"Four Brothers" of Particle Cancer Therapy: Electrons, Protons, Heavy Ions, Boron Neutrons
"Four Brothers" of Particle Cancer Therapy: Electrons, Protons, Heavy Ions, Boron Neutrons – Can't Tell Them Apart?
Foreword
Since 2012, when China’s first heavy ion device was established in Wuwei, Gansu, we have been deeply involved in the field of particle therapy for cancer. From that point on, we began the journey of building China’s first heavy ion facility. After eight years of arduous efforts, the first patient received formal heavy ion therapy in November 2018, marking China as the third country in the world—after Japan and Germany—to master the entire chain of heavy ion production, research, clinical application, and cancer treatment technology. Building on the success of the Wuwei Heavy Ion Center, subsequent heavy ion centers have reduced their construction period to just 3–5 years. Now, 14 years later, heavy ion therapy in China has grown from nothing, evolving from exploration to maturity. The Wuwei Heavy Ion Center has treated over 2,800 cancer patients, and currently treats more than 100 patients per month, with increasingly refined techniques bringing new hope to many more cancer patients.
In daily practice, patients and their families often ask: What exactly is the difference between electrons, protons, heavy ions, and boron neutrons—all these high-tech-sounding options? Which one is better? Today, we will demystify these four particle radiotherapy technologies in the most accessible way possible.
1. They Are All "Particles," But Each Has Its Own Temperament
In the radiation therapy family, there are two major categories: one is photons (X-rays, gamma rays), and the other is particles. Electrons, protons, heavy ions (carbon ions), and neutrons all belong to the particle family, but their "personalities" are vastly different.
To use an analogy: if conventional radiotherapy is a "shotgun," then particle radiotherapy is a "sniper rifle." However, the ammunition and lethality of these four "sniper rifles" are quite different from one another.

Left: Electron beam. Due to their light mass, electrons are easily scattered, have a short range, and the Bragg peak is not sharp enough.
Right: Proton beam. The Bragg peak is sharper.
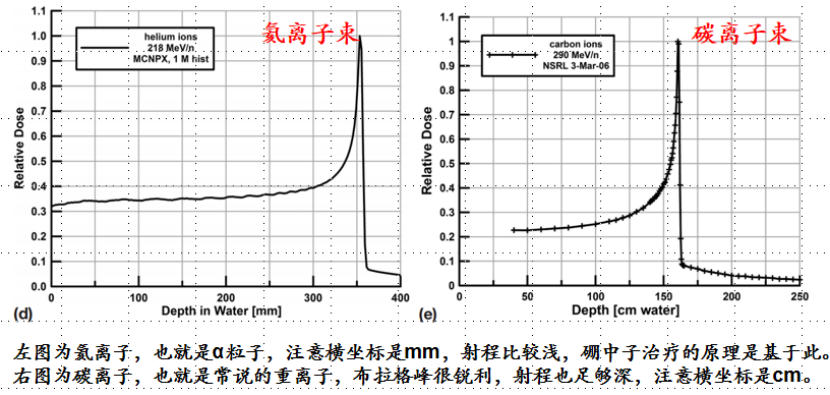
Left: Helium ions (alpha particles). Note that the x-axis is in mm, the range is relatively shallow. This is the principle behind boron neutron capture therapy (BNCT).
Right: Carbon ions, commonly referred to as heavy ions. The Bragg peak is very sharp, and the range is sufficiently deep. Note that the x-axis is in cm.
Figure 1: Schematic comparison of depth-dose distribution of four types of particle beams
2. Electrons: The Underestimated "Poor Man's Particle Knife"
What is the principle?
Electrons are the lightest charged particles. Many people think that only protons have a Bragg peak—but that's not the case. Electrons also have a Bragg peak. Within a certain energy range, electrons also exhibit a "bulge" of energy deposition at the end of their range, known as a "Bragg-like peak." It is precisely this characteristic that has earned electrons the reputation in the field as the "poor man's particle knife" or the "poor man's proton."
Due to their very small mass, electrons have a short range. After penetrating just a few centimeters into tissue, their energy rapidly attenuates. This very feature makes them a "powerful tool" for treating superficial tumors.
Advantage
- Definitive efficacy for superficial tumors: Such as skin cancer, lip cancer, post-operative chest wall irradiation for breast cancer, superficial lymph node metastases, etc.
- Simple equipment and low cost: Medical electron linear accelerators are available in almost every radiation oncology department
- Mature technology and extensive experience: Decades of clinical application ensure safety.
