Bone Metastasis in Cancer: What You Need to Know
Bone Metastasis in Cancer: What You Need to Know
Bone metastasis refers to the process where malignant tumors (such as lung cancer, breast cancer, etc.) invade the circulatory system from their primary site and subsequently spread to bone tissue through blood flow, causing infiltration. This represents a severe disease condition. Bone metastasis is particularly common in patients with malignant tumors such as lung cancer, prostate cancer, kidney cancer, and breast cancer, primarily affecting the spine and pelvic regions. Clinically, patients typically present with persistent pain at the affected site that gradually worsens and is difficult to relieve. In advanced stages, local masses, functional impairment, and even pathological fractures may occur. When spinal metastasis occurs, the tumor itself or accompanying pathological fractures may compress the spinal cord or nerve roots, leading to symptoms such as limb pain and weakness. In severe cases, this may progress to paralysis and bowel/bladder dysfunction - a series of serious symptoms.
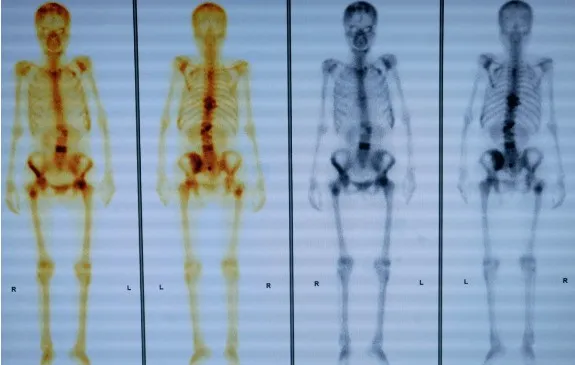
In advanced cancer patients, extensive bone metastases and refractory bone pain represent the most prevalent yet challenging clinical issues. With continuous optimization of diagnostic technologies and gradual improvement in treatment standards for malignant tumors, comprehensive therapeutic strategies for bone metastases have garnered increasing attention.
Mechanism of Radionuclide Therapy for Bone Metastases
Cancer cells infiltrate bone metastatic sites, causing osteolytic destruction while triggering abnormally active osteoblastic repair. Bone-seeking radiopharmaceuticals accumulate preferentially in these metabolically hyperactive regions, with significantly lower uptake in normal bone tissue. This selective concentration around tumor foci allows targeted irradiation via radionuclide emissions, achieving both analgesic effects and tumoricidal outcomes.
Taking strontium-89 (⁸⁹Sr) as an example, it is a highly bone-seeking radionuclide that belongs to the same main group of elements as calcium. After entering the human body, ⁸⁹Sr participates in bone mineral metabolism similarly to calcium. When administered intravenously, ⁸⁹Sr accumulates in bone metastasis lesions at concentrations 2 to 25 times higher than in normal bone tissue, and remains in cancerous foci for an extended period. The radionuclide persists in bone tumor lesions for approximately 100 days, during which time it emits β-radiation to kill cancer cells and shrink lesions, thereby providing excellent analgesic effects. Notably, the effective range of this radiation in tissue is only 2.4 mm, ensuring minimal damage to surrounding normal tissues or organs. This selective localization and limited radiation range make ⁸⁹Sr an effective and targeted therapeutic option for bone metastases.
Advantages of Radionuclide Therapy for Bone Metastases
Currently, the main treatment modalities for metastatic bone tumors include external beam radiation therapy (radiotherapy), chemotherapy, surgical intervention (lesion resection), and analgesic medications. However, each of these approaches has certain limitations. For instance, surgical procedures and radiotherapy often prove ineffective against widespread bone metastases; chemotherapy may induce adverse reactions such as nausea, vomiting, and cytopenia in patients; while prolonged use of analgesics carries a risk of drug dependence. In contrast, radionuclide therapy for bone metastases demonstrates superior advantages in multiple aspects. This treatment modality offers relatively simple administration procedures, exhibits strong target specificity, shows no significant myelosuppressive effects, and is associated with fewer adverse reactions. The targeted nature of radionuclides allows for concentrated therapeutic effects on metastatic lesions while minimizing damage to healthy tissues, representing a more precise and tolerable approach for managing disseminated bone metastases.
