Hospital MDT Demonstrates Advantages: Personalized Approaches Overcome Clinical Challenges
Colorectal cancer, one of the most common malignancies in the gastrointestinal tract, often develops silently with minimal early symptoms. As the tumor grows, patients may experience changes in bowel habits, blood in stool, diarrhea, alternating diarrhea and constipation, and localized abdominal pain. In advanced stages, systemic symptoms such as anemia and unintended weight loss may appear.
Ranked among the top digestive system cancers in terms of incidence and mortality (following gastric, esophageal, and primary liver cancers), colorectal cancer is highly treatable when detected early. The primary treatment is surgical removal of the tumor, supported by a combination of chemotherapy, radiation therapy, immunotherapy, and traditional Chinese medicine to improve outcomes and quality of life.
Our Hospital’s Abdominal Surgery Team: Expertise and Innovation in Patient Care
The Abdominal Surgery Team at our hospital is a newly established discipline led by Dr. Li Shigong, former Director of Hepatobiliary and Pancreatic Surgery, alongside a group of talented young specialists from the former Hepatobiliary, Pancreatic, and Gastrointestinal Surgery departments. With extensive experience and comprehensive technical expertise, the team excels in both traditional and minimally invasive surgeries, including laparoscopic and robotic procedures. They are also highly skilled in complex multi-organ resection surgeries within the abdominal region.
Guided by medical standards while embracing personalized treatment approaches, the team consistently achieves satisfactory outcomes for patients. Recently, through meticulous preparation and exceptional surgical skills, The Abdominal Surgery Team successfully developed integrated and individualized treatment plans for several challenging cases, earning high praise and recognition from patients.
 | Case 1: Individualized Laparoscopic Sphincter-Preserving Surgery for Low Rectal Cancer The patient, Ms. Mou XX, a 65-year-old female, presented with a rectal lesion located 4 cm from the anal verge. Colonoscopy identified a 2-4 cm ulcerative lesion in the lower rectum. CT imaging revealed thickening of the rectal wall with a mass extending beyond the serosal layer, while MRI demonstrated heterogeneous thickening of the lower rectal wall and several small perirectal lymph nodes. The clinical staging was cT4aN1M0. According to standard rectal cancer treatment guidelines, the patient required neoadjuvant therapy followed by surgical intervention. However, due to personal psychological factors, the patient refused chemotherapy and strongly opposed the idea of a colostomy. She also insisted on sphincter preservation. With the rapid advancements in surgical techniques and medical equipment, it is now feasible to achieve safe tumor resection margins while preserving the anal sphincter, even for tumors located 4 cm from the anal verge. After thorough multidisciplinary discussion, our Abdominal Surgery Team concluded that, although the patient’s clinical stage did not align with the principle of immediate resection, an individualized treatment plan could be offered based on her specific needs. The team decided to perform a laparoscopic low anterior resection with sphincter preservation, without prophylactic colostomy. Postoperatively, the patient received meticulous care and demonstrated excellent compliance with the treatment regimen. She achieved complete recovery and was discharged without complications, resulting in high satisfaction for both the medical team and the patient. |
|---|---|
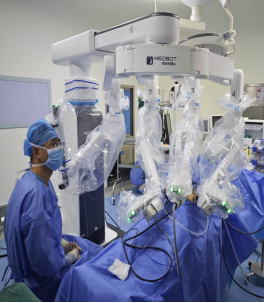 | Case 2: The patient, Mr. Gao, an 82-year-old male with colon cancer located in the descending colon. Colonoscopy revealed a 5-8 cm ulcerative lesion in the middle to lower segment of the descending colon. CT scan showed thickening of the rectal wall with mass formation, which had invaded through the serosal layer. Given the patient's advanced age, weakened physical condition, and comorbidities including mild pulmonary hypertension and chronic bronchitis, our department organized a multidisciplinary team (MDT) meeting involving the entire hospital. After thorough preoperative examinations, a detailed treatment and surgical plan was formulated. The cardiology, respiratory, and anesthesiology departments conducted repeated consultations to manage the comorbidities, ensuring the smooth implementation of the surgery. The abdominal surgery team successfully performed a laparoscopic left hemicolectomy. The entire procedure was completed without complications, and the patient recovered well postoperatively, demonstrating the strong advantages of multidisciplinary collaboration in our hospital. |