- Good protection of normal tissues: Penetration depth is controllable, and deep normal tissues are not affected
Limitation
- Limited range (generally no more than 5–7 cm), making it unable to treat deep-seated tumors.
- Dose distribution is not as "sharp" as that of protons and heavy ions.
- Biological effectiveness comparable to X-rays, with no particular advantage.
The "Status in the Field" of Electrons
Electrons are the most "down-to-earth" technology in radiation oncology. They are unassuming, yet play an irreplaceable role in areas such as skin cancer, postoperative radiotherapy for keloids, and post-lumpectomy radiotherapy for breast cancer. If protons and heavy ions are "luxury sports cars," then electrons are the "pickup truck"—not flashy, but practical, reliable, and affordable for everyone. Thanks to their Bragg-like peak and low cost, they are vividly known as the "poor man's particle knife."
3. Proton Therapy: The Precise "Little Hammer"
What is the principle?
Protons are the nuclei of hydrogen atoms. Proton therapy uses an accelerator to speed protons to about 70% of the speed of light, then precisely directs them at the tumor.
Protons have a remarkable physical property—the Bragg peak. What does that mean? When conventional X-rays enter the body, their energy is highest near the skin, then gradually decreases as they travel through the body. By the time they reach the tumor, they may have lost much of their punch, and they continue past the tumor, damaging healthy tissue beyond it. In contrast, a proton beam releases very little energy before reaching the tumor, unleashes its full energy at the tumor site, and then stops abruptly—like a "precision demolition expert.
Advantage
- Precisely targets tumors, minimal damage to normal tissu
- Especially suitable for pediatric tumors, skull base tumors, left-sided breast cancer (spares the heart)
- Most widely used particle radiotherapy worldwide (over 200,000 patients treated)
Limitation
- Tumor-killing effect not fundamentally different from X-rays (RBE ~1.1x)
- Limited efficacy against hypoxic and radioresistant tumors
- Expensive equipment (~¥300 million), high treatment cost
A Thought-provoking Example
As of 2026, the U.S. has 47 proton centers, but most are operating at a loss. Why? Because insurance companies won't pay. They know clearly: proton therapy offers comparable efficacy to intensity-modulated photon radiotherapy, with the only advantage being reduced damage to surrounding organs. Therefore, insurers are only willing to cover proton therapy for a few indications—such as left-sided breast cancer (where the heart lies behind the target area). This fully reflects scientific rigor—efficacy comes first.
4. Heavy Ion (Carbon Ion) Therapy: The True "Sledgehammer" – and a Superior Choice
What is the principle?
Heavy ion typically refers to carbon ion (hereinafter referred to as heavy ion). It is much heavier than a proton and bombards the tumor after being accelerated to 70% of the speed of light. Heavy ions not only possess the proton's Bragg peak but also have a "superpower" that protons lack — high relative biological effectiveness (RBE).
The RBE of heavy ions can reach 2–5 in the Bragg peak region, which is 2–5 times that of protons. This means:
Directly destroys the double strands of tumor cell DNA, causing "lethal damage"
Equally effective against hypoxic tumor cells (does not rely on oxygen free radicals)
Not affected by the cell cycle, can kill tumor cells at all stages
Why is it called "the most balanced ray"?
Heavy ions have low LET in the entrance channel (sparing normal tissue), peak LET in the Bragg peak region (efficiently killing tumors), and then drop sharply after the peak. This perfect "low entrance, high peak" combination has earned it the reputation as the "most superior and balanced radiation" of the 21st century.
Clinical Advantages
- Short treatment course: 1–4 weeks, average less than 3 weeks
- Better efficacy: Proven effective against refractory and radioresistant tumors, and also more effective than conventional therapy for common tumors
- Milder side effects: Better protection of normal tissues, higher quality of life
- Significantly reduced cost: Heavy ion therapy cost has dropped to under 200,000 RMB for the full course, greatly improving accessibility
- Expanding indications: Previously thought suitable only for refractory and resistant tumors, accumulating evidence now shows that nearly all tumors suitable for proton and photon therapy are also suitable for heavy ion therapy, with better efficacy and milder side effects
Scope of indications
- Tumors that respond poorly to conventional radiotherapy, such as osteosarcoma, chordoma, pancreatic cancer, and liver cancer
- Common tumors such as head and neck cancer, lung cancer, prostate cancer, and esophageal cancer
- Special types such as pediatric tumors and recurrent tumors
China's Path to Heavy Ion Therapy
In 2012, China's first heavy ion equipment was installed in Wuwei, Gansu Province, marking the beginning of heavy ion therapy in China. The construction of the Wuwei center took eight years. With the successful experience gained from the Wuwei Heavy Ion Center, the construction period for subsequent centers has been shortened to 3–5 years. In November 2018, the first patient officially received heavy ion therapy, a milestone event in the history of heavy ion therapy in China.
