Wuwei Heavy Ion Center: Summary and Analysis of 77 Cases of Chordoma Treated with Heavy (Carbon) Ion
Wuwei Heavy Ion Center: Summary and Analysis of 77 Cases of Chordoma Treated with Heavy (Carbon) Ion Therapy
I. Basic Information
Since the treatment of the first patient in November 2018, as of April 1, 2026, the Wuwei Heavy Ion Center has treated 77 patients with chordoma using heavy (carbon) ion therapy. Among them, there are 54 males and 23 females, with a mean age of (53.79 ± 15.32) years (age range: 16 to 80 years). Of these patients, 27 had previously undergone surgery, while 50 had not. The Wuwei Center has treated a large number of patients with complex, large, inoperable tumors, or those for whom surgery would have led to severe functional loss (e.g., loss of bowel and bladder control, motor dysfunction), further confirming the unique efficacy of heavy (carbon) ion therapy.
II. Survival Status
A survival analysis was conducted on the 50 chordoma patients who did not undergo surgery, with a follow-up period ranging from 0 to 64 months. The Kaplan-Meier (K-M) method was used for survival analysis. The cumulative survival probability at the end of treatment was 1.0000. The cumulative survival probabilities at 12, 24, and 36 months after treatment were 0.9800, 0.8590, and 0.7636, respectively (see Table 1).
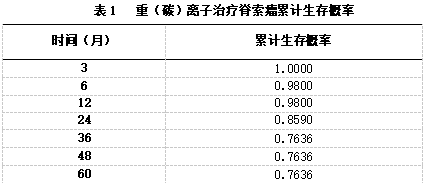
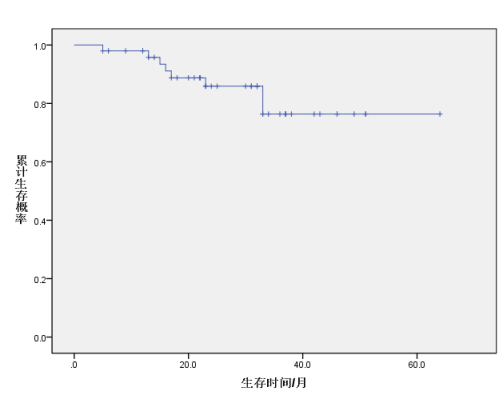
Figure 1 Survival curve from the end of treatment to 60 months after treatment
III. Summary of 8 Years of Experience in Heavy (Carbon) Ion Therapy for Chordoma
Based on available clinical data, heavy (carbon) ion therapy offers an effective, low-toxicity treatment option for chordoma, particularly suitable for surgically unresectable or recurrent tumors. A quantitative analysis based on evidence-based data is presented below:
3.1 Efficacy Data: Local Control Rate and Survival Rate
The outstanding advantage of heavy (carbon) ion therapy is its high local control (LC) rate. The one-year local control rate can reach 100%, and the response rate of heavy (carbon) ion therapy for chordoma is nearly 100%. Since chordoma is insensitive to conventional radiotherapy and is adjacent to vital organs, heavy ions, leveraging their dual physical and biological advantages, can deliver a radical dose to the tumor. For small chordomas (<5 cm) and those located in low-risk areas where nerve injury is less likely, surgery is also a good option. However, when chordomas are large and the risk of postoperative incontinence or loss of lower limb motor function is high, heavy ion therapy must be chosen. Heavy ion therapy is certainly effective for radical treatment of small chordomas, but for large tumors (e.g., 10–20 cm or larger), it demonstrates unique advantages and becomes an irreplaceable treatment option.
