Heavy Ion Therapy: A "Ray of Hope" for Ovarian Cancer Patients in Desperation
Heavy Ion Therapy: A "Ray of Hope" for Ovarian Cancer Patients in Desperation
On the long and arduous journey against cancer, every patient is engaged in a tenacious battle against the disease. Ms. Chen is one such brave warrior in this fight. Her experience is not only a legendary tale of an individual's struggle against fate but also brings new hope and inspiration to many patients battling ovarian cancer.
A nine-year battle against cancer, shadowed by unrelenting hardships
In June 2015, 72-year-old Ms. Chen underwent surgery at a local hospital after being diagnosed with a "pelvic mass." Postoperative pathology confirmed the diagnosis of endometrioid fibroma with focal microinvasion. At the time, she likely never imagined this would only mark the beginning of a long and arduous battle against cancer. In December 2018, the pelvic mass reappeared, prompting another surgery at a local top-tier tertiary hospital. However, the operation revealed severe disease progression—the lesion had adhered to surrounding intestinal tracts and the ureter, forming a frozen pelvis that rendered surgical removal impossible. The surgeons had no choice but to close the abdomen after exploration. Pathological examination of the ascitic fluid detected tumor cells, signaling a clear deterioration of her condition. Subsequently, Ms. Chen underwent conventional radiotherapy and chemotherapy, which initially stabilized her condition for a period. Yet, the tenacity of cancer proved far beyond anticipation. From May 2021 to January 2025, her condition worsened again—the lesion gradually enlarged. She endured further rounds of chemotherapy and targeted therapy, but the efficacy assessment indicated progressive disease (PD), with the tumors continuing their relentless spread. By this point, Ms. Chen’s body was already suffering severely from profound bone marrow suppression, and treatment had reached a bottleneck. This plunged her and her family into deep despair.
Just as all hope seemed lost, carbon ion therapy brought a glimmer of renewed hope
In the darkest moments of her journey—when endless medical consultations yielded no results and the tumor continued its relentless progression—Ms. Chen learned about the Heavy Ion Therapy Center at Wuwei Cancer Hospital in Gansu Province through online research. In February 2025, she resolutely traveled to this hospital, seeking a final glimmer of hope. After admission to the Department of Gynecology and Breast Tumors (Radiotherapy Ward 4), pelvic MRI and PET/CT scans confirmed the recurrence of ovarian cancer, while a vaginal biopsy pathology report identified (vaginal stump tissue) endometrioid adenocarcinoma. Faced with this critical diagnosis, the heavy ion therapy team for gynecological cancers, led by Director Dang Youquan of Radiotherapy Ward 4, swiftly formulated a personalized treatment plan—opting for the advanced technique of carbon ion therapy.
Carbon ion therapy is an advanced radiation treatment technology based on heavy ion accelerators. Heavy ions are charged particles heavier than alpha particles (helium nuclei), primarily referring to carbon nuclei. In carbon ion therapy, as the carbon ion beam enters the human body, it loses minimal energy until reaching the tumor site, where it suddenly releases a concentrated burst of energy, creating an energy peak known as the "Bragg peak." This unique physical property enables carbon ions to precisely deliver high-dose radiation directly to the tumor tissue, delivering a powerful destructive effect while minimizing damage to surrounding healthy tissues. Compared to conventional photon radiotherapy (such as X-ray therapy), carbon ion therapy offers superior relative biological effectiveness, enabling more efficient destruction of tumor cells by inducing double-strand breaks in their DNA, resulting in lethal damage. Additionally, its dose distribution along the depth of the tumor is more precise, providing better protection for critical organs and tissues near the tumor while significantly reducing the risk of radiation-induced complications.
The treatment yielded remarkable results, giving her a new lease on life
After undergoing carbon ion therapy, Ms. Chen experienced significant relief from her symptoms. Follow-up pelvic MRI scans revealed marked shrinkage of the pelvic and vaginal stump masses, with efficacy assessment confirming a partial response (PR) - an undeniably encouraging outcome. The woman who had once suffered terribly from cancer now saw a beacon of hope for recovery. Following carbon ion therapy, Ms. Chen continued taking medication based on her genetic test results. Both she and her family expressed deep gratitude to the medical staff at the Heavy Ion Therapy Center. Through a heartfelt thank-you letter and a brightly colored banner, she conveyed her profound appreciation.