Only a few countries in the world have mastered this technology, with Japan, China, and Germany ranking in order of development. Today, the Wuwei Heavy Ion Center has treated over 2,800 patients with various types of tumors, and the pace is accelerating while the technology is becoming increasingly mature. Currently, more than 100 patients are treated per month. Remarkable efficacy has been achieved in difficult-to-treat tumors such as esophageal cancer, pancreatic cancer, liver cancer, and osteosarcoma, while better outcomes and milder side effects have also been demonstrated in the treatment of common tumors.
Fourteen years have passed. Heavy ion therapy in China has grown from nothing, from exploration to maturity, and is bringing hope to an increasing number of patients.
5. Boron Neutron Capture Therapy (BNCT): The "Elder" Who Debuted First – Why Was It Cast into the Cold Palace?
A misunderstood "rising star"
Many people think Boron Neutron Capture Therapy (BNCT) is a new technology that has emerged only in recent years, but that is not the case. Research on BNCT dates back to 1936, earlier than the clinical application of both protons and heavy ions, making it the true "elder" in the field of particle therapy.
What is the principle?
Boron neutron therapy takes a different approach. Unlike other particles that directly bombard the tumor with particle beams, it uses a "two-step" strategy:
- Administer the drug first: Inject the patient with a boron-10 containing drug, hoping it will specifically accumulate inside the tumor cells.
- Then irradiate: Irradiate the tumor area with a neutron beam. When neutrons are "captured" by the boron-10 within the tumor, a nuclear reaction occurs, releasing alpha particles and lithium ions.
Alpha particles are essentially helium ions, a type of heavy ion. Therefore, the essence of boron neutron therapy is to use the alpha particles (heavy ions) generated by bombarding boron-10 with neutrons to kill the tumor.
Why was he relegated to the cold palace?
Since the principle sounds perfect, why hasn't boron neutron therapy become mainstream? There are three main reasons:
1. The boron drug is a fatal bottleneck
The key to the success of BNCT lies in the first step — whether the boron drug can accumulate in the tumor with high concentration and specificity. Ideally, the boron concentration in the tumor should be 3–5 times higher than in normal tissue. But in reality, this goal is very difficult to achieve. The boron drug also distributes in normal tissues, causing damage to normal tissues during neutron irradiation.
2. Severe side effects are daunting
Due to the suboptimal selectivity of the boron drug and the inherent scattering of the neutron beam, BNCT has historically caused severe normal tissue damage, including radiation-induced brain necrosis, skin ulceration, vascular rupture, and other serious complications. This is the fundamental reason it was cast into the "cold palace."
3. Efficacy is inferior to heavy ion therapy
More importantly, although the alpha particles (helium ions) produced by BNCT are also heavy ions, they are inferior to carbon ions in both physical and biological aspects. Carbon ions have a sharper Bragg peak, less scattering, higher RBE (2–5 vs. approximately 1–3 for alpha particles), and more thorough tumor killing. In short, any efficacy achievable with BNCT can be better achieved with heavy ion therapy.
Why has it been “hyped” again in recent years?
In recent years, boron neutron therapy has suddenly regained popularity, mainly for two reasons:
- Low equipment cost: A BNCT device costs only a fraction (1/20th to 1/30th) of heavy ion equipment, with a much shorter construction period, making it attractive to capital.
- "Spillover effect" from mature heavy ion technology: After China's heavy ion technology matured, related research experience and talent have spilled over, driving renewed exploration of BNCT.
However, we must clearly recognize: cheap equipment does not equal good efficacy. As of October 2022, there is no medical institution in the world routinely performing BNCT. The vast majority of research remains at the small-sample, exploratory stage, and both efficacy and safety still need to be validated by large-scale prospective studies.
A question worth pondering
If the boron drug problem were solved, could BNCT challenge the position of heavy ion therapy? The answer is: very unlikely. Because even under ideal conditions, the physical properties and biological effects of alpha particles are still inferior to those of carbon ions. Carbon ion is widely recognized as the "most balanced" member of the heavy ion family — it is neither too light (like helium ions, with insufficient RBE) nor too heavy (like neon ions, which can cause "overkill" effects). This "goldilocks balance point" is a unique advantage of carbon ions.