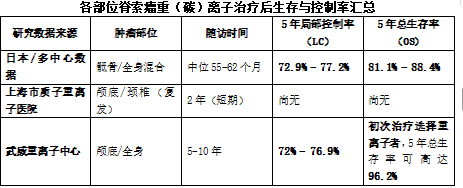
Key Interpretation:
Initial Treatment vs. Recurrence: Data show that for patients receiving initial treatment without prior radiotherapy, the 5-year overall survival rate can be as high as 96.2%. However, once surgery is performed and recurrence occurs, the efficacy significantly declines. For patients with postoperative recurrence or those undergoing a second course of radiotherapy, the survival rate drops markedly to approximately 50%. This highlights the critical importance of seizing the first treatment opportunity.
Long-term Control: For skull base chordoma, the 10-year local control rate can still be maintained at around 54%, demonstrating the long-term effectiveness of the therapy.
3.2 Safety: Manageable Toxicity and Adverse Effects
Compared with the risks associated with surgery—such as limb dysfunction and loss of bowel and bladder control—heavy (carbon) ion therapy is far less invasive.
Low Incidence of Severe Complications: In the aforementioned studies, the incidence of grade ≥3 severe complications (requiring hospitalization or surgical intervention) was low. For example, in a study involving 35 patients with sacral chordoma, only a few developed skin ulcers or infections (1 grade 4, 5 grade 3), and there were no treatment-related deaths.
Functional Preservation: In the treatment of skull base chordoma, although acute reactions such as headache and mucositis may occur, heavy ion therapy maximizes protection of the brainstem, optic nerves, and auditory pathways, thereby preserving neurological function. In the treatment of sacrococcygeal chordoma, it effectively preserves bowel and bladder function as well as lower limb motor function. Moreover, in patients who had pre-existing impairment of the cauda equina nerves or lower limb motor function before heavy (carbon) ion therapy, improvement was often observed after treatment.
3.3 Technological Advancements and Combination Therapy
Novel "Surgery + Heavy Ion" Strategy: For patients in whom the tumor border with the rectum or intestines is unclear (e.g., sacrococcygeal tumors), the Wuwei Center has pioneered the use of a SPACER technique. This involves a temporary surgical procedure to separate the rectum from the tumor using a gauze pad, after which heavy ion irradiation is delivered. The SPACER technique resolves the issue of being unable to deliver a full radical dose due to the tumor's proximity to the intestinal tract.
3.4 Summary and Recommendations
In summary, heavy (carbon) ion therapy demonstrates definitive and remarkable efficacy in the treatment of chordoma. It achieves a high local control rate (approximately 70–80% at 5 years) while effectively avoiding the severe functional impairments associated with surgery. It is particularly suitable for:
- Chordoma at any site, regardless of size. The more complex and larger the chordoma, the more irreplaceable heavy ion therapy becomes as a treatment option.
- Patients with chordoma located in anatomically complex regions with high surgical risk, such as the skull base and sacrum.
- Patients with postoperative residual or recurrent disease who are not candidates for repeat surgery.
- Patients who wish to preserve limb and organ function (e.g., defecation, urination, neurological function).
IV. Sharing of Typical Medical Cases
It has been three years since our first chordoma patient treated with heavy (carbon) ion therapy using the SPACER technique.
Patient Wang, female, 52 years old, Li minority. Diagnosis: Sacrococcygeal chordoma. Pre-treatment assessment: MRI showed partial bone destruction of the S2–S4 vertebral bodies. At the corresponding level, a mixed T1 and mixed long T2 mass lesion measuring approximately 8.8 × 7.1 cm (S6, I57) was observed, extending into the pelvic cavity with local invasion of the sacral canal and relatively clear borders. The lesion was adjacent to the colorectum over approximately 270 degrees of its circumference.
