Heavy Ion Therapy: A "Ray of Hope" for Ovarian Cancer Patients in Desperation
Heavy Ion Therapy: A "Ray of Hope" for Ovarian Cancer Patients in Desperation
On the long and arduous journey of fighting cancer, every patient wages a tenacious battle against the disease. Ms. Chen, a courageous warrior in this fight, is no exception. Her experience is not only a legend of personal struggle against fate but also a beacon of new hope and inspiration for many ovarian cancer patients.
Nine Years of Fighting Cancer: A Road Filled with Challenges
In June 2015, 72-year-old Ms. Chen underwent surgery for a "pelvic mass" at a local hospital. Postoperative pathology diagnosed it as an endometrial fibroma with focal microinvasion. At the time, she likely had no idea that this was just the beginning of a long battle against cancer. In December 2018, the pelvic mass reappeared, and she underwent surgery at a top-tier hospital in her area. However, during the operation, the severity of her condition became apparent: the lesions were adhered to the surrounding intestines and ureters, forming a "frozen pelvis," rendering the surgery impossible. The procedure was aborted after exploratory surgery, and pathological examination of the ascites revealed the presence of tumor cells, indicating a worsening of her condition. Subsequently, the patient received conventional radiotherapy and chemotherapy, which stabilized her condition for a time.
Yet, the tenacity of cancer proved overwhelming. From May 2021 to January 2025, Ms. Chen's condition progressed again, with the lesions gradually enlarging. She underwent chemotherapy and targeted therapy, but the efficacy was evaluated as progressive disease (PD), meaning the tumors continued to spread relentlessly. By this point, Ms. Chen was suffering from severe physical discomfort and significant bone marrow suppression, leading to a therapeutic impasse that plunged her and her family into deep despair.
A Glimmer of Hope: Heavy Ion Therapy Brings New Possibilities
In this darkest hour, with no other treatment options and the tumors advancing unchecked, Ms. Chen learned about the Heavy Ion Therapy Center at Gansu Wuwei Cancer Hospital through the internet. In February 2025, she made the resolute decision to seek a final glimmer of hope at this hospital. After being admitted to the Department of Gynecological and Breast Oncology (Radiotherapy Department IV), pelvic MRI and PET/CT scans confirmed a recurrence of ovarian cancer. A vaginal biopsy pathology report diagnosed it as (vaginal stump tissue) endometrial adenocarcinoma.
Faced with this diagnosis, Director Dang Youquan and the gynecological oncology heavy ion therapy team swiftly formulated a personalized treatment plan, opting for the advanced technology of carbon ion therapy.
Carbon ion therapy is a cutting-edge radiotherapy technique based on a heavy ion accelerator. Heavy ions refer to charged particles heavier than alpha particles (helium nuclei), primarily carbon atomic nuclei. In heavy ion therapy, when carbon ion beams enter the human body, they lose minimal energy before reaching the tumor site. However, upon reaching the tumor, they suddenly release a large amount of energy, forming a peak known as the "Bragg peak." This unique physical property allows heavy ions to precisely deliver high doses of energy to the tumor tissue, delivering a powerful blow to the tumor while minimizing damage to surrounding healthy tissues.
Compared to conventional photon radiotherapy (such as X-ray radiotherapy), heavy ion therapy offers a higher relative biological effectiveness, more efficiently killing tumor cells by causing double-strand breaks in tumor DNA, leading to lethal damage. Additionally, its dose distribution in the depth direction of the tumor is more precise, better protecting critical organs and tissues around the tumor and reducing the risk of radiotherapy complications.
Remarkable Efficacy: A New Lease on Life
After undergoing carbon ion therapy, Ms. Chen's symptoms significantly improved. A follow-up pelvic MRI showed a noticeable reduction in the pelvic and vaginal stump masses, with the efficacy evaluated as partial response (PR)—an undeniably encouraging outcome. Once tormented by the pain of cancer, she now sees a glimmer of recovery. Following heavy ion therapy, Ms. Chen will continue medication based on her genetic test results. She and her family are deeply grateful to the medical staff at the Heavy Ion Therapy Center, expressing their heartfelt thanks through a sincere letter of appreciation and a vibrant banner.
