Heavy Ion Therapy for Cholangiocarcinoma: Survival Advantage in 46 Real-World Cases
Heavy Ion Therapy for Cholangiocarcinoma: Survival Advantage in 46 Real-World Cases
Cholangiocarcinoma, often referred to as the "silent killer" due to its insidious onset, rapid progression, and limited treatment options, is now being challenged by a cutting-edge technology known as a "national heavy instrument" – heavy (carbon) ion therapy – in Wuwei, Gansu. Detailed clinical data are opening a new lifeline for patients with cholangiocarcinoma.
The Wuwei Heavy Ion Center is equipped with China's first heavy ion treatment system possessing complete independent intellectual property rights. Since the first patient was treated in November 2018, the center has completed eight years of clinical practice. As of May 2026, over 2,800 patients have been treated, covering more than 100 tumor types, including 46 cases of cholangiocarcinoma.
I. Survival Data of Cholangiocarcinoma Treatment at Wuwei Center
From November 2018 to May 2026, the Wuwei Heavy Ion Center treated a total of 46 patients with cholangiocarcinoma, of whom over 70% had stage III/IV disease. The survival analysis results (Kaplan‑Meier method) are shown in Table 1.
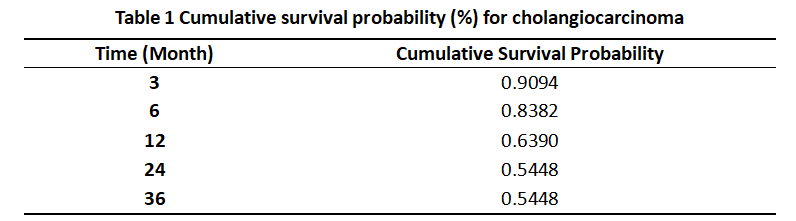
Among the patient cohort, the proportions of stage I and II cases were very small, while stage III/IV accounted for more than 70%. The mean survival time was 24 ± 2.42 months. The survival curve shows a clear plateau, with the survival rate at 24 months being the same as that at 36 months (54.48%), suggesting that patients who remain free of recurrence two years after treatment may achieve long-term survival.
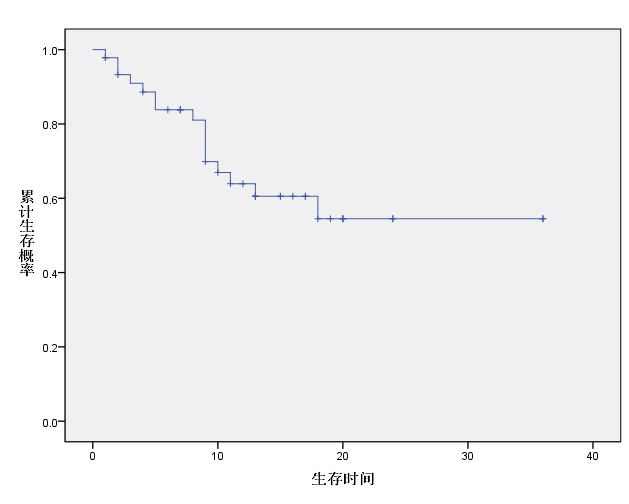
Figure 1 Survival curve of patients with cholangiocarcinoma after heavy ion (carbon ion) therapy (0~36 months)
II. Comparison with Traditional Treatment (Historical Control)
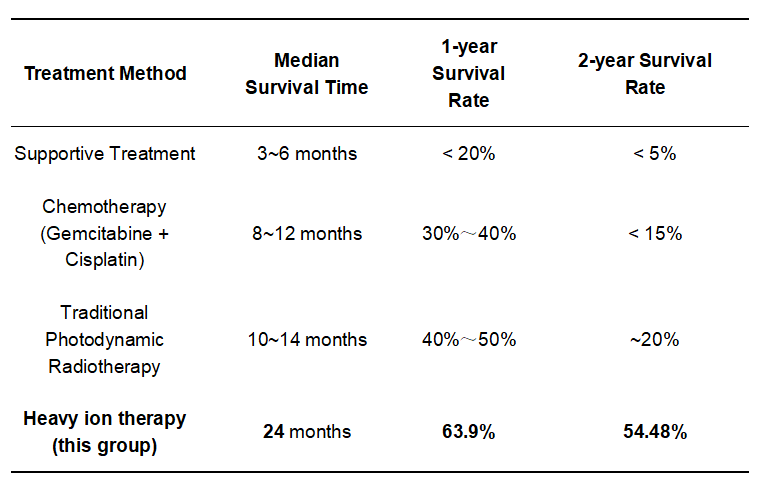
Conclusion: Heavy ion therapy demonstrates significantly superior outcomes compared to historical controls in advanced cholangiocarcinoma, particularly with a 2-year survival rate exceeding 50%, representing an important clinical breakthrough. The real-world data from 46 cases of cholangiocarcinoma at the Wuwei Heavy Ion Center indicate that heavy (carbon) ion therapy achieves survival benefits substantially better than conventional treatments in locally advanced and advanced cholangiocarcinoma, with a 2-year survival rate surpassing 50%. These findings provide robust evidence for the application of China's "national heavy instrument" in treating refractory tumors.
