Hyperthermic Intraperitoneal Chemotherapy (HIPEC): Precision Hyperthermia in Cancer Treatment
Hyperthermic Intraperitoneal Chemotherapy (HIPEC): Precision Hyperthermia in Cancer Treatment
What is HIPEC?
Hyperthermic Intraperitoneal Chemotherapy (HIPEC) is a localized treatment technique that combines high temperature with chemotherapy drugs, specifically designed to treat intra‑abdominal tumors—particularly malignant tumors that have metastasized to the peritoneum.
In simple terms, after surgical removal of the tumor, the surgeon circulates a warm chemotherapy solution (approximately 41–43°C) throughout the abdominal cavity, allowing the fluid to thoroughly contact and rinse every corner of the peritoneal space. The procedure lasts 60–90 minutes, after which the fluid is drained.
This process is often colloquially called an “abdominal hot bath” or a “sauna for the abdomen”—except that it is the cancer cells being “soaked,” with the goal of eradicating any residual tumor.
Why Does Heat “Burn” Cancer Cells?
Normal human cells have a certain tolerance to heat, while cancer cells are particularly sensitive to high temperatures. The reasons include:

Research shows that at 41–43°C, hyperthermia combined with chemotherapy (e.g., cisplatin) can be 3–5 times more effective at killing cancer cells than chemotherapy alone.
How Is the Treatment Performed?
HIPEC is usually combined with Cytoreductive Surgery (CRS). The entire treatment consists of the following stages:

Which Patients Are Suitable for HIPEC?
HIPEC is primarily indicated for patients with malignant tumors that have spread to the peritoneum (peritoneal metastasis or peritoneal carcinomatosis). Common candidate populations include:

The key assessment tool for selecting HIPEC is the Peritoneal Cancer Index (PCI)—a scoring system (0–39) that quantifies the extent of peritoneal involvement. Generally, patients with a PCI ≤ 20 derive the greatest benefit from CRS + HIPEC.
How Effective Is It?
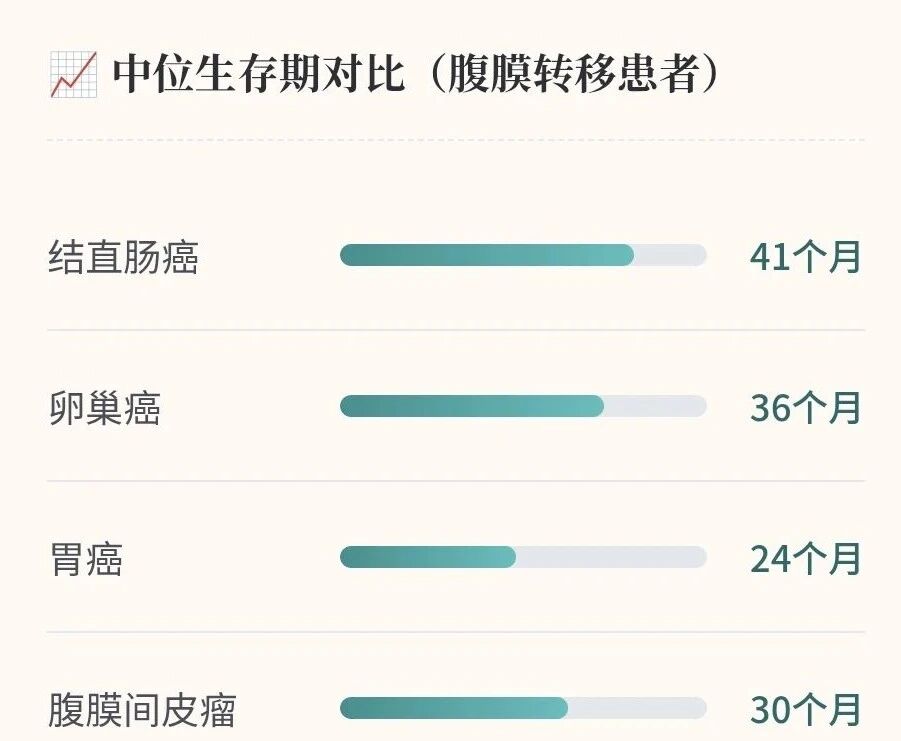
The following data from major clinical studies demonstrate the survival improvement of CRS + HIPEC compared with chemotherapy alone:

Risks and Considerations
HIPEC is a major surgical procedure that carries inherent risks, making thorough preoperative discussion essential.