Ms. Chen's successful treatment serves as a guiding light for many ovarian cancer patients. Ovarian cancer, one of the most common malignancies of the female reproductive system, often presents with subtle early symptoms, leading to late-stage diagnoses in most patients. The high difficulty of treatment and recurrence rate make it a formidable challenge. Traditional treatments such as surgery, chemotherapy, and radiotherapy often have limitations when dealing with recurrent or metastatic ovarian cancer. Heavy ion therapy, with its unique advantages, offers patients a novel and more effective treatment option.
For ovarian cancer patients and their families, it is crucial not to lose hope in the face of the disease. With continuous advancements in medical technology, cutting-edge treatments like heavy ion therapy are emerging. Actively seeking information, consulting multiple medical professionals, and finding the most suitable treatment plan may bring a turnaround in the most desperate situations. At the same time, we look forward to more research investments and technological innovations to provide cancer patients with greater chances of cure, allowing more lives to shine brightly in the fight against cancer.
Figure 1 (Pre-heavy ion radiotherapy MRI)
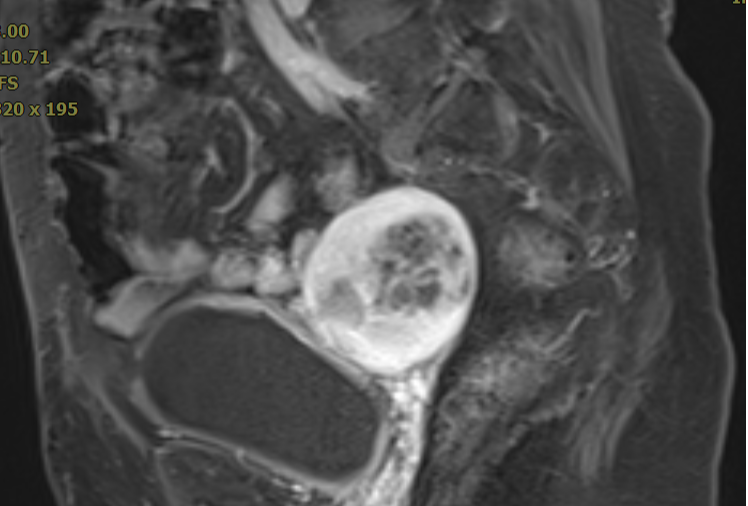
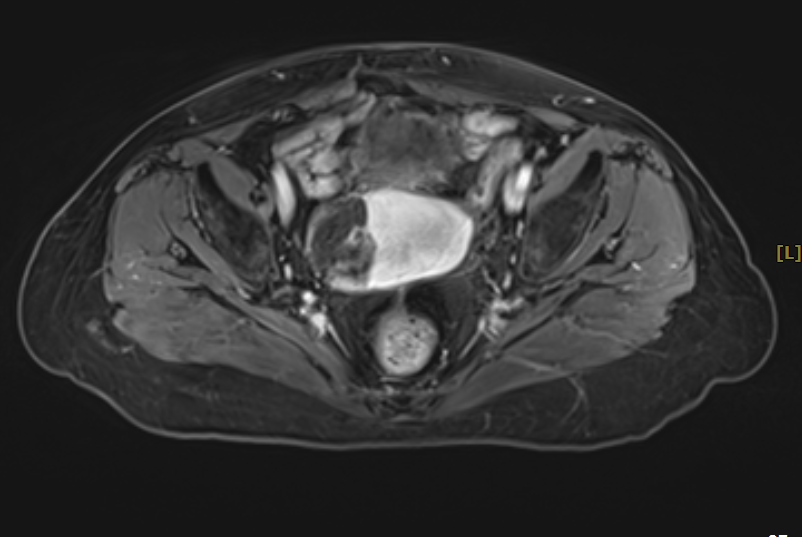
Pre-heavy ion radiotherapy MRI findings: Postoperative absence of the uterus. A cystic-solid mass measuring 8.7×5.9×5.8 cm is observed at the vaginal stump (right side of the pelvis), with localized diffusion restriction. The solid components and septa show significant enhancement on contrast scan, with indistinct boundaries between the vaginal stump and adjacent bowel.