六、四兄弟对比一图看懂
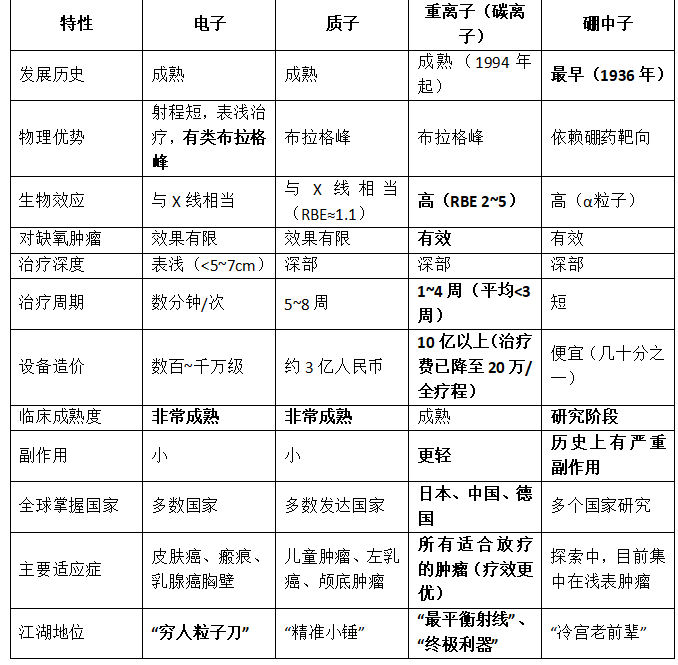
7. Scientific Selection: Don’t Choose the Most Expensive or the “hottest” One, Just Choose the Right One
1. Electrons: The "Poor Man's Particle Knife" for Superficial Tumors
For skin cancer, lip cancer, post-operative chest wall irradiation for breast cancer, and prevention of keloid recurrence after surgery, electrons are the most cost-effective and reliably effective choice. They are not flashy, but practical and dependable. With their Bragg-peak-like characteristics and low cost, they are aptly described as the "poor man's particle knife."
2. Protons: Precise Protection, but Efficacy Comparable to Photons
In terms of tumor-killing efficacy, protons are not fundamentally different from advanced intensity-modulated X-ray radiotherapy. Their advantage lies in better protection of surrounding normal tissues. Therefore, protons are advantageous for tumors in special locations (such as those near critical organs). However, it is worth noting that among the 47 proton centers in the United States, most are operating at a loss, reflecting the limitations of their efficacy.
3. Heavy Ions (Carbon Ions): The True "Ultimate Weapon" – and the Superior Choice
For tumors that respond poorly to conventional radiotherapy—such as osteosarcoma, chordoma, pancreatic cancer, and liver cancer—the high biological effectiveness of heavy ions offers a clear advantage. Their RBE can reach 2–5, which is 2–5 times that of protons (RBE ≈ 1.1).
More importantly, accumulating evidence shows that nearly all tumors suitable for proton and photon therapy are also suitable for heavy ion therapy, with better efficacy and milder side effects. The treatment course for heavy ion therapy is only 1–4 weeks (average less than 3 weeks), and the total cost for the full course has dropped to under 200,000 RMB. Patients enjoy a higher quality of life and live with greater dignity. It is currently recognized as the most balanced and superior heavy ion beam for cancer treatment. In reality, any efficacy achievable with BNCT can be better achieved with heavy ion therapy
4. Boron Neutron: A Rational Perspective – Not to Be Overhyped
Although BNCT is the "elder" in the field, it has long been cast into the "cold palace" due to the boron drug bottleneck and side effect issues. Renewed research in recent years is worth attention, but patients and their families should view it rationally and not regard it as a mature treatment option. Until a breakthrough is achieved in boron drugs, heavy ions remain the preferred choice for particle cancer therapy.
8. Editor's Note
As workers in the field of particle therapy, we are often asked: "Which one is the best?" The answer is: There is no best technology, only the most suitable treatment plan.
- Superficial tumors → Electrons are sufficient, don't waste money (they are the "poor man's particle knife")
- Pediatric tumors, tumors in special locations → Protons are a good choice; heavy ions offer even better tissue sparing
- Nearly all tumors suitable for radiotherapy → Heavy ions are the superior choice (better efficacy, milder side effects, shorter course, affordable cost)
- Boron neutron → Long history but still a long way to go; currently not recommended as a first-line option
More importantly, don't blindly pursue "high-tech" solutions. Modern intensity-modulated photon radiotherapy (IMRT) can already achieve very precise dose distribution. For many common tumors, it remains a safe, effective, and cost-effective choice.
