[Expert Q&A] The silent killer in the human body — liver cancer
The silent killer in the human body — liver cancer
Currently, liver cancer ranks fourth in incidence among the many malignant tumors in China, and it has consistently held the second position in mortality rates for many years. This severe situation poses a significant threat to the life safety and health of the Chinese population.
Although experts in the field of hepatology have placed great emphasis on the early screening of liver cancer, unfortunately, the early diagnosis rate remains extremely low. This directly results in a mortality rate far exceeding that of other types of tumors. Delving into the reasons, a major factor is that liver cancer often lacks noticeable symptoms in its early stages, making it difficult for patients to detect through self-awareness, thereby missing the critical window for early treatment. This phenomenon underscores the importance of raising public awareness of early warning signs, strengthening regular screenings, and advancing diagnostic and therapeutic innovations.
Today, let us join Dr. Liang Chunhui, Director of the Second Hepatology Department at the Hepatobiliary Center of Gansu Wuwei Cancer Hospital, to explore and unveil the mysteries of the silent killer lurking within the human body—liver cancer. Under Dr. Liang’s professional guidance, we will gain a clearer understanding of the complexity and severity of liver cancer, working together to enhance public health awareness and contribute to early detection and treatment.

Q: Dr. Liang, why doesn’t early-stage liver cancer cause pain?
A: Viewers of Jiao Yulu are deeply moved by the scene where the protagonist uses a chair back to support his liver to alleviate the intense pain caused by liver cancer. However, it is important to clarify that not all liver cancer patient experiences liver-area pain. In fact, early-stage liver cancer often presents with a series of nonspecific, generalized symptoms, such as unexplained weight loss and fatigue, which can also appear in the early stages of various cancers and chronic wasting diseases, making them less indicative.
As for liver-area pain, while it is a hallmark symptom of liver cancer, in the early stages, this pain is often extremely mild or even imperceptible. Only when liver cancer progresses to an advanced stage, with the tumor significantly enlarging and compressing or invading surrounding tissues, does the pain become pronounced and hard to ignore. Therefore, for early detection and diagnosis of liver cancer, we cannot rely solely on the presence or absence of liver-area pain but must integrate multiple clinical indicators for comprehensive evaluation.
The pain characteristics of liver cancer can be summarized into two key points: First, pain typically does not accompany small liver cancer but becomes noticeable only when the tumor grows larger, entering the stage of large liver cancer. Second, the emergence of pain often signals increased treatment difficulty—when pain is absent, liver cancer may still be curable through timely intervention, but once pain appears, it usually indicates a more severe stage, making complete cure significantly harder.

Since the liver itself lacks direct pain-sensing nerves, when liver cancer is still in its tiny, intrahepatic growth phase, patients often feel no pain or discomfort. This stealthy nature makes regular health check-ups and follow-ups particularly crucial; otherwise, small liver cancer may silently grow unchecked.
When liver cancer enlarges significantly, especially exceeding 10 cm in diameter, its expansion not only alters the liver’s internal structure but also exerts strong tension on the liver capsule—the outer membrane of the liver. The liver capsule, which contains pain-sensing nerves, reacts to the stretching caused by the growing tumor much like an inflating balloon, where increasing surface tension leads to severe pain.
Regrettably, when such pain manifests due to tumor growth, it often marks the irreversible advanced stage of the disease. At this point, large liver cancer presents far greater treatment challenges and poorer prognoses compared to early-stage small liver cancer. Hence, emphasizing the importance of regular check-ups aims to encourage early detection and intervention, thereby improving treatment success rates and patient quality of life.
Q: Dr. Liang, what are the high-risk factors for liver cancer?
A: The high-risk factors for liver cancer mainly include the following:
Hepatitis B virus (HBV) infection: HBV is a major risk factor for liver cancer. Its pathogenic mechanisms involve two aspects: First, HBV can integrate into the genome of human liver cells. If this integration occurs in regions that activate oncogenes or suppress tumor suppressor genes, it may trigger liver cancer. Second, recurrent hepatitis B leads to progressive liver fibrosis, eventually developing into cirrhosis. In the cirrhotic stage, disordered liver cell growth increases the risk of malignant transformation, culminating in liver cancer.
Chronic excessive alcohol consumption: Alcohol is another proven liver-damaging factor, capable of independently causing cirrhosis and liver cancer. Studies show that men consuming over 40 grams of alcohol daily (half for women) for five years face the risk of alcoholic liver disease. Without timely intervention, this can progress to cirrhosis and liver cancer, severely threatening life.