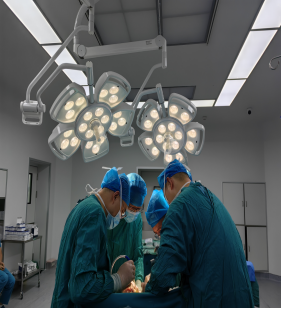 | Patient Profile: The patient, Mr. Li XX, a 68-year-old male, presented with a 3-5 cm ulcerative lesion in the mid-to-lower rectum as identified by colonoscopy. CT imaging revealed thickening of the rectal wall with a mass extending beyond the serosal layer, while MRI showed heterogeneous thickening of the mid-to-lower rectal wall and several small perirectal lymph nodes. The clinical staging was cT4aN1M0. Notably, the patient was highly obese, with a BMI of 33.5, and had a narrow pelvis, which posed significant challenges for laparoscopic rectal surgery. Surgical Challenges and Approach: Given the patient’s anatomical constraints and obesity, the surgical team faced considerable difficulties in achieving adequate exposure during the procedure. Despite these challenges, the Abdominal Surgery Team demonstrated exceptional precision and patience, successfully performing a laparoscopic radical resection for rectal cancer while preserving the anal sphincter. Outcome: Postoperatively, the patient received meticulous care and achieved primary wound healing. He recovered well and was discharged without complications, marking another successful case of individualized surgical management under complex conditions. |
 | Case 4: The patient, Mr. Wang, is a 70-year-old male who underwent a colonoscopy revealing a 5-7 cm elevated lesion in the mid-ascending colon. CT imaging demonstrated wall thickening and mass formation in the ascending colon, with a clinical staging of cT4bN2M0, indicating an advanced stage. The abdominal surgery team at our hospital conducted a multidisciplinary team (MDT) consultation and discussion, formulating a preoperative conversion therapy using the XELOX regimen for two cycles. The chemotherapy response and staging were reassessed to determine the subsequent treatment strategy. Through precise conversion therapy, the lesion significantly reduced in size, and the staging was downgraded to CT3N1M0. Following this, a laparoscopic radical right hemicolectomy was successfully performed. |
Medical associations and anti-cancer societies periodically revise the guidelines for the diagnosis and treatment of colorectal cancer to guide clinical specialists in providing standardized care. However, considering the varying needs of patients with the same disease, it is essential to integrate medical science with humanistic care. Clinicians should develop individualized treatment plans for patients, tailoring different approaches for the same disease based on individual circumstances. This is a critical aspect that must be carefully considered.
Diagnosis and Treatment Scope of Abdominal Surgery:
1.Liver cancer, hepatic hemangioma, liver abscess, and other benign and malignant liver diseases.
2.Gallstones, common bile duct stones, and cholangiocarcinoma.
3.Acute pancreatitis, pancreatic pseudocysts, pancreatic neuroendocrine tumors, pancreatic cystadenocarcinoma, and pancreatic cancer.
4.Liver cirrhosis with splenomegaly, hypersplenism, etc.
5.Colon polyps, adenomas, and colon cancer; rectal polyps, adenomas, and rectal cancer; gastric polyps, gastric ulcers, and gastric cancer.
6.Intestinal obstruction, hernia, appendicitis, anal fistula, anal fissure, and internal/external hemorrhoids.
Department's Expertise in Surgeries:
Minimally invasive laparoscopic and robotic surgeries for colon cancer, rectal cancer, and low rectal cancer, as well as gastric cancer.
Combined laparoscopic and choledochoscopic minimally invasive surgery for gallstones and common bile duct stones.
Radiofrequency ablation for liver tumors, traditional open liver tumor resection, and minimally invasive laparoscopic and robotic liver tumor resection.
Traditional open surgery, laparoscopic, and robotic pancreaticoduodenectomy for bile duct tumors, duodenal tumors, and pancreatic tumors, as well as duodenum-preserving pancreatic head resection.
Portoazygous devascularization for liver cirrhosis with splenomegaly and hypersplenism, and splenectomy for splenic rupture.
Laparoscopic hernia repair and appendectomy.
PPH (Procedure for Prolapse and Hemorrhoids) surgery for anal fistula, anal fissure, and internal/external hemorrhoids.
 |  |  |
| Li Shigong Tel:15025957869 | Tao Jichun Tel:13830539708 | Sun Yanfeng Tel:13884554011 |
