offers a novel and effective treatment approach. This case demonstrates that even with as many as 16 pulmonary metastases, heavy (carbon) ion radiotherapy can achieve complete inactivation in a single session under precise respiratory control, creating new hope for patients with advanced-stage cancer.
Finally
Breathing is the essence of life, yet in the context of precision radiotherapy, it becomes the greatest "variable." The non-invasive high-frequency oscillatory ventilation under general anesthesia, pioneered by the Wuwei Heavy Ion Center, skillfully strikes a balance between "sustaining life" and "controlling respiratory motion"—allowing patients to safely "pause" their breathing while enabling the radiation beam to precisely "lock onto" the tumor.
Fifty patients are just the beginning. As this technology matures and becomes more widely adopted, more patients with thoracic and abdominal tumors will benefit from this innovation. The next frontier of precision radiotherapy may very well begin with "strictly managing breathing."
Written by: Zhang Yanshan (Vice President of Gansu Wuwei Cancer Hospital)
Data Support: Chen Xuelian, Li Pengqing (Cancer Registry and Follow-up Office)
Reviewed by: Zhang Yanshan (Vice President of Gansu Wuwei Cancer Hospital)
Date: April 7, 2026
Individual differences exist objectively.
Specific plans vary from person to person.
Gansu Wuwei Cancer Hospital (Wuwei Institute of Medical Sciences)
(Gan) Yiguang [2025] No. 11-14-387