III. Why is cholangiocarcinoma difficult to treat?
The difficulty in treating cholangiocarcinoma is closely related to three major "culprits":
1. Complex anatomy: The bile ducts extend deep into the liver, adjacent to important blood vessels such as the portal vein and hepatic artery. Surgery is extremely challenging, and complete resection is often impossible.
2. Severe hypoxia: Hypoxic regions are common within the tumor tissue. Cells in these areas are highly resistant to conventional photon radiotherapy and chemotherapy, making them a source of recurrence.
3. High invasiveness and early metastasis: Cholangiocarcinoma readily invades along the bile duct wall and metastasizes early to lymph nodes and distant sites, leading to a very poor prognosis.
IV. Why can heavy ions effectively treat cholangiocarcinoma?
Heavy (carbon) ion therapy precisely targets these pain points:
Physical advantage – "precise blasting" via the Bragg peak: Heavy ion energy is precisely deposited in the tumor target area, causing minimal damage to adjacent normal tissues such as the liver and intestines, achieving "millimeter-level" precision.
Biological advantage – "armor-piercing" effect with high RBE: The relative biological effectiveness (RBE) of heavy ions is 2–5 times that of conventional photons. Heavy ions directly induce double-strand breaks in tumor cell DNA and remain effective against hypoxic cells and radioresistant cells.
Spatial advantage – regional clearance: Heavy ion therapy can cover the tumor itself, the bile duct invasion pathway, and high-risk lymphatic drainage areas, achieving "one‑stop" regional cure.
Core conclusion: For cholangiocarcinoma with a very poor prognosis – especially the patient cohort in this study, which contained a high proportion of advanced cases – the 3‑year survival rate after heavy ion therapy remained above 50%. This outcome is significantly better than historical results of conventional palliative treatment and brings new hope for the treatment of advanced cholangiocarcinoma.
V. Typical Cases
Case 1: Mr. Hai, 81 years old, extrahepatic cholangiocarcinoma, cT3N0M0 stage IIB
In January 2025, the patient presented with fever and chills. Abdominal CT revealed low biliary tract obstruction and a nodular shadow at the distal end of the common bile duct, approximately 1.7 cm in longest diameter, suspicious for cholangiocarcinoma. On February 6, 2025, ERCP was performed with placement of a biliary stent. Pathology showed moderately differentiated adenocarcinoma. Due to the patient's advanced age, the patient and his family declined surgery and chemotherapy. Subsequently, he consulted Professor Zhang Yanshan at the Wuwei Heavy Ion Center, where he received heavy ion therapy targeting the bile duct tumor and lymphatic drainage area. During and after treatment, the patient experienced no significant discomfort, and the lesion disappeared.
Currently, at 13 months post-treatment, the lesion has disappeared, with only slight thickening of the bile duct wall. Tumor markers are within normal limits, and the patient is generally in good condition, living a normal life. Due to his advanced age, the patient himself is unwilling to receive additional treatment.