Figure 2 (Post-heavy ion radiotherapy MRI)
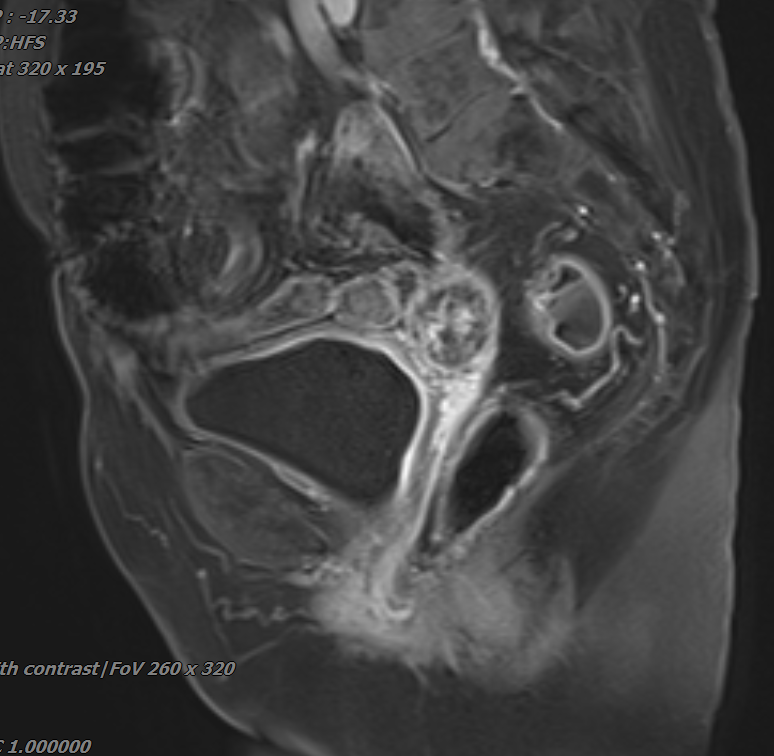
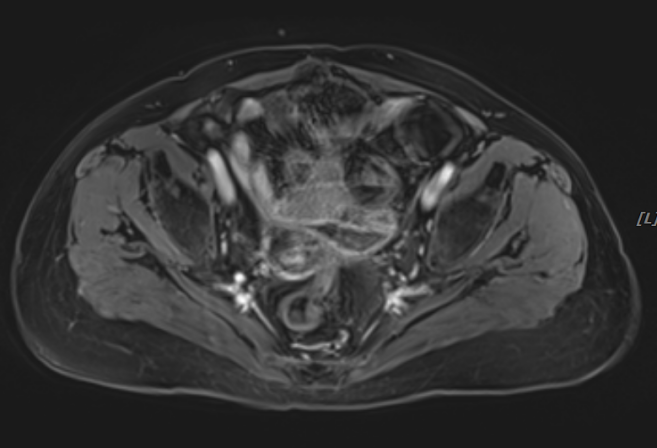
Post-heavy ion radiotherapy MRI findings: Absence of the uterus. A cystic-solid mass measuring 2.3×2.5×2.1 cm is observed at the vaginal stump (right side of the pelvis), with localized diffusion restriction. The solid components and septa show significant enhancement on contrast scan, with indistinct boundaries between the vaginal stump and adjacent bowel. The lesion has significantly reduced in size compared to previous imaging.
Figure 3 (1-month post-heavy ion radiotherapy MRI)
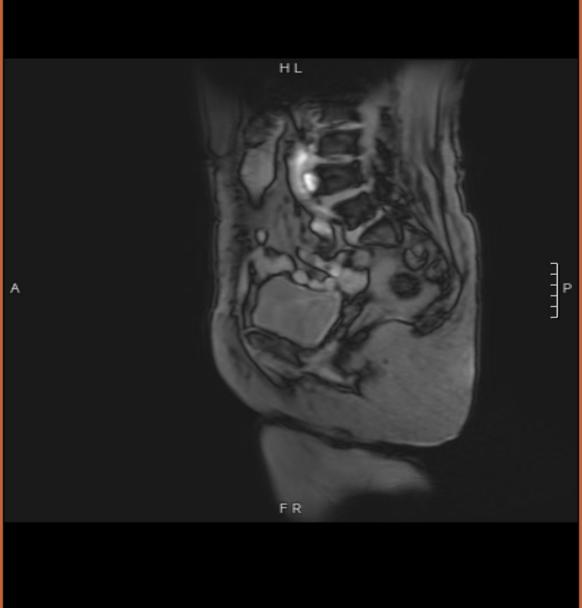
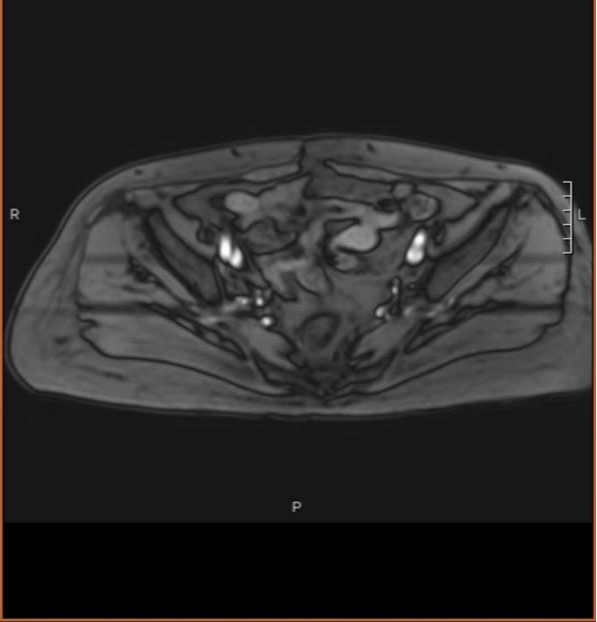
One-month follow-up MRI after heavy ion radiotherapy findings: Absence of the uterus. The vaginal stump exhibits mixed signals, with no diffusion restriction observed. No enlarged lymph nodes are detected in the pelvis.
