Integrated Pain Diagnosis and Treatment Center · Nine Featured Treatment Technologies (Part 3)
Integrated Pain Diagnosis and Treatment Center · Nine Featured Treatment Technologies (Part 3)
(7) Patient-Controlled Analgesia (PCA)
PCA serves as a complementary approach to conventional analgesic medication. It is used for opioid dose titration in cancer pain patients, management of frequent breakthrough pain, and continuous analgesia for patients with dysphagia, gastrointestinal dysfunction, or those receiving end‑of‑life care.
Advantages of PCA:
- Reduces side effects caused by excessive analgesic dosing.
- Enhances comfort and facilitates pain management.
- Enables on‑demand medication delivery for personalized analgesia.
- Effectively alleviates cancer pain and lowers the incidence of complications.

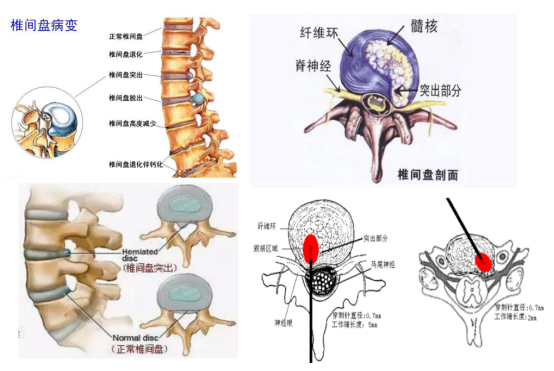
(8) Targeted Ablation for Herniated Discs: Collagenase, Ozone, and Plasma Treatments
“Targeted ablation” refers to the precise guidance of imaging equipment (e.g., DSA, CT) to insert a fine needle into or around the herniated disc. Specific agents are then injected to shrink, dissolve, atrophy, or inactivate the protruding nucleus pulposus through chemical or physical reactions, thereby relieving compression on nerve roots or the spinal cord.
These three techniques are all forms of “percutaneous minimally invasive interventional therapy.” Using a fine needle accurately placed into the affected disc, the herniated nucleus pulposus is reduced in volume and pressure via chemical (collagenase), physico‑chemical (ozone), or physical (plasma) means, ultimately relieving nerve compression.
Advantages of Targeted Ablation for Herniated Discs:
1.Minimally invasive and precise: Only a fine needle is used, guided by imaging to act accurately on the target lesion with minimal trauma.
2.Safe and function‑preserving: Avoids the major trauma and risks of general anesthesia associated with open surgery, preserving spinal structure and mobility to the greatest extent.
3.Quick recovery: Rapid postoperative recovery, short hospital stay, and a prompt return to normal life.
4.Stepwise option: Serves as an important minimally invasive step between conservative care and open surgery; even if outcomes are suboptimal, it does not preclude other subsequent treatments.
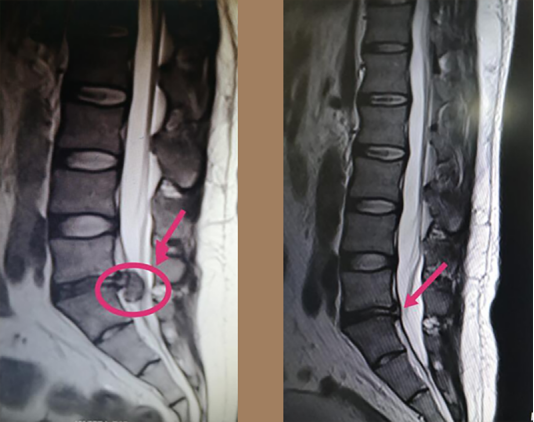
Pre- and post-treatment imaging comparison
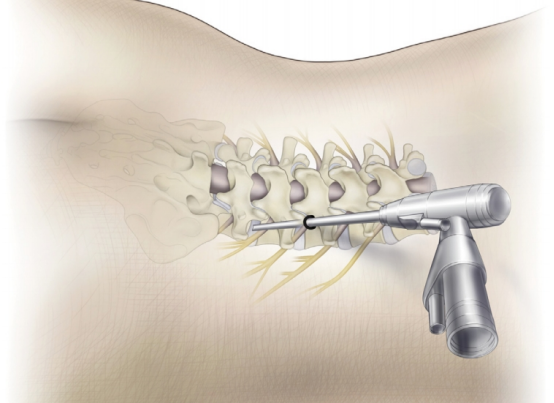
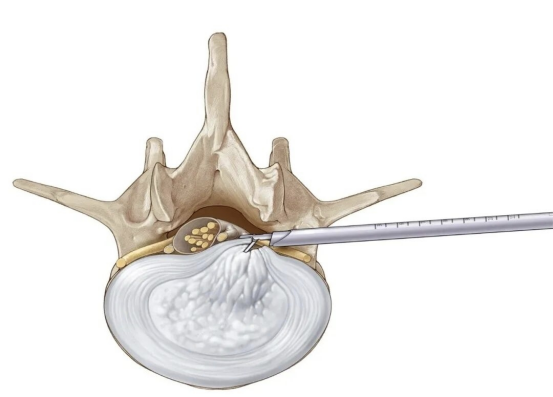
(9) Spinal Endoscopy Technology
Spinal endoscopy is a revolutionary minimally invasive spinal surgery. In essence, it involves inserting a slender tube equipped with a high‑definition camera through a “keyhole” incision of about 1 cm. The physician views a magnified screen and uses micro‑instruments to precisely address spinal pathologies (such as herniated discs or hypertrophic ligaments), relieving nerve compression. Simply put, it is like performing a precise repair inside the spine using an “endoscope” and “micro‑tools,” thereby avoiding the trauma of traditional open surgery.
Three Key Advantages of Spinal Endoscopy:
1.Minimally invasive: Very small incision (approx. 7–8 mm), no extensive muscle dissection, preserving spinal stability.
2.Precise: The endoscopic lens magnifies the surgical field, allowing finer and safer manipulation.
3.Fast recovery: Minimal bleeding, mild pain; patients can typically stand or walk on the same or next day, with short hospital stays (1–3 days).
4.Modern spinal surgery advocates a “step‑by‑step treatment” philosophy:
5.First step: Conservative treatment (rest, medication, rehabilitation/physical therapy) – the majority of patients (>80%) recover or improve at this stage.
6.Second step: Minimally invasive interventional therapy (e.g., collagenase/ozone ablation, radiofrequency, plasma, endoscopic discectomy) – suitable for specific types of herniation unresponsive to conservative care.
7.Third step: Open surgery (e.g., discectomy, laminectomy, fusion with internal fixation) – reserved for severe cases, failed minimally invasive treatments, or patients with clear surgical indications.
Introduction to the Pain Medicine Department
Our hospital’s Pain Medicine Department is comprised of a pain outpatient clinic, a cancer pain multidisciplinary team (MDT) clinic, a pain treatment room, and an inpatient pain ward. We specialize in managing a wide range of acute and chronic pain conditions, cancer-related pain, and intractable pain.
The department offers advanced interventional therapies for cancer pain, including:
- Intrathecal analgesic pump implantation
- Neuromodulation with spinal cord or peripheral nerve stimulation
- Celiac plexus neurolysis
- Radiofrequency neuromodulation
- Vertebroplasty for metastatic spinal lesions
- Building on the hospital’s long-standing tradition of patient‑centered care and extensive multidisciplinary experience, we are dedicated to alleviating your pain and committed to supporting your journey toward a pain‑free life.