Is Radionuclide Therapy Safe?
Radionuclide therapy for bone metastases offers multiple advantages. Firstly, the radiation dose is relatively low. Since radionuclides can precisely target and distribute in the lesion sites while being scarcely absorbed by normal, non-lesioned tissues, radiation exposure to healthy tissues is minimized. Secondly, the therapeutic radionuclides emit short-range radiation, which prevents radioactive damage to surrounding normal tissues and organs. Additionally, radionuclides possess strong ionization capability, enabling effective destruction of tumor cells and thereby achieving excellent therapeutic outcomes.
Preprocedural Preparation for Radionuclide Therapy
Prior to radionuclide therapy for bone metastases, chemotherapy or radiotherapy should be discontinued for at least 6 weeks to prevent myelosuppression. Concurrently, bisphosphonate medications must be stopped for 2 days, and supportive care should be provided to the patient. Additionally, the patient's height and weight should be measured, along with bone scintigraphy, X-ray examinations, and pathological tests being performed. Within 7 days post-treatment, complete blood count, liver/kidney function tests, electrolyte panels, and enzymatic assays should be conducted. During the 8-week period following treatment, whole-body bone scintigraphy should be performed to observe radionuclide uptake in metastatic sites, with quantification of the radiopharmaceutical uptake rate. Important contraindication: Radionuclide therapy is generally not recommended for patients with a life expectancy of less than 4 weeks.
Department Introduction
The Department of Nuclear Medicine was founded in 1998 and is the first nuclear medicine department in Wuwei. Now it has developed into a clinical discipline that fully meets the scale requirements and business needs of tertiary hospitals. At present, the department has developed into a comprehensive department with more complete business development in our province, integrating nuclear medicine imaging diagnosis (SPECT, PET/CT), nuclear therapy, in vitro detection and analysis, and thyroid specialist clinic.
Radionuclide Therapy Services Offered by the Department
1. Iodine-131 (¹³¹I) Therapy for Hyperthyroidism & Differentiated Thyroid Cancer, precision targeting, pathogen elimination, renewed vitality. Lodine-131 (¹³¹I) is a radioactive isotope of iodine that is specifically taken up by thyroid tissue. Functioning like a "precision-guided missile," it delivers targeted β-radiation to locally destroy thyroid cells, making it an effective treatment for both hyperthyroidism and thyroid cancer.
2. Strontium-89 (⁸⁹Sr) Therapy for Skeletal Metastases, precision targeting, multimodal efficacy, metastasis control. Strontium-89 (⁸⁹Sr) is a bone-seeking radionuclide that, akin to possessing "precision navigation," selectively accumulates in bone metastatic lesions. It continuously emits β-rays to deliver localized irradiation, damaging cancer cells' DNA and other critical structures while inhibiting their proliferation. This achieves the therapeutic goals of alleviating bone pain and controlling local tumor progression, with minimal impact on surrounding healthy tissues—truly embodying "targeted precision" in combating bone metastases.
3. 90Sr (strontium)-90Y (yttrium) application for the treatment of keloids and hemangiomas, continuous nuclear force, close to health, mysterious skin beauty container. It mainly treats skin scars, hemangiomas, vulvar white shifts, scabs, lichen planus, pterygium, etc. The 90Sr nuclide application can precisely target the lesion skin area, and the range of radiation is relatively concentrated, just like customizing an exclusive "treatment circle" for skin diseases, minimizing the "accidental injury" to the surrounding healthy skin and ensuring the accuracy and effectiveness of the treatment.
4. 90Sr (strontium)-90Y (yttrium) for the treatment of prostatic hyperplasia and hypertrophy, "Precision Nuclide, Targeted Attack" unlocks new health possibilities for patients with prostatic hyperplasia! Like an invisible scalpel, it is a blessing for elderly patients with prostatic hyperplasia and enlargement.