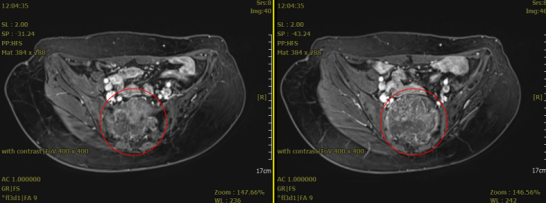
MRI examination before carbon ion therapy in March 2023; the red circle marks the tumor
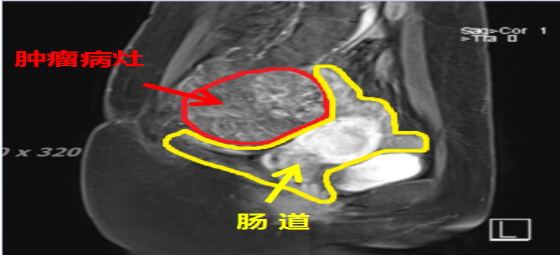
MRI examination before carbon ion therapy in March 2023; the red circle marks the tumor
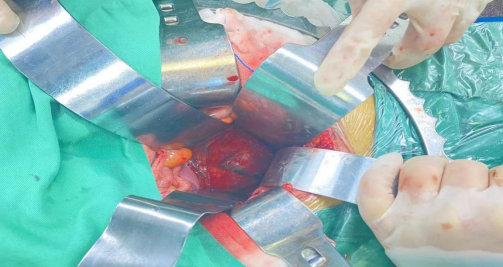
During the operation, gauze pads were placed between the tumor and the intestinal tract to separate and protect the intestines
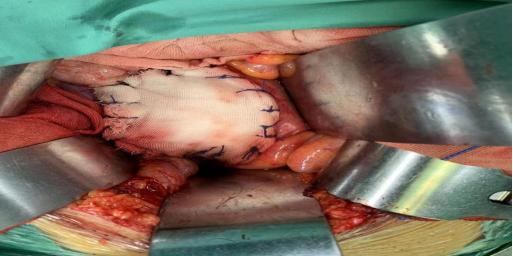
Insert a large gauze pad as an isolation material
For heavy (carbon) ion therapy target volume delineation, a spacer material was surgically placed between the tumor and the organs at risk. This provided sufficient distance between the target tumor and the surrounding normal tissues, thereby allowing an adequate radical dose to be delivered to the tumor.
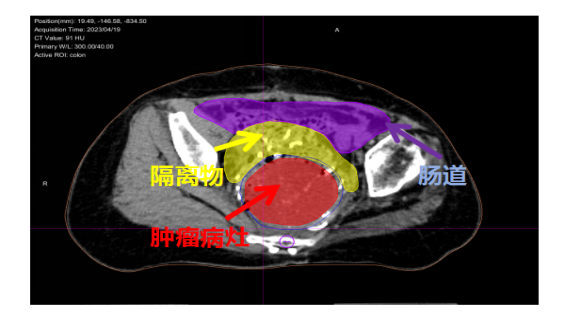
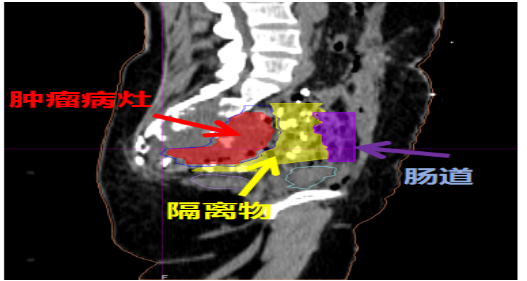
During the surgery, gauze pads were placed between the tumor and the intestinal tract to separate and protect the intestines, and heavy ion inactivation of the tumor was completed on the same day
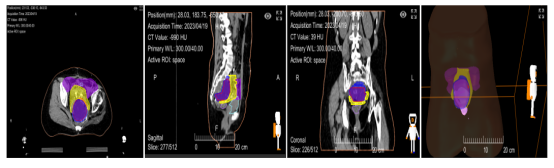
Target Volume Delineation: GTV - Red, Colon - Purple, Isolated Tissue - Yellow
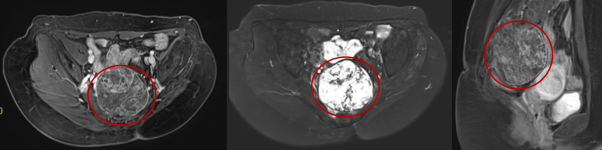
Before treatment, the tumor measured 8.8×7.1 cm. The left image is an axial T1-weighted MRI scan, the middle one is an axial T2-weighted scan, and the right one is a sagittal T1-weighted scan
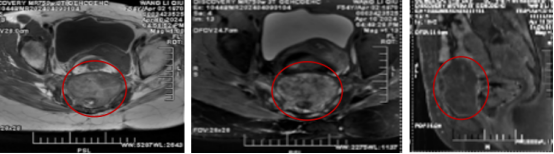
One year after treatment, the tumor measured 7.8×7.4 cm. The left image is an axial T1-weighted MRI scan, the middle image is an axial T2-weighted scan, and the right image is a sagittal T1-weighted scan