Case provided by: Attending Physician Wang Xin
Department: Radiation Oncology Center Ⅰ(International Medical Department Ⅰ)
Case 2: Ms. Wu, 68 years old, intrahepatic cholangiocarcinoma, cT1bN0M0 stage IB
In June 2022, a liver mass was detected during a routine physical examination. In July 2022, the patient underwent Yttrium-90 therapy (costing over 400,000 RMB). However, three months after treatment, significant progression of the primary tumor was observed. In February 2023, follow-up abdominal MR revealed abnormal mass signals in segments S4 and S5 of the liver, with clear demarcation from the gallbladder and the left and right branches of the portal vein, and the lesion had enlarged compared to previous imaging. The patient received targeted therapy, immunotherapy, and transarterial chemoembolization (TACE). Subsequently, in April 2023, she visited our hospital and underwent carbon ion radiotherapy.
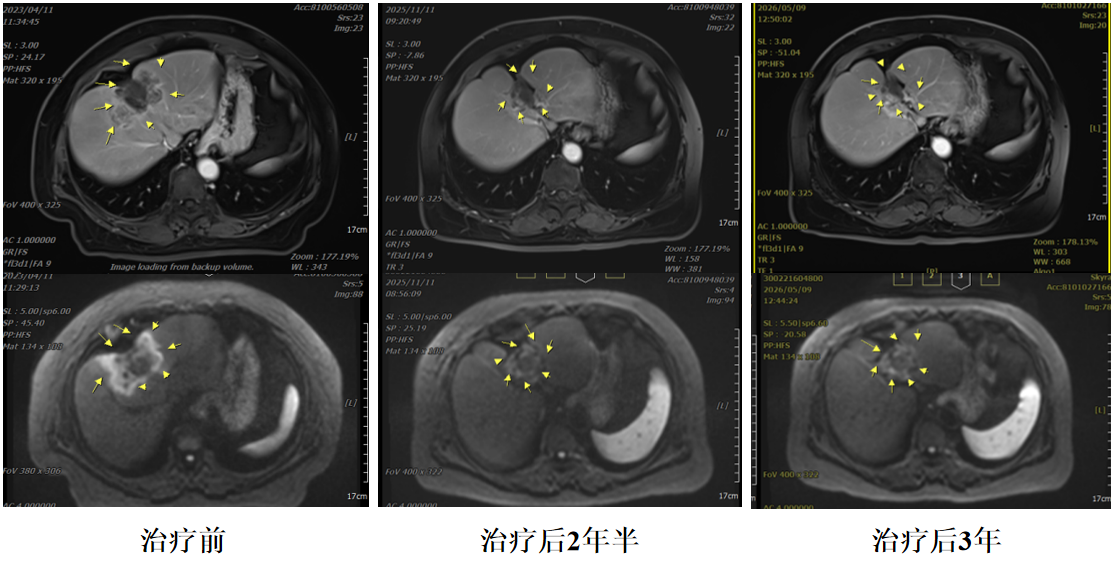
Now, more than three years after treatment, the patient has been off all anticancer medications for over two years. She is in good health and regularly returns to our center for follow-up every three months. There is no evidence of any tumor, and she is living a normal life.
Case provided by: Attending Physician Ma Tong
Department: Radiation Oncology Center Ⅰ(International Medical Department Ⅰ)
Case 3: Ms. Jiang, 77 years old, hilar cholangiocarcinoma, cT1N0M0 stage I
In July 2024, the patient was admitted with jaundice and severe liver function abnormalities. Abdominal CT showed marked dilation of the intrahepatic bile ducts with obstruction at the hepatic hilum, and the common bile duct was not clearly visible. After PTCD drainage, the jaundice improved. The patient and her family explicitly refused surgery. Subsequently, she visited our hospital and underwent heavy ion radiotherapy combined with two cycles of concurrent chemotherapy. The treatment was completed successfully, the lesion was effectively controlled, the jaundice resolved, and the patient recovered well.