Frequently Asked Questions (FAQs)
What preparations are needed before surgery?
Before surgery, the following preparations are typically required:
- Comprehensive imaging studies (contrast‑enhanced CT, MRI, or PET‑CT) to evaluate the extent of peritoneal metastasis.
- Cardiopulmonary function tests and blood chemistry tests.
- Bowel preparation (liquid diet for 3 days before surgery and fasting the night before).
- For malnourished patients, 1–2 weeks of preoperative nutritional support is often recommended to improve surgical tolerance.
How long does the surgery take, and what is the recovery period?
The combined CRS+HIPEC procedure usually lasts 6–12 hours, depending on the tumor extent and the organs requiring resection. After surgery, patients are typically monitored in the ICU for 1–2 days, followed by a hospital stay in a general ward for about 10–20 days. Full recovery to normal daily activities generally takes 1–3 months. Regular follow‑up is necessary after discharge, with imaging studies recommended every 3–6 months.
Can HIPEC be repeated?
In most cases, HIPEC is performed as a one‑time treatment concurrent with tumor‑removal surgery. Some centers may schedule 1–2 sessions of early postoperative intraperitoneal chemotherapy (EPIC) as adjuvant treatment after the initial surgery. If recurrence occurs and repeat surgery is considered, a second HIPEC may be an option, but this requires rigorous assessment of the patient’s overall health and tumor status.
Radiotherapy Department II (Lanzhou Campus)

As a specialized radiotherapy unit for gynecological oncology, Radiotherapy Department II (Lanzhou Campus) focuses exclusively on the radiation therapy of gynecological tumors. Equipped with advanced radiotherapy technology and a dedicated medical team, the department provides precise, standardized, and individualized comprehensive treatment for patients with gynecological cancers. The department actively conducts basic and clinical research related to gynecological radiotherapy and undertakes multiple scientific research projects. It also serves as a teaching and training base, cultivating professionals for the field. With a patient-centered philosophy and supported by cutting‑edge technology, the department is committed to improving the cure rate and quality of life of gynecological cancer patients, delivering high‑quality, efficient, and humanized medical services.
Professional Team
The department currently has 14 medical staff members, including 7 physicians and 7 nurses. It is a dynamic and knowledgeable professional team, comprising 2 senior‑title and 2 intermediate‑title specialists.
- Director Zhao Fengju, Chief Physician, has over 30 years of experience in radiotherapy and is a rare oncology expert in Northwest China. She serves as the Chair of the Gansu Anti‑Cancer Association Brachytherapy Committee and Vice‑Chair of the Northwest Gynecological Oncology and Brachytherapy Committee. She specializes in comprehensive treatment of gynecological tumors, including radiotherapy, chemotherapy, and immunotherapy/targeted therapy. She has introduced advanced external beam techniques such as carbon‑ion radiotherapy (CIRT) and image‑guided radiotherapy (IGRT) for gynecological cancers, as well as 3D brachytherapy, interstitial implantation, and painless afterloading therapy, with extensive clinical experience in oncology radiotherapy and chemotherapy.
- Chief Physician Du Lanning previously worked in radiotherapy at the First Hospital of Lanzhou University for over 40 years. She is proficient in radiotherapy and comprehensive treatment for various common malignant tumors, including head and neck cancer, lung cancer, gastrointestinal cancer, breast cancer, and urological tumors.
The department also benefits from technical and academic guidance by distinguished experts such as Professor Wang Junjie, Chair of the National Radiotherapy Committee, Director of the Radiotherapy Department at Peking University Third Hospital, and President of the Lanzhou Branch of Gansu Wuwei Cancer Hospital, as well as Professor Li Sha, Director of the Radiotherapy Department at the Army General Hospital.
Scope of Treatment
The department primarily provides carbon‑ion therapy, photon radiotherapy, and brachytherapy for gynecological malignancies (e.g., cervical cancer, endometrial cancer, ovarian cancer, vulvar cancer, vaginal cancer) as well as for lung cancer, gastrointestinal malignancies, urological tumors, and other cancers. It also offers comprehensive treatments including chemotherapy, targeted therapy, immunotherapy, and cellular immunotherapy for various malignant tumors.