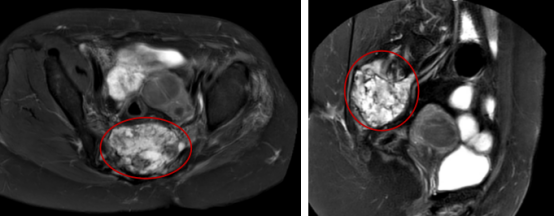
Two years after treatment, the tumor measured 7.5×5.3 cm. MRI: T2 axial view, T2 sagittal view
Three years after treatment, the tumor has continued to shrink and be absorbed. The patient's bowel and bladder functions, as well as motor function, have recovered very well. The pain was significantly relieved one year after treatment and has slowly disappeared.
Case provided by: Dr. Zhang Yanshan
Department: Radiation Oncology Center Ⅰ(International Medical Department Ⅰ)
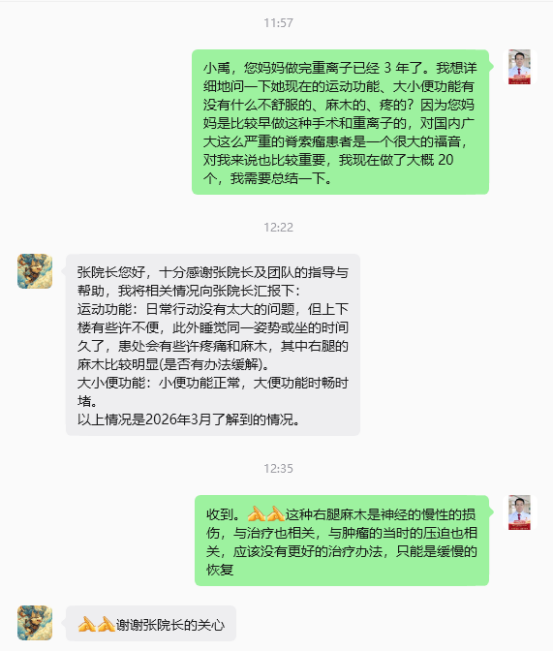
Summary of this case: The patient did not experience any toxic or side effects related to heavy (carbon) ion therapy. For patients who had pre-existing impairment of the cauda equina nerves or lower limb motor function before treatment, symptoms were often alleviated after treatment. This demonstrates the superiority of heavy (carbon) ion therapy in the field of chordoma treatment. Most of the chordoma cases treated at the Wuwei Center are challenging, and heavy ion therapy has successfully addressed them well! We thank the patient for her trust in our center and wish her continued improvement and well-being.
Contributors: Chen Xuelian, Li Pengqing (Cancer Registry and Follow-up Office)
Reviewed by: Zhang Yanshan (Vice President, Gansu Wuwei Cancer Hospital)
Date: April 1, 2026
Individual differences exist objectively.
Specific plans vary from person to person.
Gansu Wuwei Cancer Hospital (Wuwei Institute of Medical Sciences)
(Gansu) Medical Advertisement [2025] No. 11-14-387
