How Drug-Eluting Microspheres Are Reshaping the Anti-Cancer Battlefield
Drug-Eluting Microspheres: A Precision Revolution in Targeted Liver Cancer
Liver Cancer: The "King of Cancers". In China, a country with a high incidence of liver cancer, about 80% of patients are diagnosed at intermediate or advanced stages, surgery becomes infeasible. While Transarterial Chemoembolization (TACE) remains the first-line treatment, it has limitations such as widespread drug diffusion, incomplete embolization, and high recurrence rates. Now, the emergence of drug-eluting bead TACE (DEB-TACE) technology offers a more precise and effective interventional treatment option for patients with advanced primary liver cancer or metastatic liver cancer.
Technological Breakthrough: The Three Core Advantages of Drug-loaded Microspheres
1. Precise Embolization & Sustained Drug Release
Drug-eluting microspheres, made of polyvinyl alcohol (PVA) or other polymer materials, can precisely embolize tumor-feeding arteries, cutting off nutrient supply to "starve" the tumor. Meanwhile, the microspheres load chemotherapy drugs (e.g., doxorubicin, pirarubicin) via ionic adsorption, enabling localized sustained release for up to one month. This elevates intratumoral drug concentration to 100-400 times higher than systemic levels, significantly enhancing anticancer efficacy.
2. Reduced Systemic Toxicity
While traditional TACE uses lipiodol (which easily washes away in blood flow, allowing drugs to enter systemic circulation), drug-eluting microspheres lower peripheral blood drug concentration by over 50% through localized sustained release. This dramatically reduces systemic side effects such as nausea and myelosuppression.
3. Broad Applicability & Strong Potential for Combination Therapy
Unlike conventional methods, drug-eluting microspheres remain effective even for hypovascular lesions. Clinical studies show they can be combined with hepatic arterial infusion chemotherapy (HAIC), targeted therapy, and immunotherapy, forming a "local + systemic" comprehensive treatment strategy. This approach is particularly suitable for complex cases like massive hepatocellular carcinoma and portal vein tumor thrombosis (PVTT).
Clinical Data: Significantly Improved Survival Benefits
Survival Rate Breakthrough: Meta-analysis reveals that DEB-TACE patients achieved 12%, 24%, and 69% higher 1-year, 2-year, and 3-year overall survival rates respectively compared to conventional TACE, with median survival extended to 31.8 months.
Higher Tumor Response Rate: Studies demonstrate that the drug-eluting microsphere treatment group reached 52.5% complete response (CR) rate and 90% overall response rate, significantly outperforming conventional therapy's 72.5%.
Enhanced Safety Profile: The incidence of post-embolization syndrome (e.g., fever, pain) was reduced, while severe complications (e.g., liver abscess) remained controllable, resulting in better patient tolerance.
Domestic Innovation: VisPearl® Microspheres Lead Technological Advancement
The independently developed VisPearl® drug-loaded microspheres from China optimize particle size (40-90μm) and drug-loading efficiency to precisely match different vascular branches. Smaller microspheres (100-300μm) penetrate deeper into tumor peripheries for thorough embolization, while larger ones (300-500μm) target proximal vessels in massive hepatocellular carcinoma, significantly improving complete necrosis rates.
Real-World Case: A Journey from Despair to Renewed Hope
Case 1: A 61-year-old male with recurrent hepatocellular carcinoma post-surgery and carbon ion therapy. Abdominal MRI revealed: A treated space-occupying lesion in the left hepatic lobe (4.3×4.8 cm, S2501, I19), showing slight enlargement with irregular margins and marked enhancement
Newly developed adjacent intrahepatic bile duct dilation and left portal vein thrombosis
New subcapsular enhancing nodule in the left lobe (suspected metastasis)
After drug-eluting microsphere embolization, the target lesion achieved complete necrosis.
Case 2: Successful Conversion Therapy in 68-Year-Old HCC Patient (8cm Tumor) with DEB-TACE
A 68-year-old patient with primary hepatocellular carcinoma (8cm lesion) achieved complete tumor devascularization and preserved liver function following DEB-TACE treatment, creating optimal conditions for subsequent conversion surgery.