Department Introduction
Radiotherapy Department IV specializes in photon and carbon ion therapy for gynecological and breast malignancies, including cervical cancer, endometrial cancer, vaginal cancer, vulvar cancer, ovarian cancer, and breast cancer. Treatment modalities include radical radiotherapy, neoadjuvant radiotherapy, postoperative adjuvant radiotherapy, chemotherapy, immunotherapy, targeted therapy, endocrine therapy, and comprehensive combinations of these approaches. The department has 13 medical staff, including 2 associate senior physicians, 1 attending physician, and 3 resident physicians. Team members have received advanced training at renowned institutions such as Tianjin Cancer Hospital, Beijing Cancer Hospital, PLA General Hospital (301 Hospital), Peking University Third Hospital, Shanghai Proton and Heavy Ion Center, and Sichuan Cancer Hospital.
The department director, Dang Youquan, is an associate chief physician with 24 years of experience in radiation oncology. He has trained at several top-tier hospitals nationwide and has profound expertise in radiotherapy and comprehensive treatment for gynecological and breast tumors. He currently serves as:
- Committee Member of the Ion Radiotherapy Branch, China Medical Equipment Association
- Executive Director of the Western Oncology Alliance
- Standing Committee Member of the Brachytherapy Committee, Gansu Anti-Cancer Association
- Committee Member of the Radiation Oncology Branch, Gansu Geriatrics Society
- Committee Member of the Oncology Nutrition Branch, Gansu Nutrition Society
- Part-time Lecturer at Wuwei Vocational College
The department collaborates with internationally renowned experts, including:
- Prof. Jörg Hauffe (Munich Proton and Heavy Ion Center, Germany)
- Prof. Hirohiko Tsujii (Pioneer of heavy ion cancer therapy, Japan)
- Prof. Yee-min Jen (Former Chairman of the Taiwan Radiation Oncology Committee)
Additionally, the department receives ongoing clinical and academic guidance from:
- Prof. Liu Zi (Chair of Gynecologic Oncology Committee, First Affiliated Hospital of Xi’an Jiaotong University)
- Prof. Li Sha (Chief Physician, Radiotherapy Department, PLA 940th Hospital)
The team has completed 5 provincial and municipal research projects, published over 10 papers, and holds 3 patents. The department offers advanced radiotherapy technologies, including:
- Heavy ion radiotherapy
- Image-guided radiotherapy (IGRT)
- Intensity-modulated radiotherapy (IMRT)
- Stereotactic radiotherapy (SRS/SBRT)
- 3D conformal radiotherapy (3DCRT)
- Volumetric modulated arc therapy (VMAT/RapidArc)
- 4D dynamic radiotherapy
- Painless 3D brachytherapy
- 3D-printed template-guided interstitial brachytherapy
- Bladder volume measurement-guided precision radiotherapy for gynecologic tumors
- Surface applicator therapy
- Preoperative/postoperative radiotherapy
- Radiotherapy for benign diseases
- External high-frequency hyperthermia
These cutting-edge techniques are integrated with surgery, chemotherapy, hyperthermia, molecular targeted therapy, immunotherapy, and traditional Chinese medicine to deliver evidence-based, multidisciplinary cancer treatment. Over the years, the department’s comprehensive oncology approach has achieved outcomes and earned widespread recognition from patients, peers, and society.