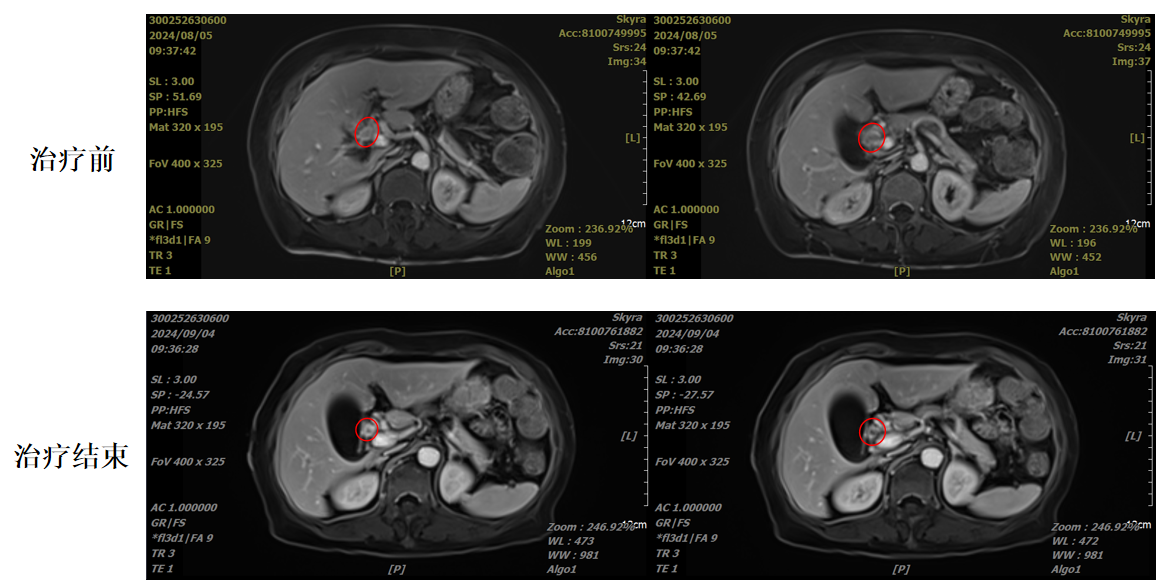
For early-stage hilar cholangiocarcinoma in patients who are unable or unwilling to undergo surgery, heavy ion therapy offers a non‑invasive curative option. It is particularly suitable for elderly patients or those with multiple comorbidities, and is associated with no significant adverse effects or suffering during treatment, thereby ensuring a high quality of life.
Case provided by: Attending Physician Wang Xin
Department: Radiation Oncology Center Ⅰ(International Medical Department Ⅰ)
Case 4: Ms. Cheng, 79 years old, extrahepatic cholangiocarcinoma, cT3N1M0 stage IIB
In August 2024, the patient presented with darkening of urine color, accompanied by dry mouth, bitter taste, and postprandial abdominal discomfort. The urine gradually became tea-colored. Abdominal MRCP revealed low biliary tract obstruction and an abnormal change in the distal segment of the common bile duct, approximately 1.4 cm in length, suggestive of a neoplastic lesion. The patient and her family declined surgery. Subsequently, she visited our hospital and received carbon ion radiotherapy targeting the bile duct tumor and lymphatic drainage area, along with two cycles of concurrent chemotherapy. After treatment, the lesion was significantly reduced in size.
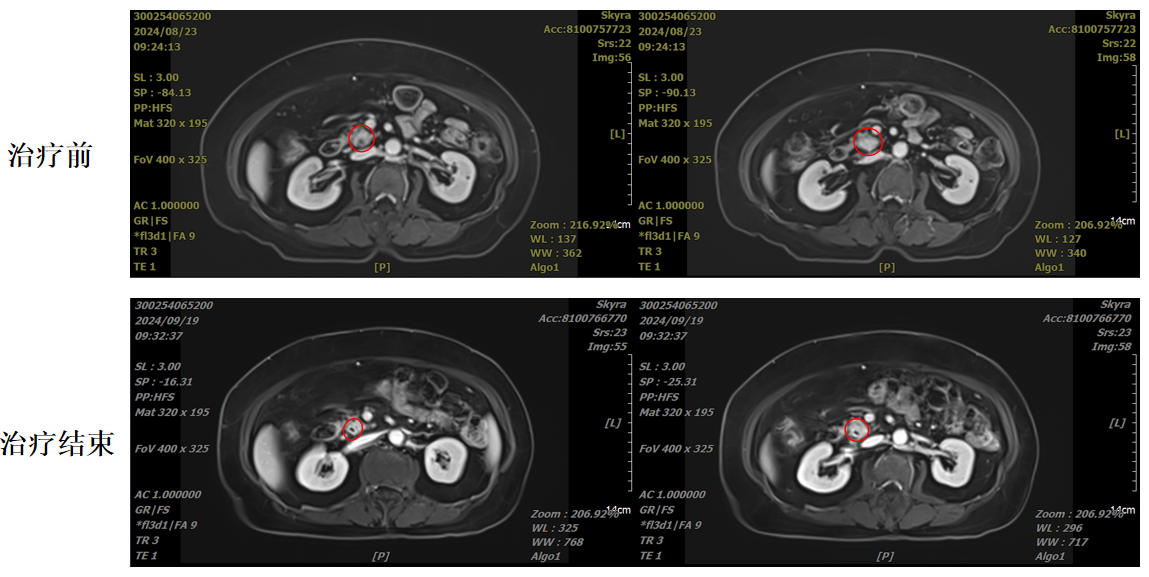
At 20 months post-treatment, the patient remains free of any significant discomfort and has returned to normal life. She is unwilling to go to the hospital for follow-up examinations, stating that she feels no discomfort at all and that it was a very wise treatment choice.