Ms. Chen's successful treatment serves as a shining example for many ovarian cancer patients. As one of the most common malignant tumors of the female reproductive system, ovarian cancer often presents with no obvious early symptoms, leading to late-stage diagnosis in most patients and posing significant treatment challenges with high recurrence rates. Traditional treatments like surgery, chemotherapy, and radiation therapy often have limitations when dealing with recurrent or metastatic ovarian cancer. Carbon ion therapy, with its unique advantages, offers a new and more effective treatment option for these patients.
For ovarian cancer patients and their families, facing the disease should never mean giving up hope. In this era of rapid medical advancements, cutting-edge technologies like carbon ion therapy are continually emerging. Actively seeking information, consulting multiple medical experts, and finding the most suitable treatment plan may turn desperation into opportunity. At the same time, we look forward to more research investment and technological innovation that could bring greater chances of cure for cancer patients, allowing more lives to shine brightly in their battle against this disease.
Figure 1 (MRI before heavy ion radiotherapy)
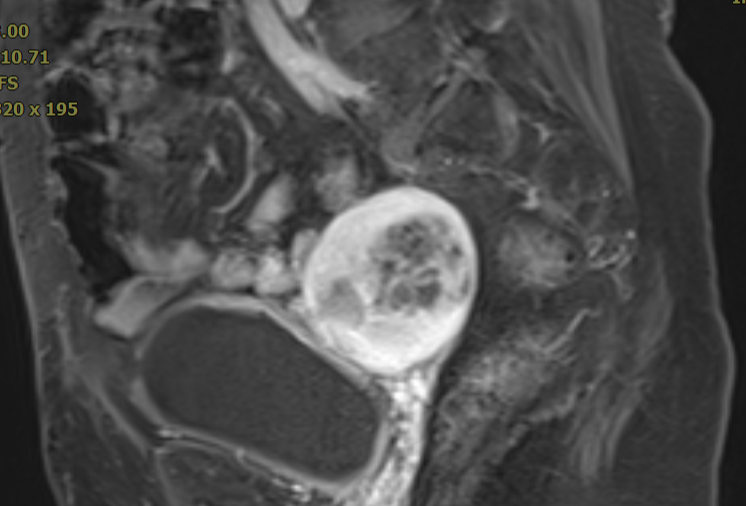
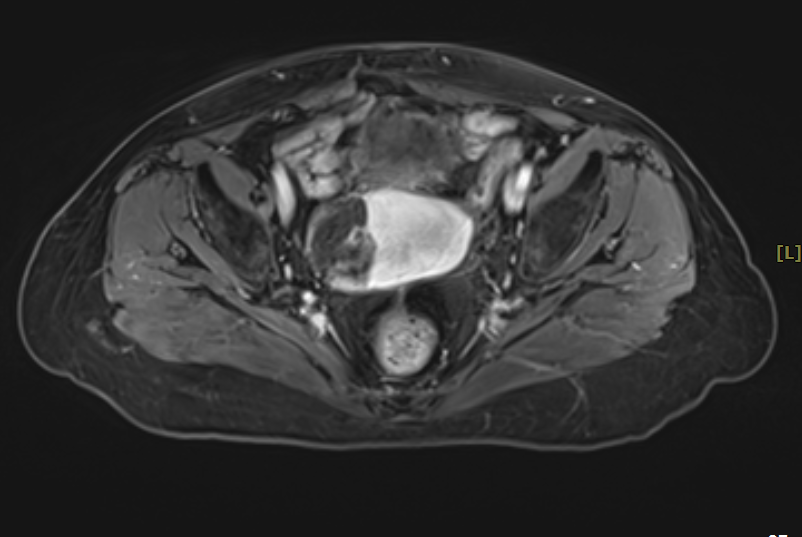
Pre-heavy ion radiotherapy MRI showed: absent uterus post-surgery, with an 8.7×5.9×5.8 cm cystic-solid mass located at the vaginal stump (right pelvic side). The mass exhibited restricted diffusion locally, with marked enhancement of the solid components and septations on contrast-enhanced scan. The mass demonstrated indistinct margins with the vaginal stump and adjacent intestinal loops.