Looking back at the development of heavy ion therapy in China: In 2012, the first equipment was installed in Wuwei. After eight years of construction (with the successful experience of the Wuwei Heavy Ion Center, subsequent centers have shortened the construction period to 3–5 years), the first patient received treatment in November 2018. Fourteen years have now passed. These 14 years have witnessed heavy ion therapy in China grow from nothing, from exploration to maturity. Today, the Wuwei Heavy Ion Center has treated over 2,800 patients, currently treating more than 100 patients per month. The technology is increasingly mature, and the cost has dropped to under 200,000 RMB for the full course, bringing hope of cure and a higher quality of life to an increasing number of patients.
We have reason to believe that with continuous technological advancement and accumulating experience, heavy ion therapy will play an increasingly important role in the field of oncology.
Finally, to borrow the words of a senior colleague: "What patients pursue is always effective tumor treatment, not how flashy the technology is." We hope this article helps everyone rationally understand these four particle cancer therapy technologies and make informed choices.
References
[1] Kanai T, Endo M, Minohara S, et al. Biophysical characteristics of HIMAC clinical irradiation system for heavy-ion radiation therapy.International Journal of Radiation Oncology, Biology, Physics, 1999, 44(1): 201-210.
[2] Kanai T, Furusawa Y, Fukutsu K, et al. Irradiation of mixed beam and design of spread-out Bragg peak for heavy-ion radiotherapy.Radiation Research, 1997, 147(1): 78-85.
[3] Karger CP, Peschke P, Sanchez-Brandelik R, et al. Dose response and dose-volume effects for the rat spinal cord after carbon ion irradiation: the impact of dose-averaged linear energy transfer.Radiotherapy and Oncology, 2006, 78(3): 270-276.
[4] Weyrather WK, Kraft G. RBE of carbon ions: experimental data and the concept of the local effect model.Journal of Radiation Research, 2004, 45(1): 1-9.
[5] Weber U, Kraft G. Comparison of carbon ions versus protons.The Cancer Journal, 2009, 15(4): 325-332.
[6] Wang D, Liu R, Zhang Q, et al. Charged Particle Irradiation for Pancreatic Cancer: A Systematic Review of In Vitro Studies.Frontiers in Oncology, 2022, 11: 775597.
[7] 张雁山等. 碳离子束放射治疗肿瘤的临床进展.医学综述, 2017.
[8] 硼中子俘获疗法的临床应用综述(译文). 中国武威重离子中心.
[9] 质子和重离子的区别. 甘肃武威肿瘤医院重离子中心.
[10] 质子重离子治疗癌症的基础原理. 太怡生命, 2019.
[11] Nedunchezhian K, et al. Boron Neutron Capture Therapy - A Literature Review.Journal of Clinical and Diagnostic Research, 2016, 10(12): Ze01-Ze4.
About the author
Zhang Yanshan, M.D., Ph.D., Chief Physician of Surgery and Chief Physician of Radiation Oncology. Guest Researcher and Supervisor at the University of Chinese Academy of Sciences, Professor and Master's Supervisor at Gansu University of Chinese Medicine, Professor and Master's Supervisor at Northwest Normal University, among others. Recognized as a Leading Talent of Gansu Province and an Outstanding Expert of Gansu Province. Director of the Wuwei Heavy Ion Center. Praised by Dr. Joerg Hauffe, CEO of the RPTC Proton Center in Germany, as "Mr. Carbon." Dr. Zhang was the first in China to engage in clinical treatment using domestically produced heavy ion technology. He treats the largest number of heavy ion cases annually in China, with the most complex medical conditions, and has accumulated extensive experience in heavy ion therapy for solid tumors across various anatomical sites. He pioneered the "galloping scheme" for treating bladder cancer, the High-Frequency Oscillatory Ventilation (HFOV) technique to control respiratory motion, and the surgical "spacer technique," thereby establishing the concept of "heavy ion surgery."
Reviewed by: Zhang Yanshan (Vice President, Gansu Wuwei Cancer Hospital)
Individual differences objectively exist
Specific treatment plans vary from person to person
Gansu Wuwei Cancer Hospital (Wuwei Academy of Medical Sciences)
(Gan) Medical Advertisement [2025] No. 11-14-387