Case provided by: Attending Physician Wang Xin
Department: Radiation Oncology Center Ⅰ(International Medical Department Ⅰ)
VI. Which patients are suitable?
Priority Recommendation:
- All stages of intrahepatic and extrahepatic cholangiocarcinoma are suitable for heavy ion therapy.
- For early-stage patients: Surgery is also an option. If surgery is unwilling or not feasible for various reasons, heavy ion therapy is the best choice.
- For locally advanced, unresectable, or unwilling-to-operate patients: Heavy ion therapy offers significant advantages.
- For postoperative recurrence or residual disease that cannot be re-operated: Heavy ion therapy can address visible lesions.
- For stage IV patients with oligometastasis (e.g., single or few metastatic lesions in the liver or lymph nodes).
Need for Caution (limited efficacy): Diffuse intrahepatic metastasis, extensive peritoneal metastasis, or bone marrow metastasis.
Note: In heavy ion therapy for intrahepatic and extrahepatic cholangiocarcinoma, irradiation of the draining lymphatic drainage area is generally required. This is a major advantage of heavy ion therapy. Moreover, metastatic lymph node cancers are particularly sensitive to heavy ions, which is a key reason why heavy ion therapy significantly improves survival rates.
VII. Conclusion
Cholangiocarcinoma was once considered a "tough nut" in oncology. However, at the Wuwei Heavy Ion Center, real-world data from 46 patients demonstrate that heavy ions—with their high efficacy, low toxicity, and precision—are becoming a powerful weapon in the treatment of cholangiocarcinoma.
The Wuwei Heavy Ion Center is the clinical application base for China's first heavy ion (carbon ion) treatment system with complete independent intellectual property rights. The system is technically supported by the Institute of Modern Physics, Chinese Academy of Sciences, and clinically operated by Gansu Wuwei Cancer Hospital. The center officially began treating tumors in November 2018. To date, it has treated over 2,800 patients, covering more than 100 tumor types, including lung cancer, pancreatic cancer, liver cancer, glioblastoma, nasopharyngeal carcinoma, rectal cancer, and various sarcomas. As the only medical institution in the world operating two heavy ion (carbon ion) treatment systems simultaneously, the center has achieved nine "world‑first" innovations in technology: pioneering precise radiotherapy under ventilator control; bladder cancer treatment with accurate bladder capacity management; single‑fraction radiotherapy using surgically implanted spacers between organs and tumors; developing the world's first 360° rotatable and liftable ion radiotherapy chair; performing the world's first heavy ion (carbon ion) treatments for cardiac tumors; and pioneering dual‑Bragg‑peak lattice radiotherapy with heavy ions, among others. Leveraging 30 research platforms including the CAS Key Laboratory of Heavy Ion Radiation Biology and Biomedicine and the Sydney University Biomedical Data Analysis and Visualization Laboratory, the center has conducted over 30 clinical studies on major tumor types. To date, the center has published nine monographs, including the Standard Operating Procedure for Carbon Ion Radiotherapy, establishing a comprehensive knowledge system covering physical technology, clinical diagnosis and treatment, and health management.
Writer: Wang Xin, First Department of Radiotherapy Center
Data Support: Tumor Registry and Follow-up Office (Chen Xuelian, Li Pengqing)
Reviewer: Zhang Yanshan (Vice President)
Date: May 11, 2026