Figure 2 (MRI after heavy ion radiotherapy)
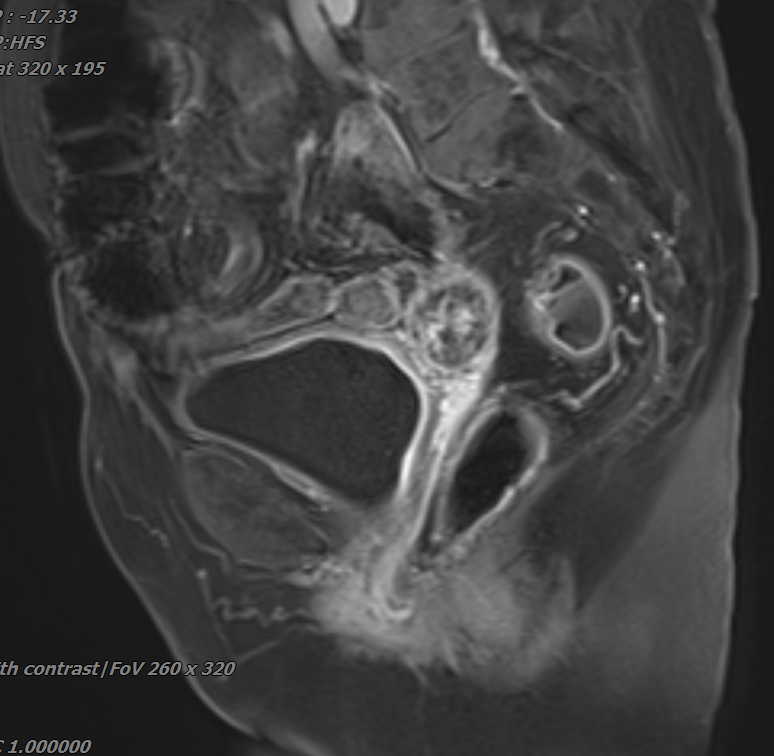
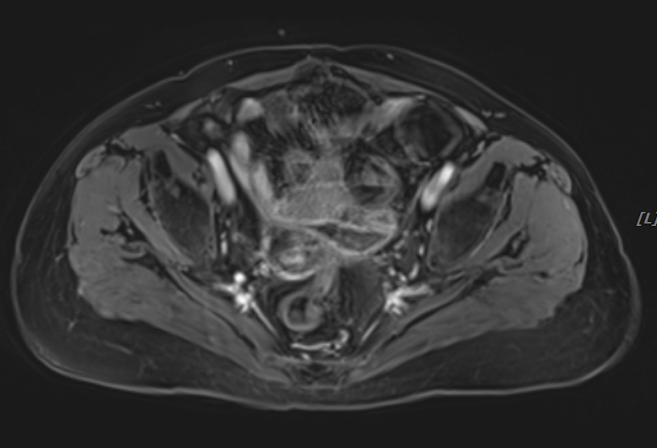
Post-heavy ion radiotherapy MRI revealed: absent uterus, with a 2.3×2.5×2.1 cm cystic-solid mass at the vaginal stump (right pelvic side) showing localized restricted diffusion, marked enhancement of solid components and septations on contrast-enhanced scan, and indistinct margins with the vaginal stump and adjacent intestinal loops. The lesion demonstrated significant size reduction compared to previous imaging.
Figure 3 (MRI at 1-month follow-up after heavy ion radiotherapy)
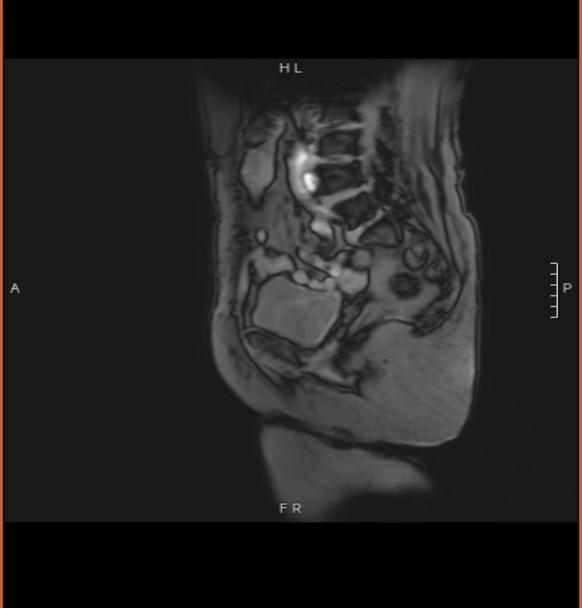
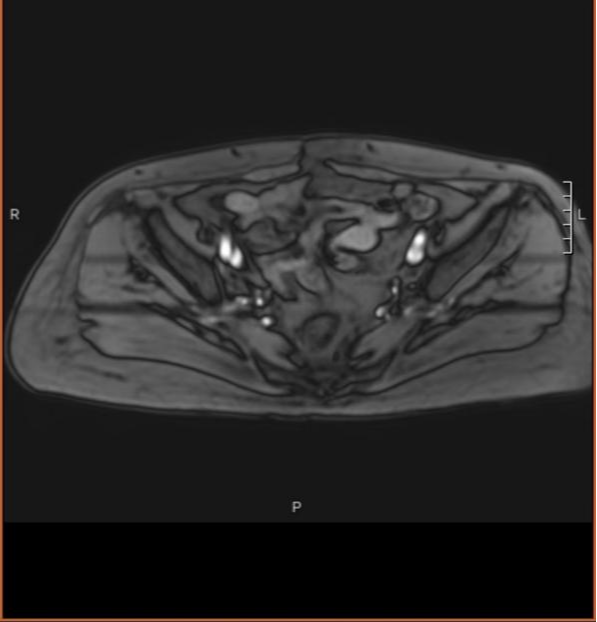
Post-heavy ion radiotherapy one-month follow-up MRI findings: absent uterus, heterogeneous signal intensity at the vaginal stump, no evidence of restricted diffusion, and no enlarged lymph nodes in the pelvic cavity.