Forty grams of alcohol may sound negligible, but it equates to roughly 100 ml of 50-proof liquor or two bottles of beer—enough to pose a latent threat to the liver. Therefore, abstaining from alcohol is not only a key skill for liver protection but also a necessary choice for a healthy life. Ideally, one should avoid alcohol entirely; if unavoidable, limit consumption to special occasions, such as social gatherings, and avoid drinking alone—a practice reflecting self-discipline and respect for health.
Obesity: Fatty liver has become an extremely common liver disease in urban China, with a prevalence of 20–30%, far exceeding hepatitis B and posing a significant health hazard. The cause of fatty liver is straightforward—excessive intake and insufficient exercise lead to fat accumulation. This not only affects physical appearance but also primarily harms liver health, causing fatty liver. Notably, even if risks like cardiovascular disease and diabetes due to obesity are controlled, fatty liver can still worsen into cirrhosis and liver cancer. More critically, there is currently no targeted pharmacological treatment for fatty liver. with weight loss being the primary non-pharmacological approach. Thus, maintaining a healthy weight, balanced diet, and increased exercise are vital for preventing and treating fatty liver and protecting the liver from liver cancer.
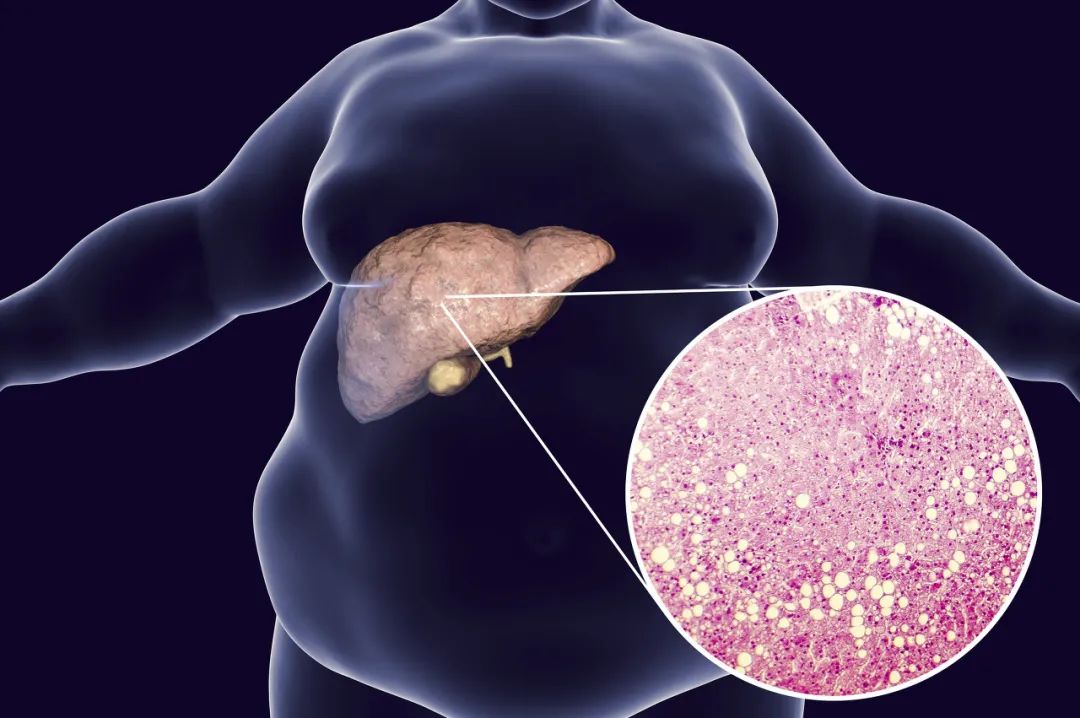
Aflatoxin contamination: Aflatoxin, especially its highly toxic variant B1, is a recognized potent carcinogen targeting liver cells. It can induce DNA misrepair, leading to severe mutations and increasing liver cancer risk. In-depth epidemiological studies in China reveal a sobering correlation: in certain regions, the level of aflatoxin contamination in diets is significantly positively associated with the incidence of primary liver cancer, further cementing aflatoxin’s role as a major trigger for liver cancer.
As early as 1993, the WHO’s cancer research agency classified aflatoxin as a Group 1 carcinogen, authoritatively recognizing its natural occurrence and extreme toxicity. Aflatoxin widely contaminates grain, oil, and their processed products, including but not limited to peanuts, peanut oil, corn, rice, and cottonseed—common staples in daily life. Thus, strengthening monitoring and control of aflatoxin and reducing its presence in the food chain are invaluable for preventing liver cancer and safeguarding public health.