5. Lodine 125 particle implantation for the treatment of various tumors, "iodine" brightens the anti-cancer pathway, and 125 iodine interventional therapy opens a new chapter of precision treatment for tumor patients. For all kinds of solid tumors, it is like a small but powerful "smart bomb", which irradiates tumor cells at close range and continuously, just like launching a silent but lethal "battle" in the tumor "base camp", by destroying the DNA structure of tumor cells, inhibiting the proliferation and differentiation of tumor cells, and eventually leading to the death of tumor cells, so as to achieve the purpose of treating tumors while minimizing radiation damage to surrounding normal tissues.

131 iodine medication window

Drug dispensing system

Drug injection area
The Department to Carry out Diagnostic Projects
SPECT/CT - the "insight" of precision medical imaging diagnosis, integrating images and accurate insights to escort your health diagnosis. SPECT (Single Photon Emission Computed Tomography) is a imaging technique that uses radionuclide-labeled tracers to detect the single photons emitted in the body to reflect the function and metabolism of tissues and organs. CT (computed tomography) is a tomography scan of the human body based on X-rays, which can clearly show the morphology, density and other anatomical information of the human tissue structure. SPECT/CT perfectly integrates these two powerful technologies to realize the integration of functional metabolic imaging and anatomical structure imaging, just like equipping doctors with a pair of "discerning eyes", which can not only see the "appearance" of internal tissues and organs of the body, but also understand their functional status, so that diseases can not be hidden.
1. 99mTc-MDP SPECT/CT whole-body bone scintigraphy, accurately locate tumor metastases, perform tumor staging, efficacy evaluation and guide treatment plans.
2. SPECT/CT whole-body iodine 131 imaging, exploring the body, accurately gaining insight into the traces of diseases, iodine lighting the beacon of health, so that diseases have nowhere to hide. It is possible to determine the functional status of the thyroid gland and whether there are abnormalities such as metastatic lesions, just like following the "light" to find the "treasures" or "hidden dangers" hidden in the body. Based on the whole-body iodine-131 scintigraphy, the development of a personalized treatment plan is like lighting a beacon for subsequent treatment, guiding the right direction.
3. 99mTc-MIBI SPECT/CT myocardial perfusion imaging, insight into myocardium, accurate detection of the 'heart', and "perspective glass" to protect heart health. It can clearly reveal the function and blood perfusion of myocardium, and provide a key basis for early diagnosis, disease evaluation and treatment plan formulation of heart diseases.
4. 99mTc-DTPA SPECT/CT renal dynamic imaging explores the "image window" of kidney function, accurately presents the mystery of the kidney, and protects your urinary health. It can intuitively analyze the blood perfusion, glomerular filtration function, renal tubular secretion function and urinary tract patency of the kidney, etc., to help doctors fully understand the physiological state of the kidney and whether there are lesions.
5. SPECT/CT thyroid scintigraphy, insight into the thyroid gland, the "image eye" of endocrine health, accurately present the thyroid state, and escort your endocrine health. It can clearly show the morphology, function and lesions of the thyroid gland, and provide a strong basis for the diagnosis, treatment and monitoring of thyroid diseases.
6. SPECT/CT parathyroid scintigraphy, accurately explore the "health code of parathyroids", unlock the mystery of parathyroids, and protect blood calcium balance and health. It can show the location, shape, size and functional status of the parathyroid glands, which is like drawing a "health map" of the parathyroid glands to help doctors find potential lesions.
7. SPECT/CT salivary gland scintigraphy, explore the "image code" of salivary gland health, unlock the mystery of salivary glands, and protect the defense line of oral health. It can intuitively analyze the shape, location, function and whether the excretory passage is unobstructed and other conditions of the salivary glands, and help doctors determine whether the salivary glands are healthy and what kind of problems exist.
Department leader: Tao Xuemei
Title: Associate Chief Physician
Specialty: Thyroid diseases, various radionuclide therapies
Location: Room 223, Second Floor, General Hospital Outpatient Department; Room 212, Heavy Ion Hospital Outpatient Department.