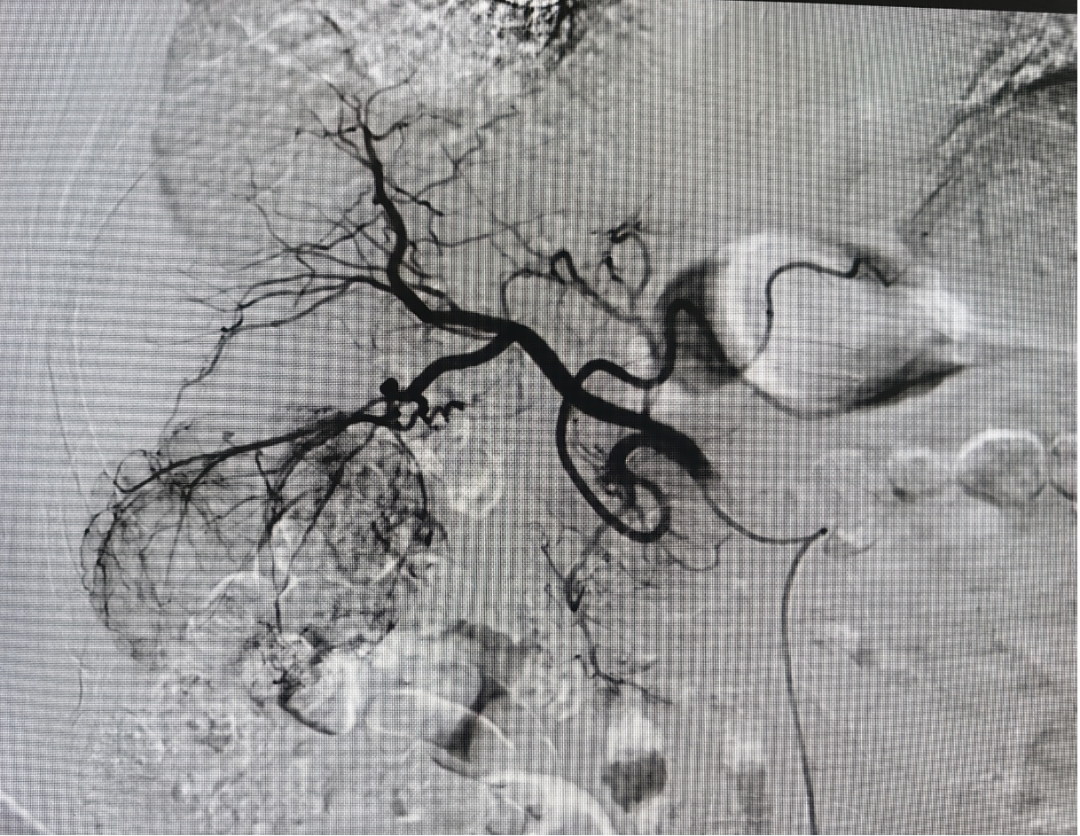

Preoperative Postoperative
Future Perspectives: The Dawn of Personalized Therapy
Drug-eluting microsphere technology is advancing toward greater precision:
Personalized Particle Size Selection: Tailor embolization strategies based on tumor size and vascular characteristics—small particles for lesions <3cm, large particles for tumors >5cm.
Combination Therapy Expansion: Synergizing with immune checkpoint inhibitors and anti-angiogenic drugs shows potential to break through treatment barriers in advanced HCC.
Indication Extension: Exploring applications in other solid tumors (e.g., lung cancer, renal carcinoma) to benefit broader patient populations.
Drug-loaded microsphere technology, with its "minimally invasive, precise, and sustained-release" advantages, has redefined the gold standard for liver cancer intervention. Whether prolonging survival or enhancing quality of life, it brings a dawn of hope to patients with intermediate and advanced-stage disease. Choosing drug-eluting microspheres is not just selecting a treatment—it's embracing the courage and hope to coexist with cancer!

Director Yang Wangsheng
Minimally invasive surgeries focused on in the Department of Cardiology and Interventional include:
(I) Cardiac and Major Vascular Interventions:
1. Congenital Heart Disease: Catheter-based closure for atrial septal defect (ASD) / ventricular septal defect (VSD) / patent ductus arteriosus (PDA), Coronary artery disease (CAD) interventions (PCI), Pacemaker implantation for bradyarrhythmias, Radiofrequency ablation for tachyarrhythmias.
2. Aortic Diseases: Endovascular stent-graft exclusion for: Aortic dissection / aortic aneurysm, Abdominal aortic aneurysm ; Stent placement for: Aortic ulcer, Intramural aortic hematoma.
(II) Minimally Invasive Peripheral Vascular Procedures:
- Balloon angioplasty and stenting for lower extremity arteriosclerosis obliterans
- Balloon angioplasty and stenting for renal artery stenosis
- Subclavian artery stenting
- Thrombolysis and thrombectomy for lower extremity deep vein thrombosis
- Inferior vena cava filter placement and retrieval
- Radiofrequency ablation and foam sclerotherapy for varicose veins
- Surgical thrombectomy and thrombolysis for acute arterial embolism
- Thrombus aspiration and catheter-directed thrombolysis for acute pulmonary embolism
- Embolization therapy for visceral artery aneurysms
(III) Minimally Invasive Oncology and Other Specialized Procedures:
- Interventional Embolization for massive hemorrhage (respiratory, gastrointestinal, and gynecological)
- Tumor Embolization Therapy for benign/malignant solid tumors (hepatocellular carcinoma, hepatic hemangioma, uterine fibroids, cervical cancer, soft tissue tumors, etc.)
- Transarterial Chemotherapy Infusion for advanced-stage malignancies
- Interventional Diagnosis & Treatment of arterial/venous hemangiomas
- Port Catheter Implantation & Removal for oncology patients
- Address: Building 1, Ground Floor, Wuwei Heavy Ion Center, Gansu Wuwei Cancer Hospital.
