No Surgery, Less Pain | Heavy Ions: A "Precision Blast" Against Tumors
No Surgery, Less Pain | Heavy Ions: A "Precision Blast" Against Tumors
Introduction:
Conventional radiotherapy may affect both the tumor and surrounding normal tissues. Heavy ion therapy acts like a precisely targeted ray, concentrating energy upon reaching the lesion area and accurately targeting the tumor region. This helps better protect normal organs and tissues, improving quality of life during treatment.
I. Heavy Ion Therapy: Why Is It Hailed as a "Precision-Guided Weapon"?
Its precision and power come from two key "weapons":
1. Physical Precision: The "Bragg Peak" Effect
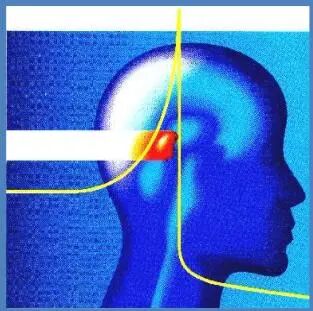
When a heavy ion beam (such as carbon ions) penetrates the human body, its energy release is highly "intelligent." Before reaching the tumor target area, it releases very little energy, like a secret agent infiltrating enemy territory. Once it reaches the preset depth of the tumor, the energy is released instantly and intensively, forming an extremely high dose peak (the Bragg peak), after which the dose drops off rapidly. This means that almost all the energy is deposited directly into the tumor, with minimal damage to normal tissues along the path and behind the tumor.
2. Biological Precision: Stronger "Elimination" Capability
Heavy ion beams cause irreversible "double-strand breaks" to the DNA of tumor cells, with a biological effectiveness 2–3 times higher than that of conventional photon radiotherapy. Especially for tumors that are resistant to conventional radiotherapy (such as chordoma, chondrosarcoma, some types of pancreatic cancer, and liver cancer), heavy ion therapy often demonstrates better treatment outcomes.
II. Pre-battle Deployment: Precision Strike Starts With Meticulous Preparation Down To The Smallest Detail
To achieve a perfect "sniper strike," meticulous pre-treatment preparation is crucial. This is not only the task of the doctors but also requires close cooperation from the patient.
Step 1: Creating a "Custom Mold" – Ensuring Absolutely Still Positioning During Treatment
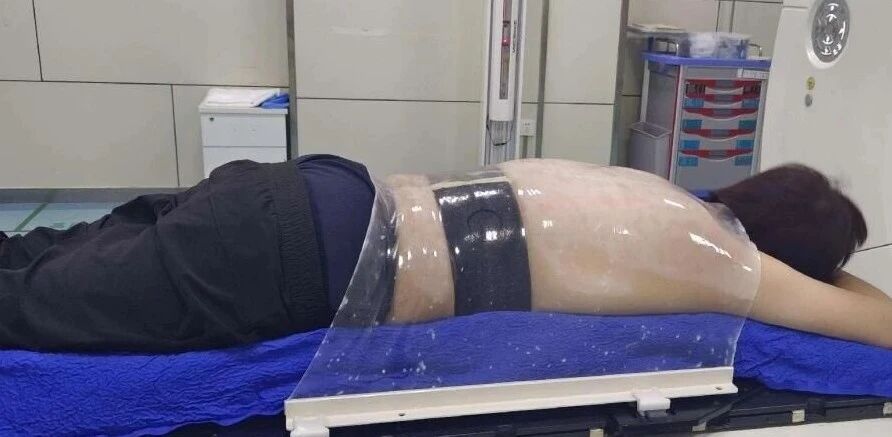
During treatment, the machine will emit the ion beam strictly according to the treatment plan. Any slight movement may cause the "bullet" to miss its target. Therefore, a personalized immobilization device (such as a vacuum cushion or thermoplastic mask) must be custom-made for each patient.
Considerations: Immobilization must take into account the beam angle during treatment, how to avoid vital organs (such as the spinal cord and intestines), and whether special preparations are required (such as fasting, moderate bladder filling, use of an abdominal belt, or respiratory gating techniques to control tumor movement associated with breathing).
Step 2: Comprehensive Reconnaissance – Clarify the "enemy situation" (tumor information)
Imaging Reconnaissance (Identifying Location and Activity):
- MRI (Magnetic Resonance Imaging): The "structural scout." Clearly displays the relationship between the tumor and critical tissues such as nerves and blood vessels.
- CT (Computed Tomography): Provides a "3D map" of the human body and serves as the core anatomical basis for radiotherapy planning.
- PET-CT (Functional Metabolic Imaging): Not only a "locator" but also an "activity detector." Identifies tumor regions with abnormally high metabolic activity as well as potential metastatic lesions.
Pathological Reconnaissance (Identifying the Enemy): Through biopsy, the type and grade of the tumor are confirmed under a microscope. This is the ultimate basis for determining whether a patient is suitable for heavy ion therapy.
General Health Assessment (Ensuring Our Combat Capability): Includes blood tests (complete blood count), liver and kidney function tests, cardiopulmonary function tests, and other evaluations to comprehensively assess whether the patient's body can safely tolerate the treatment.
Step 3: Precise Calibration – Complete the deduction of the "Digital Sand Table"
After all the necessary examinations and imaging scans have been completed, the imaging data will be imported into the treatment planning system, where the following steps will be carried out:
- Target Delineation: The physician accurately outlines the tumor area to be irradiated and the subclinical regions requiring prophylactic irradiation.
- Plan Design: The physicist, acting like a military strategist, determines the beam angle, energy, and intensity, and generates an optimal irradiation plan on the computer that adequately covers the tumor while protecting the surrounding normal tissues.
- Plan Verification: After the treatment plan has been created and approved by the physician, the physicist first performs dose verification for the plan. Once the plan has passed verification, it is handed over to the technical team for treatment delivery.
III. Pre-battle Calibration: The Final "Quality Inspection" Before Treatment
From simulation to the start of formal treatment, several days may pass. To ensure that everything is perfectly aligned, a crucial "repositioning" step must be performed before the first treatment session.
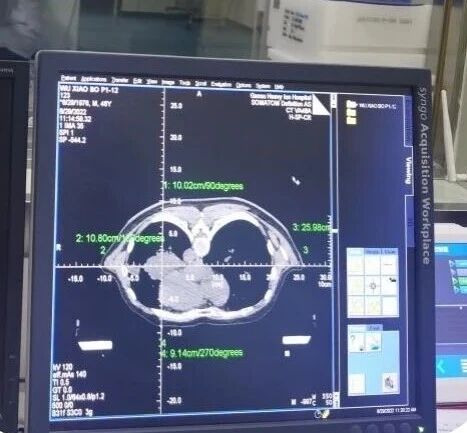
Process: The patient lies again on the treatment couch, using the same immobilization device. The physician and physicist compare the digital coordinates from the treatment plan with the actual markers on the patient's body, making micrometer-level fine adjustments using the laser positioning system. Imaging is then used to confirm that the tumor position exactly matches the target area in the plan. Once repositioning is confirmed to be accurate, the patient is ready to enter the treatment room and receive the heavy ion irradiation—like an "invisible surgery."

Summary and Outlook
Heavy ion therapy is a modern radiotherapy technology that integrates cutting-edge physics, biomedical science, and precision engineering. From evaluation, immobilization, and planning to calibration, the entire process is centered on precision. Under the assessment of professional physicians and standardized procedures, it provides cancer patients with a more targeted local treatment option.