Department Introduction
The Department of Radiotherapy IV specializes in photon and carbon ion therapy for gynecological and breast malignancies, with key disease types including cervical cancer, endometrial cancer, vaginal cancer, vulvar cancer, ovarian cancer, and breast cancer. The department offers comprehensive treatment modalities such as radical radiotherapy, neoadjuvant radiotherapy before surgery, adjuvant radiotherapy after surgery, chemotherapy, immunotherapy, targeted therapy, endocrine therapy, and combined approaches of these treatments. The department has a team of 13 medical professionals, comprising 2 associate senior-level physicians, 1 attending physician, and 3 resident physicians. Department staff have received advanced training at Tianjin Cancer Hospital, Beijing Cancer Hospital, PLA General Hospital (301 Hospital), Peking University Third Hospital, Shanghai Proton and Heavy Ion Center, and Sichuan Cancer Hospital.
Dang Youquan, Associate Chief Physician and Director of the department, has 24 years of experience in tumor radiotherapy. She has completed advanced training at multiple renowned top-tier hospitals across China and possesses extensive expertise in radiotherapy and comprehensive treatment for gynecological and breast cancers, demonstrating profound professional accomplishment. Currently, she serves as a committee member of the Ion Radiotherapy Branch of the China Medical Equipment Association, executive director of the Western Cancer Specialty Alliance, standing committee member of the Brachytherapy Committee under the Gansu Anti-Cancer Association, committee member of the Radiotherapy for Elderly Patients Committee of the Gansu Geriatrics Medical Association, committee member of the Oncology Nutrition Branch of the Gansu Nutrition Society, and part-time instructor at Wuwei Vocational College.
The department regularly invites Professor Jorg Hauffe from the Munich Proton and Heavy Ion Therapy Center in Germany, Professor Hirohiko Tsujii—renowned as the "father of heavy ion radiotherapy"—and Professor Yee-Min Jen, former chairman of the Taiwan Radiation Oncology Society, for ward rounds and clinical guidance. The department also receives ongoing support from Professor Liu Zi, director of the Gynecologic Oncology Committee at the First Affiliated Hospital of Xi'an Jiaotong University, and Professor Li Sha, chief physician of the Radiotherapy Department at the 940th Hospital of the Joint Logistic Support Force, in clinical practice and research education. The department has completed five provincial and municipal research projects, published over ten papers, and obtained three invention patents. Currently, it offers a full range of advanced radiotherapy techniques including heavy ion radiotherapy, IGRT, IMRT, stereotactic radiotherapy (SRS/SBRT), 3D conformal radiotherapy, VMAT/RapidArc, four-dimensional dynamic radiotherapy, painless brachytherapy, 3D-printed interstitial brachytherapy, bladder volume measurement-guided precision radiotherapy for gynecological cancers, contact therapy, preoperative and postoperative radiotherapy, radiotherapy for benign diseases, and external deep hyperthermia. These cutting-edge technologies are integrated with surgery, chemotherapy, hyperthermia, molecular targeted therapy, immunotherapy, and traditional Chinese medicine to form a comprehensive, evidence-based treatment model. This multimodal approach has achieved remarkable clinical outcomes, earning widespread recognition from patients, peers, and the medical community.