Q: Dr. Liang, how can liver cancer be detected early?
A: So-called early-stage liver cancer typically refers to the initial phase of the disease where patients show no obvious symptoms, and only through meticulous imaging can a single liver cancer lesion smaller than 3 cm in diameter be detected. At this stage, thanks to its small size and localized focus, liver cancer has high curative potential. Through surgical resection or minimally invasive radiofrequency ablation, early-stage liver cancer can often be radically removed or ablated, completely eliminating the lesion.
For patients who undergo appropriate radical surgery, their future life expectancy and quality of life can be restored to levels comparable to those without liver cancer, achieving near-complete health recovery. Therefore, regular follow-ups are particularly important for high-risk groups. This not only aids in detecting tiny liver cancer lesions early but is also the most effective way to achieve early intervention, radical cure, and ensure long-term quality of life.
When liver cancer is still in its minuscule stage, the human body often cannot perceive its presence. Thus, for high-risk groups, regular screenings are key to early detection of small liver cancer. Currently, the most efficient, reliable, and cost-effective screening strategy is a combination of liver ultrasound and alpha-fetoprotein (AFP) blood testing every six months. This dual approach can accurately detect small liver cancer lesions about 1 cm in diameter, with a detection rate of 60–70%, providing a valuable opportunity for early intervention.
Notably, if either the ultrasound or AFP levels show abnormalities during screening, further action—such as PET-CT or contrast-enhanced MRI—should be taken immediately. These advanced imaging techniques, as the gold standard for early liver cancer diagnosis, can more precisely reveal lesions, buying precious time for timely treatment. In summary, through regular screenings and a scientific diagnostic process, we can more effectively detect and address small liver cancer, improving treatment outcomes and patient survival rates.
Q: Dr. Liang, how can liver cancer be prevented?
A: Regular health check-ups are essential. Combining serum AFP testing with liver ultrasound is currently the most economical and effective early screening strategy for liver cancer. For high-risk individuals, it is recommended to undergo such comprehensive check-ups at least every six months to achieve early detection, diagnosis, and treatment.
Maintain a balanced diet for health. In daily meals, reduce intake of pickled foods like salted vegetables, which may contain high salt levels and potential harmful substances. Strictly avoid moldy foods, as they harbor potent carcinogens. Additionally, quitting smoking and limiting alcohol are crucial measures for liver health, as the harm from tobacco and alcohol cannot be overlooked.
Get vaccinated proactively. The hepatitis B vaccine is an effective way to prevent HBV infection and its potential chronic diseases, including liver cancer. Vaccination significantly reduces the risk of HBV infection, building a solid defense for personal health.
Summary
Liver cancer is a malignant tumor caused by multiple factors (e.g., hepatitis B, alcohol, obesity, aflatoxin). High-risk individuals should undergo liver ultrasound and AFP testing every six months for early detection and treatment. Single liver cancer lesions smaller than 3 cm in diameter can be radically cured through surgery.

The Hepatobiliary Center of Wuwei Medical Science Institute has been designated as a National Model Base for Hepatobiliary Disease Prevention and Treatment Technologies. As a comprehensive specialty center, it provides:
• Therapeutic interventions: liver-protective regimens, antiviral treatments, artificial liver support systems
• Surgical solutions: conventional and minimally invasive surgeries, interventional therapies, radioactive iodine-125 seed implantation
• Advanced therapies: targeted immunotherapy, cellular immunotherapy, and stem cell transplantation
As one of China's few dedicated hepatobiliary centers, it offers:
✓ Integrated diagnostic services
✓ Multimodal treatment approaches
✓ Whole-process disease management
The center's achievements include:
• Leading multiple real-world clinical studies
• Implementing national healthcare accessibility initiatives
• Establishing Gansu's inaugural Joint Diabetes-Liver Disease Management Center
• Creating an international consultation platform for refractory hepatobiliary cases
Clinic Locations
Main Hospital Campus (Downtown Area):
- Vice President Zhang Wenhua's Clinic:
- Hepatology Department Clinics:
- Hepatobiliary Surgery II Department Clinic:
Heavy Ion Therapy Campus:
- Hepatology Department Clinics:
- Hepatobiliary Surgery II Department Clinic:
- Other Physician Offices:
Note: For detailed consultation schedules, please refer to the official duty roster.
Contact Information
- Head Nurse Zhou Ziying: 189-0395-7717
- Head Nurse Yang Lixia: 138-0935-6120
- Head Nurse Zhang Xiaoyan: 136-3935-9127
